Individual-Level Digital Determinants of Health and Technology Acceptance of Patient Portals: Cross-Sectional Assessment
- PMID: 38695754
- PMCID: PMC11196914
- DOI: 10.2196/56493
Individual-Level Digital Determinants of Health and Technology Acceptance of Patient Portals: Cross-Sectional Assessment
Abstract
Background: Digital determinants of health (DDoH), including access to technological tools and digital health literacy, function independently as barriers to health. Assessment for DDoH is not routine within most health care systems, although addressing DDoH could help mitigate differential health outcomes and the digital divide.
Objective: This study aims to assess the role of individual-level DDoH factors on patient enrollment in and use of the patient portal.
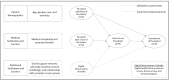
Methods: We developed a multimodal, cross-sectional survey and deployed it to 11,424 individuals based on their preferred mode and language documented within the electronic medical record. Based on the Technology Acceptance Model, enrollment in and intent to use the patient portal were the outcomes of interest. Perceived usefulness and ease of use were assessed to determine construct validity, and exploratory investigations included individual-level DDoH, including internet and device access, availability of technological support, medical complexity, individual relationship with the health care system, and digital health literacy. Counts (n) and proportions (%) were used to describe response categories, and adjusted and unadjusted odds ratios are reported.
Results: This study included 1850 respondents (11,424 invited, 16.2% response rate), who were mostly female (1048/1850, 56.6%) and White (1240/1850, 67%), with an average age of 63 years. In the validation of the Technology Acceptance Model, measures of perceived ease of use (ie, using the patient portal will require a lot of mental effort; the patient portal will be very easy to use) and perceived usefulness (ie, the usefulness of the patient portal to send and receive messages with providers, schedule appointments, and refill medications) were positively associated with both enrollment in and intent to use the patient portal. Within adjusted models, perceived ease of use and perceived usefulness constructs, in addition to constructs of digital health literacy, knowing what health resources are available on the internet (adjusted odds ratio [aOR] 3.5, 95% CI 1.8-6.6), portal ease of use (aOR 2.8, 95% CI 1.6-5), and portal usefulness (aOR 2.4, 95% CI 1.4-4.2) were significantly associated with patient portal enrollment. Other factors associated with patient portal enrollment and intent to use included being comfortable reading and speaking English, reported use of the internet to surf the web or to send or receive emails, home internet access, and access to technology devices (computer, tablet, smartphone, etc).
Conclusions: Assessing for and addressing individual-level DDoH, including digital health literacy, access to digital tools and technologies, and support of the relational aspects between patients, social support systems, and health care providers, could help mitigate disparities in health. By focusing efforts to assess for and address individual-level DDoH, an opportunity exists to improve digitally driven health care delivery outcomes like access and structural outcomes like bias built within algorithms created with incomplete representation across communities.
Keywords: digital determinants of health; digital health; digital health literacy; digital inclusion; eHealth; electronic health records; mobile phone; patient portals; technology acceptance model.
©Lindsey M Philpot, Priya Ramar, Daniel L Roellinger, Jane W Njeru, Jon O Ebbert. Originally published in JMIR Formative Research (https://formative.jmir.org), 10.06.2024.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures


References
-
- Chunara R, Zhao Y, Chen J, Lawrence K, Testa PA, Nov O, Mann DM. Telemedicine and healthcare disparities: a cohort study in a large healthcare system in New York City during COVID-19. J Am Med Inform Assoc. 2021;28(1):33–41. doi: 10.1093/jamia/ocaa217. https://europepmc.org/abstract/MED/32866264 5899729 - DOI - PMC - PubMed
-
- Richwine C. Progress and persistent disparities in patient access to electronic health information. JAMA Health Forum. 2023;4(11):e233883. doi: 10.1001/jamahealthforum.2023.3883. https://europepmc.org/abstract/MED/37948063 2811770 - DOI - PMC - PubMed
-
- Brands MR, Gouw SC, Beestrum M, Cronin RM, Fijnvandraat K, Badawy SM. Patient-centered digital health records and their effects on health outcomes: systematic review. J Med Internet Res. 2022;24(12):e43086. doi: 10.2196/43086. https://www.jmir.org/2022/12/e43086/ v24i12e43086 - DOI - PMC - PubMed
-
- Lawrence K. In: Digital Health Equity. Linwood SL, editor. Brisbane (AU): Exon Publications; 2022. - PubMed
LinkOut - more resources
Full Text Sources

