Exploring the bi-directional relationship between periodontitis and dyslipidemia: a comprehensive systematic review and meta-analysis
- PMID: 38684998
- PMCID: PMC11059608
- DOI: 10.1186/s12903-023-03668-7
Exploring the bi-directional relationship between periodontitis and dyslipidemia: a comprehensive systematic review and meta-analysis
Abstract
Aim: As periodontitis and dyslipidemia are diseases that occur with high incidence, the relationship between them has attracted much attention. Previous studies on these diseases have tended to focus on lipid parameters and periodontitis, we aimed to investigate the relationship between dyslipidemia and periodontitis.
Materials and methods: A comprehensive search to identify the studies investigating the relationship between dyslipidemia and periodontitis was performed on PubMed, Web of Science and Cochrane Library before the date of August, 2023. Studies were considered eligible if they contained data on abnormal blood lipid parameters and periodontitis. Studies that reported mean differences and 95% confidence intervals or odds ratios were used.
Results: A total of 73 publications were included in the meta-analysis. Hyper total cholesterol (TC), triglycerides (TGs), low-density lipoprotein (LDL), very low-density lipoprotein (VLDL) and lower high-density lipoprotein (HDL) levels are risk factors for periodontitis. Periodontal disease is a risk factor for high TG and low HDL levels. Three months after periodontal treatment, the levels of TC, TG and HDL were significantly improved, and statin treatment only improved gingival index (GI) levels compared to that of the dietary control.
Conclusions: The findings reported here suggest that the mutual promotion of periodontitis and dyslipidemia can be confirmed. Non-surgical periodontal therapy may improve lipid abnormalities. It can't be demonstrated whether systematic application of statins have a better effect on the improvement in periodontal status in patients with dyslipidemia compared to that of the control.
Keywords: Blood lipid treatment; Dyslipidemia; Meta-analysis; Periodontal treatment; Periodontitis.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures



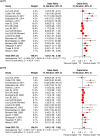






Similar articles
-
Relationship between periodontal status and dyslipidemia in patients with type 2 diabetic nephropathy and chronic periodontitis: A cross-sectional study.J Periodontal Res. 2022 Oct;57(5):969-976. doi: 10.1111/jre.13033. Epub 2022 Jul 18. J Periodontal Res. 2022. PMID: 35848007
-
Heat-shock protein 60 kDa and atherogenic dyslipidemia in patients with untreated mild periodontitis: a pilot study.Cell Stress Chaperones. 2012 May;17(3):399-407. doi: 10.1007/s12192-011-0315-1. Epub 2012 Jan 4. Cell Stress Chaperones. 2012. PMID: 22215516 Free PMC article.
-
Mixed dyslipidemia among patients using lipid-lowering therapy in French general practice: an observational study.Clin Ther. 2007 Aug;29(8):1671-81. doi: 10.1016/j.clinthera.2007.08.003. Clin Ther. 2007. PMID: 17919548
-
Pitavastatin: novel effects on lipid parameters.Atheroscler Suppl. 2011 Nov;12(3):277-84. doi: 10.1016/S1567-5688(11)70887-X. Atheroscler Suppl. 2011. PMID: 22152282 Review.
-
Targeting dyslipidemia by herbal medicines: A systematic review of meta-analyses.J Ethnopharmacol. 2021 Nov 15;280:114407. doi: 10.1016/j.jep.2021.114407. Epub 2021 Jul 9. J Ethnopharmacol. 2021. PMID: 34252530
Cited by
-
Acceleration of HDL-Mediated Cholesterol Efflux Alleviates Periodontitis.J Dent Res. 2024 Oct;103(11):1109-1118. doi: 10.1177/00220345241271075. Epub 2024 Sep 23. J Dent Res. 2024. PMID: 39311443
-
A Roadmap for the Rational Use of Biomarkers in Oral Disease Screening.Biomolecules. 2024 Jul 1;14(7):787. doi: 10.3390/biom14070787. Biomolecules. 2024. PMID: 39062501 Free PMC article. Review.
-
Association between periodontitis and blood lipid levels: a cross-sectional study.BMC Oral Health. 2025 Jul 2;25(1):1055. doi: 10.1186/s12903-025-06341-3. BMC Oral Health. 2025. PMID: 40604728 Free PMC article.
-
Role of fatty acid metabolism-related genes in periodontitis based on machine learning and bioinformatics analysis.Hua Xi Kou Qiang Yi Xue Za Zhi. 2024 Dec 1;42(6):735-747. doi: 10.7518/hxkq.2024.2024214. Hua Xi Kou Qiang Yi Xue Za Zhi. 2024. PMID: 39610070 Free PMC article. Chinese, English.
-
Association between periodontal disease and systemic diseases: a cross-sectional analysis of current evidence.Mil Med Res. 2024 Dec 4;11(1):74. doi: 10.1186/s40779-024-00583-y. Mil Med Res. 2024. PMID: 39633497 Free PMC article.
References
-
- GBD 2017 Oral Disorders Collaborators. Bernabe E, Marcenes W, Hernandez CR, Bailey J, Abreu LG, Alipour V, Amini S, Arabloo J, Arefi Z, Arora A, Ayanore MA, Bärnighausen TW, Bijani A, Cho DY, Chu DT, Crowe CS, Demoz GT, Demsie DG, Dibaji Forooshani ZS, et al. Global, regional, and National Levels and trends in burden of Oral conditions from 1990 to 2017: A systematic analysis for the global burden of disease 2017 study. J Dent Res. 2020;99(4):362–373. doi: 10.1177/0022034520908533. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

