Predicting heart failure symptoms from the apnoea-hypopnoea index determined by full- night polysomnography
- PMID: 38751325
- PMCID: PMC11424366
- DOI: 10.1002/ehf2.14824
Predicting heart failure symptoms from the apnoea-hypopnoea index determined by full- night polysomnography
Abstract
Aims: Sleep-disordered breathing (SDB) is closely related to cardiovascular diseases. The higher the apnoea-hypopnoea index (AHI), the higher the prevalence of cardiovascular diseases. Despite these findings suggesting a close link between SDB and heart failure, the relationship between the severity of SDB and the onset of heart failure symptoms in individuals without apparent heart failure symptoms (Heart Failure Stage A + B) remains poorly understood.
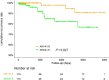
Methods and results: Between December 2010 and June 2017, we conducted full-night polysomnography (PSG) at the Nippon Medical School Chiba Hokusoh Hospital, extracting patients who were at risk of heart failure (Stage A or B in the Heart Failure Guidelines). Using a median cut-off of AHI ≥ 41.6 events/hour, we divided the patients into two groups and examined the composite endpoint of all-cause mortality plus hospitalization due to heart failure as the primary endpoint. We included 230 patients (mean age 63.0 ± 12.5 years, 78.3% males) meeting the selection criteria. When comparing the two groups, those with AHI < 41.6 events/hour (L group, n = 115) and those with AHI ≥ 41.6 events/hour (H group, n = 115), the H group had higher body mass index and higher serum triglyceride, and lower the frequency of acute coronary syndrome and lower estimated glomerular filtration rate than did the L group, but no other patient characteristics differed significantly. The H group had a significantly higher incidence of the composite endpoint than did the L group (10.6% vs. 2.6%, P = 0.027). Factors associated with the composite endpoint were identified through multivariate analyses, with AHI, haemoglobin, and left atrial dimension emerging as significant factors (hazard ratio [HR] = 1.02, 95% confidence interval [CI] = 1.00-1.04, P = 0.024; HR = 0.71, 95% CI = 0.54-0.94, P = 0.017; and HR = 1.10, 95% CI = 1.03-1.18, P = 0.006, respectively). Conversely, the minimum SpO2 during PSG (<80%) was not associated with the composite endpoint.
Conclusions: In patients with SDB who are at risk of heart failure, severe SDB is associated with a high risk of all-cause mortality and the development of heart failure. Additionally, combining cardiac echocardiography and PSG data may improve risk stratification, offering potential assistance for early intervention. Further examination with a validation cohort is necessary.
Keywords: Apnoea–hypopnoea index; Heart failure; Polysomnography; Sleep apnoea syndrome.
© 2024 The Authors. ESC Heart Failure published by John Wiley & Sons Ltd on behalf of European Society of Cardiology.
Conflict of interest statement
None declared.
Figures

Similar articles
-
Relationship between sleep-disordered breathing level and acute onset time of congestive heart failure.Int Heart J. 2008 Jul;49(4):471-80. doi: 10.1536/ihj.49.471. Int Heart J. 2008. PMID: 18753730
-
Impact of sleep disordered breathing severity on hemodynamics, autonomic balance and cardiopulmonary functional status in chronic heart failure.Int J Cardiol. 2010 Jun 11;141(3):227-35. doi: 10.1016/j.ijcard.2008.11.191. Epub 2009 Jan 13. Int J Cardiol. 2010. PMID: 19144429
-
Association between sleep-disordered breathing and arterial stiffness in heart failure patients with reduced or preserved ejection fraction.ESC Heart Fail. 2018 Jun;5(3):284-291. doi: 10.1002/ehf2.12273. Epub 2018 Feb 20. ESC Heart Fail. 2018. PMID: 29460495 Free PMC article.
-
Prevalence and Clinical Correlates of Sleep-Disordered Breathing in Patients Hospitalized With Acute Decompensated Heart Failure.Can J Cardiol. 2018 Jun;34(6):784-790. doi: 10.1016/j.cjca.2018.03.006. Epub 2018 Mar 16. Can J Cardiol. 2018. PMID: 29801743
-
Should All Congestive Heart Failure Patients Have a Routine Sleep Apnea Screening? Con.Can J Cardiol. 2015 Jul;31(7):940-4. doi: 10.1016/j.cjca.2015.04.013. Epub 2015 Apr 23. Can J Cardiol. 2015. PMID: 26112304 Free PMC article. Review.
Cited by
-
Association of estimated pulse wave velocity with all-cause mortality and cardiovascular mortality in obstructive sleep apnea patients: results from NHANES.Front Cardiovasc Med. 2025 Jun 12;12:1571610. doi: 10.3389/fcvm.2025.1571610. eCollection 2025. Front Cardiovasc Med. 2025. PMID: 40574813 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

