Classifying Self-Reported Rheumatoid Arthritis Flares Using Daily Patient-Generated Data From a Smartphone App: Exploratory Analysis Applying Machine Learning Approaches
- PMID: 38743480
- PMCID: PMC11134244
- DOI: 10.2196/50679
Classifying Self-Reported Rheumatoid Arthritis Flares Using Daily Patient-Generated Data From a Smartphone App: Exploratory Analysis Applying Machine Learning Approaches
Abstract
Background: The ability to predict rheumatoid arthritis (RA) flares between clinic visits based on real-time, longitudinal patient-generated data could potentially allow for timely interventions to avoid disease worsening.
Objective: This exploratory study aims to investigate the feasibility of using machine learning methods to classify self-reported RA flares based on a small data set of daily symptom data collected on a smartphone app.
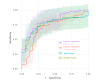
Methods: Daily symptoms and weekly flares reported on the Remote Monitoring of Rheumatoid Arthritis (REMORA) smartphone app from 20 patients with RA over 3 months were used. Predictors were several summary features of the daily symptom scores (eg, pain and fatigue) collected in the week leading up to the flare question. We fitted 3 binary classifiers: logistic regression with and without elastic net regularization, a random forest, and naive Bayes. Performance was evaluated according to the area under the curve (AUC) of the receiver operating characteristic curve. For the best-performing model, we considered sensitivity and specificity for different thresholds in order to illustrate different ways in which the predictive model could behave in a clinical setting.
Results: The data comprised an average of 60.6 daily reports and 10.5 weekly reports per participant. Participants reported a median of 2 (IQR 0.75-4.25) flares each over a median follow-up time of 81 (IQR 79-82) days. AUCs were broadly similar between models, but logistic regression with elastic net regularization had the highest AUC of 0.82. At a cutoff requiring specificity to be 0.80, the corresponding sensitivity to detect flares was 0.60 for this model. The positive predictive value (PPV) in this population was 53%, and the negative predictive value (NPV) was 85%. Given the prevalence of flares, the best PPV achieved meant only around 2 of every 3 positive predictions were correct (PPV 0.65). By prioritizing a higher NPV, the model correctly predicted over 9 in every 10 non-flare weeks, but the accuracy of predicted flares fell to only 1 in 2 being correct (NPV and PPV of 0.92 and 0.51, respectively).
Conclusions: Predicting self-reported flares based on daily symptom scorings in the preceding week using machine learning methods was feasible. The observed predictive accuracy might improve as we obtain more data, and these exploratory results need to be validated in an external cohort. In the future, analysis of frequently collected patient-generated data may allow us to predict flares before they unfold, opening opportunities for just-in-time adaptative interventions. Depending on the nature and implication of an intervention, different cutoff values for an intervention decision need to be considered, as well as the level of predictive certainty required.
Keywords: arthritic; arthritis; classification; classify; flare; flares; joint; joints; machine learning; mobile health; mobile phone; musculoskeletal; patient-generated health data; rheumatic; rheumatism; rheumatoid arthritis; smartphone; symptom; symptoms.
©Julie Gandrup, David A Selby, William G Dixon. Originally published in JMIR Formative Research (https://formative.jmir.org), 14.05.2024.
Conflict of interest statement
Conflicts of Interest: JG is currently employed at UCB Pharma, but this work was completed before joining UCB Pharma. WGD has received consultancy fees from Google, unrelated to this work. DAS declares no conflicts of interest.
Figures

References
-
- Hewlett S, Sanderson T, May J, Alten R, Bingham CO, Cross M, March L, Pohl C, Woodworth T, Bartlett SJ. 'I'm hurting, I want to kill myself': rheumatoid arthritis flare is more than a high joint count—an international patient perspective on flare where medical help is sought. Rheumatology (Oxford) 2012;51(1):69–76. doi: 10.1093/rheumatology/keq455. https://academic.oup.com/rheumatology/article/51/1/69/1772753?login=false keq455 - DOI - PubMed
-
- Markusse IM, Dirven L, Gerards AH, van Groenendael JHLM, Ronday HK, Kerstens PJSM, Lems WF, Huizinga TWJ, Allaart CF. Disease flares in rheumatoid arthritis are associated with joint damage progression and disability: 10-year results from the BeSt study. Arthritis Res Ther. 2015;17(1):232. doi: 10.1186/s13075-015-0730-2. https://arthritis-research.biomedcentral.com/articles/10.1186/s13075-015... 10.1186/s13075-015-0730-2 - DOI - PMC - PubMed
-
- Kuettel D, Primdahl J, Christensen R, Ørnbjerg LM, Hørslev-Petersen K. Impact of patient-reported flares on radiographic progression and functional impairment in patients with rheumatoid arthritis: a cohort study based on the AMBRA trial. Scand J Rheumatol. 2018;47(2):87–94. doi: 10.1080/03009742.2017.1329457. - DOI - PubMed
-
- Flurey CA, Morris M, Richards P, Hughes R, Hewlett S. It's like a juggling act: rheumatoid arthritis patient perspectives on daily life and flare while on current treatment regimes. Rheumatology (Oxford) 2014;53(4):696–703. doi: 10.1093/rheumatology/ket416. https://europepmc.org/abstract/MED/24357813 ket416 - DOI - PMC - PubMed
-
- Fautrel B, Alten R, Kirkham B, de la Torre I, Durand F, Barry J, Holzkaemper T, Fakhouri W, Taylor PC. Call for action: how to improve use of patient-reported outcomes to guide clinical decision making in rheumatoid arthritis. Rheumatol Int. 2018;38(6):935–947. doi: 10.1007/s00296-018-4005-5. https://europepmc.org/abstract/MED/29564549 10.1007/s00296-018-4005-5 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources

