Preoperative Prediction of Microvascular Invasion with Gadoxetic Acid-Enhanced Magnetic Resonance Imaging in Patients with Single Hepatocellular Carcinoma: The Implication of Surgical Decision on the Extent of Liver Resection
- PMID: 38751555
- PMCID: PMC11095589
- DOI: 10.1159/000531786
Preoperative Prediction of Microvascular Invasion with Gadoxetic Acid-Enhanced Magnetic Resonance Imaging in Patients with Single Hepatocellular Carcinoma: The Implication of Surgical Decision on the Extent of Liver Resection
Abstract
Introduction: Microvascular invasion (MVI) is one of the most important prognostic factors for hepatocellular carcinoma (HCC) recurrence, but its application in preoperative clinical decisions is limited. This study aimed to identify preoperative predictive factors for MVI in HCC and further evaluate oncologic outcomes of different types and extents of hepatectomy according to stratified risk of MVI.
Methods: Patients with surgically resected single HCC (≤5 cm) who underwent preoperative gadoxetic acid-enhanced magnetic resonance imaging (MRI) were included in a single-center retrospective study. Two radiologists reviewed the images with no clinical, pathological, or prognostic information. Significant predictive factors for MVI were identified using logistic regression analysis against pathologic MVI and used to stratify patients. In the subgroup analysis, long-term outcomes of the stratified patients were analyzed using the Kaplan-Meier method with log-rank test and compared between anatomical and nonanatomical or major and minor resection.
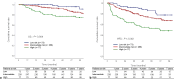
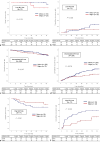
Results: A total of 408 patients, 318 men and 90 women, with a mean age of 56.7 years were included. Elevated levels of tumor markers (alpha-fetoprotein [α-FP] ≥25 ng/mL and PIVKA-II ≥40 mAU/mL) and three MRI features (tumor size ≥3 cm, non-smooth tumor margin, and arterial peritumoral enhancement) were independent predictive factors for MVI. As the MVI risk increased from low (no predictive factor) and intermediate (1-2 factors) to high-risk (3-4 factors), recurrence-free and overall survival of each group significantly decreased (p = 0.001). In the high MVI risk group, 5-year cumulative recurrence rate was significantly lower in patients who underwent major compared to minor hepatectomy (26.6 vs. 59.8%, p = 0.027).
Conclusion: Tumor markers and MRI features can predict the risk of MVI and prognosis after hepatectomy. Patients with high MVI risk had the worst prognosis among the three groups, and major hepatectomy improved long-term outcomes in these high-risk patients.
Keywords: Hepatectomy; Hepatocellular carcinoma; Magnetic resonance imaging; Microscopic vascular invasion; Recurrence.
© 2023 The Author(s). Published by S. Karger AG, Basel.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures


Similar articles
-
Preoperative gadoxetic acid-enhanced MRI for predicting microvascular invasion in patients with single hepatocellular carcinoma.J Hepatol. 2017 Sep;67(3):526-534. doi: 10.1016/j.jhep.2017.04.024. Epub 2017 May 6. J Hepatol. 2017. PMID: 28483680
-
Prediction for Aggressiveness and Postoperative Recurrence of Hepatocellular Carcinoma Using Gadoxetic Acid-Enhanced Magnetic Resonance Imaging.Acad Radiol. 2023 May;30(5):841-852. doi: 10.1016/j.acra.2022.12.018. Epub 2022 Dec 26. Acad Radiol. 2023. PMID: 36577606
-
Combined hepatocellular-cholangiocarcinoma: which preoperative clinical data and conventional MRI characteristics have value for the prediction of microvascular invasion and clinical significance?Eur Radiol. 2020 Oct;30(10):5337-5347. doi: 10.1007/s00330-020-06861-2. Epub 2020 May 8. Eur Radiol. 2020. PMID: 32385649 Free PMC article.
-
Significance of presence of microvascular invasion in specimens obtained after surgical treatment of hepatocellular carcinoma.J Gastroenterol Hepatol. 2018 Feb;33(2):347-354. doi: 10.1111/jgh.13843. J Gastroenterol Hepatol. 2018. PMID: 28589639 Review.
-
Preoperative prediction of microvascular invasion: new insights into personalized therapy for early-stage hepatocellular carcinoma.Quant Imaging Med Surg. 2024 Jul 1;14(7):5205-5223. doi: 10.21037/qims-24-44. Epub 2024 Jun 27. Quant Imaging Med Surg. 2024. PMID: 39022260 Free PMC article. Review.
Cited by
-
Diagnostic model using LI-RADS v2018 for predicting early recurrence of microvascular invasion-negative solitary hepatocellular carcinoma.Cancer Imaging. 2025 Mar 31;25(1):46. doi: 10.1186/s40644-025-00865-1. Cancer Imaging. 2025. PMID: 40165325 Free PMC article.
-
Letter to "Preoperative Prediction of Microvascular Invasion by EOB-MRI Imaging for Surgical Decision".Liver Cancer. 2024 Oct 17;14(3):351-352. doi: 10.1159/000541884. eCollection 2025 Jun. Liver Cancer. 2024. PMID: 40547963 Free PMC article. No abstract available.
-
Interpretable and generalizable deep learning model for preoperative assessment of microvascular invasion and outcome in hepatocellular carcinoma based on MRI: a multicenter study.Insights Imaging. 2025 Jul 3;16(1):151. doi: 10.1186/s13244-025-02035-0. Insights Imaging. 2025. PMID: 40610844 Free PMC article.
-
Developing a novel predictive model for identifying risk factors associated with being lost to follow-up among high-risk patients for recurrence following radical resection of hepatocellular carcinoma: the first report.BMC Cancer. 2025 Apr 2;25(1):597. doi: 10.1186/s12885-025-14030-1. BMC Cancer. 2025. PMID: 40175947 Free PMC article.
-
MRI-Based Topology Deep Learning Model for Noninvasive Prediction of Microvascular Invasion and Assisting Prognostic Stratification in HCC.Liver Int. 2025 Mar;45(3):e16205. doi: 10.1111/liv.16205. Liver Int. 2025. PMID: 39992060 Free PMC article.
References
-
- Kudo M. Multistep human hepatocarcinogenesis: correlation of imaging with pathology. J Gastroenterol. 2009;44(Suppl 19):112–8. - PubMed
-
- Rodriguez-Peralvarez M, Luong TV, Andreana L, Meyer T, Dhillon AP, Burroughs AK. A systematic review of microvascular invasion in hepatocellular carcinoma: diagnostic and prognostic variability. Ann Surg Oncol. 2013;20(1):325–39. - PubMed
-
- Lee S, Kang TW, Song KD, Lee MW, Rhim H, Lim HK, et al. . Effect of microvascular invasion risk on early recurrence of hepatocellular carcinoma after surgery and radiofrequency ablation. Ann Surg. 2021;273(3):564–71. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

