Cancer survival in sub-Saharan Africa (SURVCAN-3): a population-based study
- PMID: 38762297
- PMCID: PMC11126368
- DOI: 10.1016/S2214-109X(24)00130-X
Cancer survival in sub-Saharan Africa (SURVCAN-3): a population-based study
Abstract
Background: The Cancer Survival in Africa, Asia, and South America project (SURVCAN-3) of the International Agency for Research on Cancer aims to fill gaps in the availability of population-level cancer survival estimates from countries in these regions. Here, we analysed survival for 18 cancers using data from member registries of the African Cancer Registry Network across 11 countries in sub-Saharan Africa.
Methods: We included data on patients diagnosed with 18 cancer types between Jan 1, 2005, and Dec 31, 2014, from 13 population-based cancer registries in Cotonou (Benin), Abidjan (CÔte d'Ivoire), Addis Ababa (Ethiopia), Eldoret and Nairobi (Kenya), Bamako (Mali), Mauritius, Namibia, Seychelles, Eastern Cape (South Africa), Kampala (Uganda), and Bulawayo and Harare (Zimbabwe). Patients were followed up until Dec 31, 2018. Patient-level data including cancer topography and morphology, age and date at diagnosis, vital status, and date of death (if applicable) were collected. The follow-up (survival) time was measured from the date of incidence until the date of last contact, the date of death, or until the end of the study, whichever occurred first. We estimated the 1-year, 3-year, and 5-year survival (observed, net, and age-standardised net survival) by sex, cancer type, registry, country, and human development index (HDI). 1-year and 3-year survival data were available for all registries and all cancer sites, whereas availability of 5-year survival data was slightly more variable; thus to provide medium-term survival prospects, we have focused on 3-year survival in the Results section.
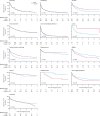
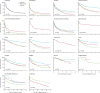
Findings: 10 500 individuals from 13 population-based cancer registries in 11 countries were included in the survival analyses. 9177 (87·4%) of 10 500 cases were morphologically verified. Survival from cancers with a high burden and amenable to prevention was poor: the 3-year age-standardised net survival was 52·3% (95% CI 49·4-55·0) for cervical cancer, 18·1% (11·5-25·9) for liver cancer, and 32·4% (27·5-37·3) for lung cancer. Less than half of the included patients were alive 3 years after a cancer diagnosis for eight cancer types (oral cavity, oesophagus, stomach, larynx, lung, liver, non-Hodgkin lymphoma, and leukaemia). There were differences in survival for some cancers by sex: survival was longer for females with stomach or lung cancer than males with stomach or lung cancer, and longer for males with non-Hodgkin lymphomas than females with non-Hodgkin lymphomas. Survival did not differ by country-level HDI for cancers of the oral cavity, oesophagus, liver, thyroid, and for Hodgkin lymphoma.
Interpretation: For cancers for which population-level prevention strategies exist, and with relatively poor prognosis, these estimates highlight the urgent need to upscale population-level prevention activities in sub-Saharan Africa. These data are vital for providing the knowledge base for advocacy to improve access to prevention, diagnosis, and care for patients with cancers in sub-Saharan Africa.
Funding: Vital Strategies, the Martin-Luther-University Halle-Wittenberg, and the International Agency for Research on Cancer.
Translations: For the French and Portuguese translations of the abstract see Supplementary Materials section.
This is an Open Access article published under the CC BY-NC-ND 3.0 IGO license which permits users to download and share the article for non-commercial purposes, so long as the article is reproduced in the whole without changes, and provided the original source is properly cited. This article shall not be used or reproduced in association with the promotion of commercial products, services or any entity. There should be no suggestion that WHO endorses any specific organisation, products or services. The use of the WHO logo is not permitted. This notice should be preserved along with the article's original URL.
Conflict of interest statement
Declaration of interests We declare no competing interests. Where authors are identified as personnel of the International Agency for Research on Cancer and WHO, the authors alone are responsible for the views expressed in this Article and they do not necessarily represent the decisions, policy, or views of the International Agency for Research on Cancer and WHO.
Figures

References
-
- Bray F, Parkin DM, Gnangnon F, et al. Cancer in sub-Saharan Africa in 2020: a review of current estimates of the national burden, data gaps, and future needs. Lancet Oncol. 2022;23:719–728. - PubMed
-
- Sankaranarayanan R, Swaminathan R, editors. Cancer survival in Africa, Asia, the Caribbean and Central America. International Agency for Research on Cancer, World Health Organization; Lyon: 2011.
-
- Soerjomataram I, Cabasag C, Bardot A, et al. Cancer survival in Africa, central and south America, and Asia (SURVCAN-3): a population-based benchmarking study in 32 countries. Lancet Oncol. 2023;24:22–32. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

