Cutaneous vasculitis: insights into pathogenesis and histopathological features
- PMID: 38767544
- PMCID: PMC11138767
- DOI: 10.32074/1591-951X-985
Cutaneous vasculitis: insights into pathogenesis and histopathological features
Abstract
The mechanisms underlying the onset and progression of vasculitis remain poorly understood. This condition is characterized by damage to the vascular wall, recruitment of inflammatory cells, and subsequent structural remodeling, which are hallmarks of vasculitis. The histopathological classification of vasculitis relies on the size of the affected vessel and the predominant type of inflammatory cell involved - neutrophils in acute cases, lymphocytes in chronic conditions, and histiocytes in granulomatous forms. Pathological changes progress in every context, and a single vasculitic pattern can be associated with various systemic conditions. Conversely, a single causative agent may lead to multiple distinct clinical and pathological manifestations of vasculitis. Moreover, many cases of vasculitis have no identifiable cause. A foundational understanding of the normal structure of the cutaneous vascular network is crucial. Similarly, identifying the cellular and molecular participants and their roles in forming the "dermal microvascular unit" is propedeutical.
This review aims to elucidate the complex mechanisms involved in the initiation and progression of vasculitis, offering a comprehensive overview of its histopathological classification, underlying causes, and the significant role of the cutaneous vascular network and cellular dynamics. By integrating the latest insights from studies on NETosis and the implications of lymphocytic infiltration in autoimmune diseases, we seek to bridge gaps in current knowledge and highlight areas for future research. Our discussion extends to the clinical implications of vasculitis, emphasizing the importance of identifying etiological agents and understanding the diverse histopathological manifestations to improve diagnostic accuracy and treatment outcomes.
Keywords: NETosis; dermal microvascular unit; leukocytoclastic; vasculitis histopathology; vasculitis pathogenesis.
Copyright © 2024 Società Italiana di Anatomia Patologica e Citopatologia Diagnostica, Divisione Italiana della International Academy of Pathology.
Conflict of interest statement
The authors declare no conflicts of interest. Date: 19/02/2024
Figures


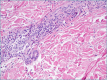
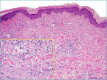


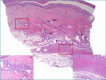
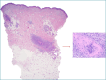

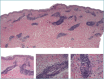


References
-
- Lyle AN, Taylor WR. The pathophysiological basis of vascular disease. Lab Invest. 2019;99(3):284-289. https://doi.org/10.1038/s41374-019-0192-2 10.1038/s41374-019-0192-2 - DOI - PubMed
-
- Carlson JA, Mihm MC, Jr., LeBoit PE. Cutaneous lymphocytic vasculitis: a definition, a review, and a proposed classification. Semin Diagn Pathol. 1996;13(1):72-90. - PubMed
-
- Watts RA, Hatemi G, Burns JC, et al. Global epidemiology of vasculitis. Nat Rev Rheumatol. 2022;18(1):22-34. https://doi.org/10.1038/s41584-021-00718-8 10.1038/s41584-021-00718-8 - DOI - PMC - PubMed
-
- Braverman IM, Keh-Yen A. Ultrastructure of the human dermal microcirculation. III. The vessels in the mid- and lower dermis and subcutaneous fat. J Invest Dermatol. 1981;77(3):297-304. https://doi.org/10.1111/1523-1747.ep12482470 10.1111/1523-1747.ep12482470 - DOI - PubMed
-
- Braverman IM. The cutaneous microcirculation: ultrastructure and microanatomical organization. Microcirculation. 1997;4(3):329-40. https://doi.org/10.3109/10739689709146797 10.3109/10739689709146797 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

