Airway Management for Acute and Reconstructive Burns: Our 30-year Experience
- PMID: 38746695
- PMCID: PMC11090659
- DOI: 10.1055/s-0044-1786008
Airway Management for Acute and Reconstructive Burns: Our 30-year Experience
Abstract
Airway management in both acute and reconstructive burn patients can be a major challenge for evaluation, intubation, and securing the airway in the setting of altered airway structure. Airway evaluation in both acute and reconstructive patients includes examination for evidence of laryngeal and supraglottic edema and structural changes due to trauma and/or scarring that will impact the successful approach to acquiring an airway for surgical procedures and medical recovery. The approach to acquiring a successful airway is rarely standard laryngoscopy and often requires fiberoptic bronchoscopy and a variety of airway manipulation techniques. Tracheostomy should be reserved for those with classic requirements of ventilatory and/or mechanical failure or severe upper airway burns. Even securing an airway for surgical procedures, especially with patients suffering injuries involving the head and neck, can be nonstandard and requires creative and flexible approaches to be successful. After much trial and error over the past 30 years in a large burn center, our multidisciplinary team has learned many valuable lessons. This review will focus on our current approach to safe airway management in acute and reconstructive burn patients.
Keywords: airway evaluation; airway management; bronchoscopy; pediatric burn.
Thieme. All rights reserved.
Conflict of interest statement
Conflict of Interest None declared.
Figures
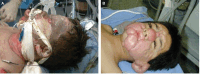
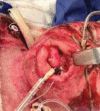
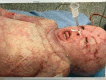
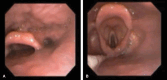


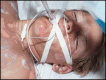


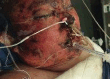
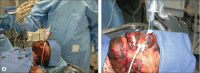
Similar articles
-
Determining the role of nasolaryngoscopy in the initial evaluation for upper airway injury in patients with facial burns.Burns. 2018 May;44(3):539-543. doi: 10.1016/j.burns.2017.09.009. Epub 2017 Nov 6. Burns. 2018. PMID: 29122412
-
Managing difficult airway in patients with post-burn mentosternal and circumoral scar contractures.Int J Burns Trauma. 2012;2(2):80-5. Epub 2012 Sep 15. Int J Burns Trauma. 2012. PMID: 23071905 Free PMC article.
-
Airway Management in Pediatric Patients With Burn Contractures of the Face and Neck.J Burn Care Res. 2022 Sep 1;43(5):1186-1202. doi: 10.1093/jbcr/irac016. J Burn Care Res. 2022. PMID: 35137105
-
Airway management of recovered pediatric patients with severe head and neck burns: a review.Paediatr Anaesth. 2012 May;22(5):462-8. doi: 10.1111/j.1460-9592.2012.03795.x. Epub 2012 Jan 19. Paediatr Anaesth. 2012. PMID: 22260458 Review.
-
Preventing Unnecessary Intubations: A 5-Year Regional Burn Center Experience Using Flexible Fiberoptic Laryngoscopy for Airway Evaluation in Patients With Suspected Inhalation or Airway Injury.J Burn Care Res. 2019 Apr 26;40(3):341-346. doi: 10.1093/jbcr/irz016. J Burn Care Res. 2019. PMID: 31222272
Cited by
-
Emergency Treatment of Burns in Adults-Characteristics of Adult Patients and Acute/Pre-Hospital Burn Management.Eur Burn J. 2025 Apr 10;6(2):19. doi: 10.3390/ebj6020019. Eur Burn J. 2025. PMID: 40265374 Free PMC article.
References
-
- Apfelbaum J L, Hagberg C A, Connis R T et al.2022 American Society of Anesthesiologists practice guidelines for management of the difficult airway. Anesthesiology. 2022;136(01):31–81. - PubMed
-
- Crawley S M, Dalton A J. Predicting the difficult airway. BJA Educ. 2015;15(05):253–258.
-
- Rafique N B, Khan F A. Comparison of Mallampati test, thyromental distance and distance from tragus to nares for predicting difficult intubation in pediatric patients. Open J Anesthesiol. 2014;04(04):104–109.
-
- Whitten C.10 common pediatric airway problems—and their solutionsAnesthesiology News 2019;August 20:Airway Management:51–69
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

