Experimental comparison of first-pass effect between direct thromboaspiration and combined thrombectomy in the setting of distal basilar occlusion
- PMID: 38751100
- PMCID: PMC11569773
- DOI: 10.1177/15910199241254412
Experimental comparison of first-pass effect between direct thromboaspiration and combined thrombectomy in the setting of distal basilar occlusion
Abstract
Background: Studies investigating endovascular therapy in vertebro-basilar stroke have led to controversial results in the past, but recent randomized trials seem to show an effectiveness superiority of endovascular therapy versus best medical treatment. However, uncertainty remains concerning many aspects of thrombectomy in acute basilar artery occlusion, notably technical considerations. This study compared the first-pass effect of direct thromboaspiration and combined thrombectomy in the setting of distal basilar occlusion.
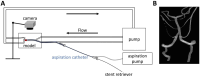
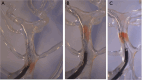
Methods: An in-vitro experimental set-up was used, consisting of a vascular phantom model and thrombus analogs of different consistencies to mimic human clots. Thrombus analogs were injected into the model through the vertebral artery and flowed to the basilar distal third to mimic a distal basilar occlusion. Ten procedures were performed for each thrombus analog stiffness and technique (direct thromboaspiration versus combined thrombectomy).
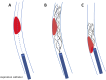
Results: Direct thromboaspiration showed an overall first-pass effect rate of 83.3% (25/30) and was particularly effective for ultra-soft and soft clot analogs, but decreased for hard clot analogs. Combined thrombectomy had an overall first-pass effect rate of 56.7% (17/30). The effect rate for ultra-soft and soft clot analogs was 60% and 50% for hard clot analogs. In the softer clot analogs, the stent-retriever device used for the combined thrombectomies tended to deviate the clot analog from a co-axial trajectory with the aspiration catheter.
Conclusions: In the context of distal basilar occlusion, our in-vitro results showed that higher first-pass effect rates were achieved with direct thromboaspiration compared to combined thrombectomy in all types of thrombus analogs.
Keywords: Stroke; basilar artery; in-vitro techniques; thrombectomy.
Conflict of interest statement
Declaration of conflicting interestsThe authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: PM is consultant for Medtronic and Stryker.
Figures
Similar articles
-
Direct thromboaspiration efficacy for mechanical thrombectomy is related to the angle of interaction between the aspiration catheter and the clot.J Neurointerv Surg. 2020 Apr;12(4):396-400. doi: 10.1136/neurintsurg-2019-015113. Epub 2019 Sep 23. J Neurointerv Surg. 2020. PMID: 31548213 Free PMC article.
-
Influence of Thrombus Composition on Thrombectomy: ADAPT vs. Balloon Guide Catheter and Stent Retriever in a Flow Model.Rofo. 2020 Mar;192(3):257-263. doi: 10.1055/a-0998-4246. Epub 2019 Sep 12. Rofo. 2020. PMID: 31514211 English.
-
Clot Meniscus Sign: An Angiographic Clue for Choosing between Stent Retriever and Contact Aspiration in Acute Basilar Artery Occlusion.AJNR Am J Neuroradiol. 2021 Apr;42(4):732-737. doi: 10.3174/ajnr.A6988. Epub 2021 Feb 4. AJNR Am J Neuroradiol. 2021. PMID: 33541894 Free PMC article.
-
Endovascular Stroke Therapy Focused on Stent Retriever Thrombectomy and Direct Clot Aspiration: Historical Review and Modern Application.J Korean Neurosurg Soc. 2017 May;60(3):335-347. doi: 10.3340/jkns.2016.0809.005. Epub 2017 May 1. J Korean Neurosurg Soc. 2017. PMID: 28490161 Free PMC article. Review.
-
Therapy for acute basilar artery occlusion: a systematic review and meta-analysis.F1000Res. 2019 Feb 7;8:165. doi: 10.12688/f1000research.18042.1. eCollection 2019. F1000Res. 2019. PMID: 31016013 Free PMC article.
References
-
- Tao C, Nogueira RG, Zhu Y, et al. Trial of endovascular treatment of acute basilar-artery occlusion. N Engl J Med 2022; 387: 1361–1372. - PubMed
-
- Jovin TG, Li C, Wu L, et al. Trial of thrombectomy 6 to 24 hours after stroke due to basilar-artery occlusion. N Engl J Med 2022; 387: 1373–1384. - PubMed
-
- Schonewille WJ. Favorable outcomes in endovascular therapy for basilar-artery occlusion. N Engl J Med 2022; 387: 1428–1429. - PubMed
-
- Kayan Y, Meyers PM, Prestigiacomo CJ, et al. Current endovascular strategies for posterior circulation large vessel occlusion stroke: report of the Society of NeuroInterventional Surgery Standards and Guidelines Committee. J NeuroIntervent Surg 2019; 11: 1055–1062. - PubMed
-
- Gory B, Mazighi M, Blanc R, et al. Mechanical thrombectomy in basilar artery occlusion: influence of reperfusion on clinical outcome and impact of the first-line strategy (ADAPT vs stent retriever). J Neurosurg 2018; 129: 1482–1491. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

