Economic implications of novel regimens for tuberculosis treatment in three high-burden countries: a modelling analysis
- PMID: 38762299
- PMCID: PMC11126367
- DOI: 10.1016/S2214-109X(24)00088-3
Economic implications of novel regimens for tuberculosis treatment in three high-burden countries: a modelling analysis
Abstract
Background: With numerous trials investigating novel drug combinations to treat tuberculosis, we aimed to evaluate the extent to which future improvements in tuberculosis treatment regimens could offset potential increases in drug costs.
Methods: In this modelling analysis, we used an ingredients-based approach to estimate prices at which novel regimens for rifampin-susceptible and rifampin-resistant tuberculosis treatment would be cost-neutral or cost-effective compared with standards of care in India, the Philippines, and South Africa. We modelled regimens meeting targets set in the WHO's 2023 Target Regimen Profiles (TRPs). Our decision-analytical model tracked cohorts of adults initiating rifampin-susceptible or rifampin-resistant tuberculosis treatment, simulating their health outcomes and costs accumulated during and following treatment under standard-of-care and novel regimen scenarios. Price thresholds included short-term cost-neutrality (considering only savings accrued during treatment), medium-term cost-neutrality (additionally considering savings from averted retreatments and secondary cases), and cost-effectiveness (incorporating willingness-to-pay for improved health outcomes).
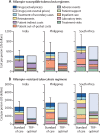
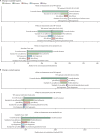
Findings: Total medium-term costs per person treated using standard-of-care regimens were estimated at US$450 (95% uncertainty interval 310-630) in India, $560 (350-860) in the Philippines, and $730 (530-1090) in South Africa for rifampin-susceptible tuberculosis (current drug costs $46) and $2100 (1590-2810) in India, $2610 (2090-3280) in the Philippines, and $3790 (3090-4630) in South Africa for rifampin-resistant tuberculosis (current drug costs $432). A rifampin-susceptible tuberculosis regimen meeting the optimal targets defined in the TRPs could be cost-neutral in the short term at drug costs of $140 (90-210) per full course in India, $230 (130-380) in the Philippines, and $280 (180-460) in South Africa. For rifampin-resistant tuberculosis, short-term cost-neutral thresholds were higher with $930 (720-1230) in India, $1180 (980-1430) in the Philippines, and $1480 (1230-1780) in South Africa. Medium-term cost-neutral prices were approximately $50-100 higher than short-term cost-neutral prices for rifampin-susceptible tuberculosis and $250-550 higher for rifampin-resistant tuberculosis. Health system cost-neutral prices that excluded patient-borne costs were 45-70% lower (rifampin-susceptible regimens) and 15-50% lower (rifampin-resistant regimens) than the cost-neutral prices that included patient costs. Cost-effective prices were substantially higher. Shorter duration was the most important driver of medium-term savings with novel regimens, followed by ease of adherence.
Interpretation: Improved tuberculosis regimens, particularly shorter regimens or those that facilitate better adherence, could reduce overall costs, potentially offsetting higher prices.
Funding: WHO.
Copyright © 2024 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY 4.0 license.
Conflict of interest statement
Declaration of interests TSR, CL, DWD, and EAK report funding from WHO. TSR and EAK report funding from the Bill & Melinda Gates Foundation. All other authors declare no competing interests.
Figures
References
-
- WHO Global tuberculosis report 2022. 2022. https://www.who.int/teams/global-tuberculosis-programme/tb-reports/globa...
-
- WHO The End TB Strategy. 2015. https://www.who.int/publications-detail-redirect/WHO-HTM-TB-2015.19
-
- Stop TB Partnership The Global Plan to End TB 2023–2030. 2022. https://www.stoptb.org/advocate-to-endtb/global-plan-to-end-tb
-
- WHO Consolidated guidelines on tuberculosis: drug-susceptible tuberculosis treatment. 2022. https://www.who.int/publications-detail-redirect/9789240048126
-
- WHO Consolidated guidelines on tuberculosis: drug-resistant tuberculosis treatment, 2022 update. 2022. https://www.who.int/publications-detail-redirect/9789240063129
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

