Practice and Predictors of Do-Not-Resuscitate Orders in a Tertiary-Care Intensive Care Unit in Saudi Arabia
- PMID: 38742230
- PMCID: PMC11090671
- DOI: 10.1155/2024/5516516
Practice and Predictors of Do-Not-Resuscitate Orders in a Tertiary-Care Intensive Care Unit in Saudi Arabia
Abstract
Introduction: The objective of this study was to describe Do-Not-Resuscitate (DNR) practices in a tertiary-care intensive care unit (ICU) in Saudi Arabia, and determine the predictors and outcomes of patients who had DNR orders.
Methods: This retrospective cohort study was based on a prospectively collected database for a medical-surgicalIntensive CareDepartment in a tertiary-care center in Riyadh, Saudi Arabia (1999-2017). We compared patients who had DNR orders during the ICU stay with those with "full code." The primary outcome was hospital mortality. The secondary outcomes included ICU mortality, tracheostomy, duration of mechanical ventilation, and length of stay in the ICU and hospital.
Results: Among 24790 patients admitted to the ICU over the 19-year study period, 3217 (13%) had DNR orders during the ICU stay. Compared to patients with "full code," patients with DNR orders were older (median 67 years [Q1, Q3: 55, 76] versus 57 years [Q1, Q3: 33, 71], p < 0.0001), were more likely to be females (43% versus 38%, p < 0.0001), had worse premorbid functional status (WHO performance status scores 4-5: 606[18.9%] versus 1894[8.8%], p < 0.0001), higher prevalence of comorbid conditions, and higher APACHE II score (median 28 [Q1, Q3: 23, 34] versus 19 [Q1, Q3: 13, 25], p < 0.0001) and were more likely to be mechanically ventilated (83% versus 55%, p < 0.0001). Patients had DNR orders were more likely to die in the ICU (67.8% versus 8.5%, p < 0.0001) and hospital (82.4% versus 18.1%, p < 0.0001). On multivariable logistic regression analysis, the following were associated with an increased likelihood of DNR status: increasing age (odds ratio (OR) 1.01, 95% confidence interval (CI) 1.01-1.02), higher APACHE II score (OR 1.09, 95% CI 1.08-1.10), and worse WHO performance status score. Patients admitted in recent years (2012-2017 versus 2002-2005) were less likely to have DNR orders (OR 0.35, 95% CI 0.32-0.39, p < 0.0001). Patients with DNR orders had higher ICU mortality, more tracheostomies, longer duration of mechanical ventilation and length of ICU stay compared to patients with with "full code" but they had shorter length of hospital stay.
Conclusion: In a tertiary-care hospital in Saudi Arabia, 13% of critically ill patients had DNR orders during ICU stay. This study identified several predictors of DNR orders, including the severity of illness and poor premorbid functional status.
Copyright © 2024 Abdulrahman Asiri et al.
Conflict of interest statement
The authors declare that there are no conflicts of interest regarding the publication of this article.
Figures
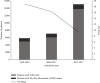
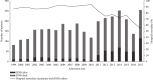
References
LinkOut - more resources
Full Text Sources

