Urinary Epidermal Growth Factor Level as a Noninvasive Indicator of Tubular Repair in Patients with Acute Kidney Injury
- PMID: 38732362
- PMCID: PMC11083164
- DOI: 10.3390/diagnostics14090947
Urinary Epidermal Growth Factor Level as a Noninvasive Indicator of Tubular Repair in Patients with Acute Kidney Injury
Abstract
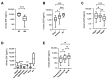
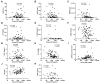
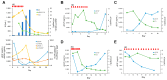
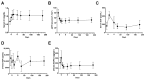
Epidermal growth factor (EGF), an essential factor for the proliferation and survival of renal tubular cells, is expressed by distal tubules and normally excreted via urine. Previous studies in rats demonstrated that acute tubular injury reduces urinary EGF levels. However, it is unclear whether urinary EGF is a suitable monitoring marker of tubular repair status after acute kidney injury (AKI) in humans. To address this question, we measured serum and urinary EGF in patients with AKI (n = 99) using ELISA and investigated whether urinary EGF levels were associated with the severity of tubular injury and renal prognosis. Urinary EGF was abundant in healthy controls but showed a significant decrease in AKI patients (14,522 ± 2190 pg/mL vs. 3201 ± 459.7 pg/mL, p < 0.05). The urinary EGF level in patients with renal AKI was notably lower than that in patients with pre-renal AKI. Furthermore, the urinary EGF level in patients with AKI stage 3 was significantly lower than that in patients with AKI stage 1. Urinary EGF levels were negatively correlated with urinary β-2MG and serum creatinine levels but positively correlated with hemoglobin levels and eGFR. Urinary EGF was not significantly correlated with urinary NAG, α-1MG, L-FABP, NGAL, KIM-1, or urinary protein concentrations. No significant correlation was observed between serum and urinary EGF levels, suggesting that urinary EGF is derived from the renal tubules rather than the blood. In living renal transplantation donors, the urinary EGF/Cr ratio was approximately half the preoperative urinary EGF/Cr ratio after unilateral nephrectomy. Collectively, these data suggest that urinary EGF is a suitable noninvasive indicator of not only the volume of functional normal renal tubules but also the status of tubular repair after AKI.
Keywords: EGF; acute kidney injury; urinary biomarker.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Potential Utility of Urinary Follistatin as a Non-Invasive Indicator of Acute Tubular Damage in Patients with Acute Kidney Injury.Cells. 2024 Mar 16;13(6):525. doi: 10.3390/cells13060525. Cells. 2024. PMID: 38534369 Free PMC article.
-
Performance of Serum Creatinine and Kidney Injury Biomarkers for Diagnosing Histologic Acute Tubular Injury.Am J Kidney Dis. 2017 Dec;70(6):807-816. doi: 10.1053/j.ajkd.2017.06.031. Epub 2017 Aug 24. Am J Kidney Dis. 2017. PMID: 28844586 Free PMC article.
-
Urinary tubular protein-based biomarkers in the rodent model of cisplatin nephrotoxicity: a comparative analysis of serum creatinine, renal histology, and urinary KIM-1, NGAL, and NAG in the initiation, maintenance, and recovery phases of acute kidney injury.J Investig Med. 2013 Mar;61(3):564-8. doi: 10.2310/JIM.0b013e31828233a8. J Investig Med. 2013. PMID: 23360846
-
Current concepts and advances in biomarkers of acute kidney injury.Crit Rev Clin Lab Sci. 2021 Aug;58(5):354-368. doi: 10.1080/10408363.2021.1879000. Epub 2021 Feb 8. Crit Rev Clin Lab Sci. 2021. PMID: 33556265 Review.
-
Update on biomarkers of acute kidney injury: moving closer to clinical impact?Mol Diagn Ther. 2012 Aug 1;16(4):199-207. doi: 10.1007/BF03262209. Mol Diagn Ther. 2012. PMID: 22650449 Review.
Cited by
-
Urinary EGF: Back to the Future.Kidney360. 2025 Mar 1;6(3):348-350. doi: 10.34067/KID.0000000720. Kidney360. 2025. PMID: 40146552 Free PMC article. No abstract available.
-
GDF15, EGF, and Neopterin in Assessing Progression of Pediatric Chronic Kidney Disease Using Artificial Intelligence Tools-A Pilot Study.Int J Mol Sci. 2025 Mar 6;26(5):2344. doi: 10.3390/ijms26052344. Int J Mol Sci. 2025. PMID: 40076962 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

