The Impact of Steroid Responder Status on Long-Term Outcomes in Critically Ill Patients With Acute Respiratory Distress Syndrome Receiving High-Dose Glucocorticoids
- PMID: 38699135
- PMCID: PMC11064740
- DOI: 10.7759/cureus.57445
The Impact of Steroid Responder Status on Long-Term Outcomes in Critically Ill Patients With Acute Respiratory Distress Syndrome Receiving High-Dose Glucocorticoids
Abstract
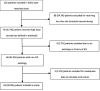
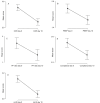
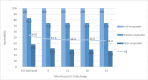
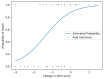
Background and objective High-dose intravenous pulsed glucocorticosteroids (GCS) are not part of the standard treatment in acute respiratory distress syndrome (ARDS), and the evidence supporting their use is conflicting. In clinical practice, however, they are used in specialist settings when clinico-patho-radiological features suggest a potentially steroid-responsive pattern, or as a last resort in cases where patients are unable to be weaned off mechanical ventilation. This study aimed to investigate if an early objective response to high-dose GCS treatment in selected critically ill patients is predictive of survival in ARDS. Methods This study involved a case series of 63 patients treated at a tertiary specialist respiratory ICU between 2009 and 2017 who received high-dose GCS for ARDS following a multidisciplinary board agreement. Patients were stratified according to the change in their modified lung injury score (mLIS) between days 0 and 10 following GCS initiation. Changes in mLIS (range: 0-4) were grouped as follows - full responders: ≥2, partial responders: ≥1 and <2, and non-responders: <1. Mortality on discharge and at 6, 12, 18, and 24 months post-ICU discharge was assessed for each group. Data were analysed using logistic regression and a receiver operating curve (ROC) to determine a statistically significant association between the change in mLIS and survival. Results Of the 63 patients, there were seven full responders, 12 partial responders, and 44 non-responders to high-dose GCS. Overall mortality at ICU discharge and 6, 12, 18 and 24 months post-discharge was 29/63 (46.0%), 33/63 (52.4%), 34/63 (54.0%), 34/63 (54.0%), and 35/63 (55.6%) respectively. Mortality was significantly lower in the partial and full-response groups than in the non-response group at all time frames. Logistic regression showed a significant association between the change in mLIS and survival (p<0.001), and a ROC demonstrated that categorising the change in mLIS was a good predictive model for survival (c-statistic 0.86). Conclusions Measuring the change in mLIS by day 10 following high-dose GCS administration for ARDS may be clinically useful in prognosticating such patients. Further research using mLIS as a measure of response to GCS, and larger datasets to enable the evaluation of prognostic factors, may assist clinicians in predicting which patients with persistent ARDS are likely to respond to GCS therapy.
Keywords: acute respiratory distress syndrome [ards]; extracorporeal membrane oxygenation support; glucocorticoid therapy; immunosuppression; invasive mechanical ventilation; lung injury score; mortality predictors; pulmonary critical care; response; systemic steroids.
Copyright © 2024, Leahy et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Nebulised heparin for patients with or at risk of acute respiratory distress syndrome: a multicentre, randomised, double-blind, placebo-controlled phase 3 trial.Lancet Respir Med. 2021 Apr;9(4):360-372. doi: 10.1016/S2213-2600(20)30470-7. Epub 2021 Jan 22. Lancet Respir Med. 2021. PMID: 33493448 Free PMC article. Clinical Trial.
-
[Dynamic measurement of volume of atelectasis area in the evaluation of the prognosis of patients with moderate-to-severe acute respiratory distress syndrome].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2020 Sep;32(9):1056-1060. doi: 10.3760/cma.j.cn121430-20191219-00056. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2020. PMID: 33081890 Chinese.
-
Extracorporeal lung support technologies - bridge to recovery and bridge to lung transplantation in adult patients: an evidence-based analysis.Ont Health Technol Assess Ser. 2010;10(5):1-47. Epub 2010 Apr 1. Ont Health Technol Assess Ser. 2010. PMID: 23074408 Free PMC article.
-
Efficacy of outcome prediction of the respiratory ECMO survival prediction score and the predicting death for severe ARDS on VV-ECMO score for patients with acute respiratory distress syndrome on extracorporeal membrane oxygenation.Perfusion. 2023 Oct;38(7):1340-1348. doi: 10.1177/02676591221115267. Epub 2022 Jul 13. Perfusion. 2023. PMID: 35830605 Review.
-
Acute Respiratory Distress Syndrome: Advances in Diagnosis and Treatment.JAMA. 2018 Feb 20;319(7):698-710. doi: 10.1001/jama.2017.21907. JAMA. 2018. PMID: 29466596 Review.
References
-
- Prolonged glucocorticoid treatment is associated with improved ARDS outcomes: analysis of individual patients' data from four randomized trials and trial-level meta-analysis of the updated literature. Meduri GU, Bridges L, Shih MC, Marik PE, Siemieniuk RA, Kocak M. Intensive Care Med. 2016;42:829–840. - PubMed
-
- Efficacy and safety of corticosteroids for persistent acute respiratory distress syndrome. Steinberg KP, Hudson LD, Goodman RB, et al. N Engl J Med. 2006;354:1671–1684. - PubMed
-
- The pathologist's approach to acute lung injury. Beasley MB. Arch Pathol Lab Med. 2010;134:719–727. - PubMed
LinkOut - more resources
Full Text Sources
