A detailed review of the spinal accessory nerve and its anatomical variations with cadaveric illustration
- PMID: 38696101
- PMCID: PMC11143051
- DOI: 10.1007/s12565-024-00770-w
A detailed review of the spinal accessory nerve and its anatomical variations with cadaveric illustration
Abstract
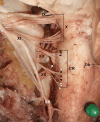
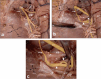
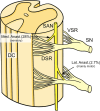
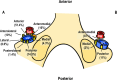
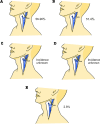
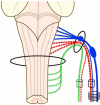
The spinal accessory nerve, considered part of the eleventh cranial nerve, provides motor innervation to sternocleidomastoid and trapezius. A comprehensive literature review and two cadaveric dissections were undertaken. The spinal accessory nerve originates from the spinal accessory nucleus. Its rootlets unite and ascend between the denticulate ligament and dorsal spinal rootlets. Thereafter, it can anastomose with spinal roots, such as the McKenzie branch, and/or cranial roots. The spinal accessory nerve courses intracranially via foramen magnum and exits via jugular foramen, within which it usually lies anteriorly. Extracranially, it usually crosses anterior to the internal jugular vein and lies lateral to internal jugular vein deep to posterior belly of digastric. The spinal accessory nerve innervates sternocleidomastoid, receives numerous contributions in the posterior triangle and terminates within trapezius. Its posterior triangle course approximates a perpendicular bisection of the mastoid-mandibular angle line. The spinal accessory nerve contains sensory nociceptive fibres. Its cranial nerve classification is debated due to occasional non-fusion with the cranial root. Surgeons should familiarize themselves with the variable course of the spinal accessory nerve to minimize risk of injury. Patients with spinal accessory nerve injuries might require specialist pain management.
Keywords: Accessory; Classification; Course; Nerve; Variation.
© 2024. Crown.
Conflict of interest statement
The authors declare that they have no conflict of interest. All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript. All cadaveric subjects had provided informed consent and anonymity was preserved at all times. The authors hereby confirm that every effort was made to comply with all local and international ethical guidelines and laws concerning the use of human cadaveric donors in anatomical research.
Figures






References
-
- Agur AMR. Grant’s atlas of anatomy. 12. Lippincott: Williams & Wilkins; 2006.
-
- Arnold F (1838) Icones nervorum capitis. Sumptibus Auctoris
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

