Synchronous supraclavicular vascularized lymph node transfer and liposuction for gynecological cancer-related lower extremity lymphedema: A clinical comparative analysis of three different procedures
- PMID: 38761979
- PMCID: PMC11523359
- DOI: 10.1016/j.jvsv.2024.101905
Synchronous supraclavicular vascularized lymph node transfer and liposuction for gynecological cancer-related lower extremity lymphedema: A clinical comparative analysis of three different procedures
Abstract
Objective: Gynecological cancer-related lower extremity lymphedema (GC-LEL), a chronic, progressive condition, lacks a standardized treatment. Currently, supraclavicular vascularized lymph node transfer (SC-VLNT) is a favored approach in the treatment of lymphedema, and there is a trend toward combination technology. This study conducts a comparative analysis of three techniques for treating GC-LEL with simultaneous SC-VLNT and liposuction.
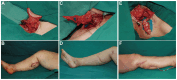
Methods: A cohort of 35 patients with GC-LEL was examined, comprising 13 patients who underwent single lymph nodes flap with a skin paddle (SLNF+P), 12 who received single lymph nodes flap without a skin paddle (SLNF), and 10 who accepted dual lymph nodes flap without a skin paddle (DLNF). Patient demographics and outcomes were meticulously documented, covering intra- and postoperative variables.
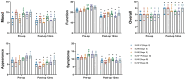
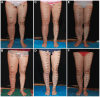
Results: The median limb volume reduction were 56.4% (SLNF+P), 60.8% (SLNF), and 50.5% (DLNF) in stage II, and 54.0% (SLNF+P), 59.8% (SLNF), and 54.4% (DLNF) in stage III. DLNF group procedures entailed longer flap harvesting and transplantation times. The SLNF+P group, on average, had an 8-day postoperative hospitalization, longer than others. All patients noted subjective improvements in Lymphedema Quality of Life scores, with lymphoscintigraphy revealing enhanced lymphatic flow in 29 of the 35 cases. A notable decrease in cellulitis incidence was observed. Additionally, the occurrence of cellulitis decreased significantly, except for DLNF (Stage Ⅱ). The median follow-up time was 16 months (range, 12-36 months), with no reported severe postoperative complications.
Conclusions: For advanced GC-LEL, SLNF combined with liposuction is a preferred treatment, offering fewer complications, shorter operative time, and hospitalization.
Keywords: Combination therapy; Liposuction; Lower extremity; Lymphedema; Vascularized lymph node.
Copyright © 2024 The Author(s). Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Disclosures None.
Figures


Similar articles
-
Changes on noncontrast magnetic resonance imaging following lymphatic surgery for upper extremity secondary lymphedema.J Vasc Surg Venous Lymphat Disord. 2025 Jan;13(1):101962. doi: 10.1016/j.jvsv.2024.101962. Epub 2024 Aug 6. J Vasc Surg Venous Lymphat Disord. 2025. PMID: 39117036 Free PMC article.
-
Gastroepiploic Vascularized Lymph Node Transfer for Extremity Lymphedema: Tips and Insights from Extensive Clinical Experience.Medicina (Kaunas). 2025 Mar 15;61(3):503. doi: 10.3390/medicina61030503. Medicina (Kaunas). 2025. PMID: 40142314 Free PMC article.
-
Comparison of vascularized supraclavicular lymph node transfer and lymphaticovenular anastomosis for advanced stage lower extremity lymphedema.Ann Plast Surg. 2015 May;74(5):573-9. doi: 10.1097/SAP.0000000000000513. Ann Plast Surg. 2015. PMID: 25875724
-
[Advances in treatment of lymphedema with supraclavicular vascularized lymph node transfer].Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2023 Jun 15;37(6):736-741. doi: 10.7507/1002-1892.202302104. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2023. PMID: 37331953 Free PMC article. Review. Chinese.
-
Surgical Treatment of Lymphedema.Plast Reconstr Surg. 2019 Sep;144(3):738-758. doi: 10.1097/PRS.0000000000005993. Plast Reconstr Surg. 2019. PMID: 31461041 Review.
Cited by
-
Case Report: Surgical management of primary lymphedema with a novel PROX1 mutation involving upper and lower limbs.Front Genet. 2025 Jul 3;16:1560471. doi: 10.3389/fgene.2025.1560471. eCollection 2025. Front Genet. 2025. PMID: 40678385 Free PMC article.
-
[Clinical efficacy of vascularized lymph node transfer combined with lymphatico-venous anastomosis in treating unilateral upper limb lymphedema after radical mastectomy for breast cancer].Zhonghua Shao Shang Yu Chuang Mian Xiu Fu Za Zhi. 2025 Jun 20;41(6):534-542. doi: 10.3760/cma.j.cn501225-20250228-00105. Zhonghua Shao Shang Yu Chuang Mian Xiu Fu Za Zhi. 2025. PMID: 40588401 Free PMC article. Chinese.
-
[An overview of integrated surgical management for secondary lower limb lymphedema guided by algorithms].Zhonghua Shao Shang Yu Chuang Mian Xiu Fu Za Zhi. 2025 Jun 20;41(6):516-524. doi: 10.3760/cma.j.cn501225-20250217-00067. Zhonghua Shao Shang Yu Chuang Mian Xiu Fu Za Zhi. 2025. PMID: 40480841 Free PMC article. Chinese.
References
-
- Grada A.A., Phillips T.J. Lymphedema: pathophysiology and clinical manifestations. J Am Acad Dermatol. 2017;77:1009–1020. - PubMed
-
- Yoshihara M., Shimono R., Tsuru S., et al. Risk factors for late-onset lower limb lymphedema after gynecological cancer treatment: a multi-institutional retrospective study. Eur J Surg Oncol. 2020;46:1334–1338. - PubMed
-
- Dayan J.H., Ly C.L., Kataru R.P., Mehrara B.J. Lymphedema: pathogenesis and novel therapies. Annu Rev Med. 2018;69:263–276. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

