Computerized decision support is an effective approach to select memory clinic patients for amyloid-PET
- PMID: 38768188
- PMCID: PMC11104589
- DOI: 10.1371/journal.pone.0303111
Computerized decision support is an effective approach to select memory clinic patients for amyloid-PET
Abstract
Background: The use of amyloid-PET in dementia workup is upcoming. At the same time, amyloid-PET is costly and limitedly available. While the appropriate use criteria (AUC) aim for optimal use of amyloid-PET, their limited sensitivity hinders the translation to clinical practice. Therefore, there is a need for tools that guide selection of patients for whom amyloid-PET has the most clinical utility. We aimed to develop a computerized decision support approach to select patients for amyloid-PET.
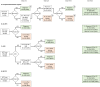
Methods: We included 286 subjects (135 controls, 108 Alzheimer's disease dementia, 33 frontotemporal lobe dementia, and 10 vascular dementia) from the Amsterdam Dementia Cohort, with available neuropsychology, APOE, MRI and [18F]florbetaben amyloid-PET. In our computerized decision support approach, using supervised machine learning based on the DSI classifier, we first classified the subjects using only neuropsychology, APOE, and quantified MRI. Then, for subjects with uncertain classification (probability of correct class (PCC) < 0.75) we enriched classification by adding (hypothetical) amyloid positive (AD-like) and negative (normal) PET visual read results and assessed whether the diagnosis became more certain in at least one scenario (PPC≥0.75). If this was the case, the actual visual read result was used in the final classification. We compared the proportion of PET scans and patients diagnosed with sufficient certainty in the computerized approach with three scenarios: 1) without amyloid-PET, 2) amyloid-PET according to the AUC, and 3) amyloid-PET for all patients.
Results: The computerized approach advised PET in n = 60(21%) patients, leading to a diagnosis with sufficient certainty in n = 188(66%) patients. This approach was more efficient than the other three scenarios: 1) without amyloid-PET, diagnostic classification was obtained in n = 155(54%), 2) applying the AUC resulted in amyloid-PET in n = 113(40%) and diagnostic classification in n = 156(55%), and 3) performing amyloid-PET in all resulted in diagnostic classification in n = 154(54%).
Conclusion: Our computerized data-driven approach selected 21% of memory clinic patients for amyloid-PET, without compromising diagnostic performance. Our work contributes to a cost-effective implementation and could support clinicians in making a balanced decision in ordering additional amyloid PET during the dementia workup.
Copyright: © 2024 Rhodius-Meester et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
We have read the journal’s policy and the authors of this paper have the following competing interests: Hanneke F.M. Rhodius-Meester performs contract research for Combinostics; all funding is paid to her institution. Ingrid van Maurik received a consultancy fee (paid to the university) from Roche. Lyduine E. Collij has received consultancy fees from GE Healthcare; all funding is paid to her institution. Juha Koikkalainen and Jyrki Lötjönen report that Combinostics Oy owns the following IPR related to the paper: 1. J. Koikkalainen and J. Lotjonen, “A method for inferring the state of a system,” US7,840,510 B2, PCT/FI2007/050277. 2. J. Lotjonen, J. Koikkalainen and J. Mattila, “State Inference in a heterogeneous system,” PCT/FI2010/050545, FI20125177. Koikkalainen and Lötjönen are shareholders in Combinostics Oy. Yolande A.L. Pijnenburg has received funding from Dioraphte Foundation, Zabawas Foundation, JPND, ZonMW, NWO, Team Alzheimer and the Dutch Brain Foundation. Frederik Barkhof is member of the Steering committee or Data Safety Monitoring Board member for Biogen, Merck, ATRI/ACTC and Prothena. Barkhof is a consultant for Roche, Celltrion, Rewind Therapeutics, Merck, IXICO, Jansen, Combinostics. Barkhof has research agreements with Merck, Biogen, GE Healthcare, Roche. Co-founder and shareholder of Queen Square Analytics LTD. Elsmarieke van de Giessen has received research support from NWO, ZonMw, Hersenstichting and KWF. van de Giessen has performed contract research for Heuron Inc., Roche and 1st Biotherapeutics. van deGiessen has a consultancy agreement with IXICO for the reading of PET scans. Wiesje M van der Flier performs contract research for Biogen. Research programs of van der Flier have been funded by ZonMW, NWO, EU-FP7, EU-JPND, Alzheimer Nederland, CardioVascular Onderzoek Nederland, Health~Holland, Topsector Life Sciences & Health, stichting Dioraphte, Gieskes-Strijbis fonds, stichting Equilibrio, Pasman stichting, stichting Alzheimer & NeuroPsychiatry Foundation, Philips, Biogen MA Inc, Novartis-NL, Life-MI, AVID, Roche BV, Fujifilm, Combinostics. van der Flier has performed contract research for Biogen MA Inc, and Boehringer Ingelheim. van der Flier has been an invited speaker at Boehringer Ingelheim, Biogen MA Inc, Danone, Eisai, WebMD Neurology (Medscape), Springer Healthcare. van der Flier is consultant to Oxford Health Policy Forum CIC, Roche and Biogen MA Inc. van der Flier participated in advisory boards of Biogen MA Inc. and Roche. All funding is paid to her institution. van der Flier was associate editor of Alzheimer, Research & Therapy in 2020/2021. van der Flier is associate editor at Brain. This does not alter our adherence to PLOS ONE policies on sharing data and materials.
Figures

References
-
- Chiotis K, Saint-Aubert L, Boccardi M, Gietl A, Picco A, Varrone A, et al.. Clinical validity of increased cortical uptake of amyloid ligands on PET as a biomarker for Alzheimer’s disease in the context of a structured 5-phase development framework. Neurobiol Aging. 2017;52:214–27. Epub 2017/03/21. doi: 10.1016/j.neurobiolaging.2016.07.012 . - DOI - PubMed
-
- Rabinovici GD, Gatsonis C, Apgar C, Chaudhary K, Gareen I, Hanna L, et al.. Association of Amyloid Positron Emission Tomography With Subsequent Change in Clinical Management Among Medicare Beneficiaries With Mild Cognitive Impairment or Dementia. Jama. 2019;321(13):1286–94. Epub 2019/04/03. doi: 10.1001/jama.2019.2000 . - DOI - PMC - PubMed
-
- de Wilde A, van der Flier WM, Pelkmans W, Bouwman F, Verwer J, Groot C, et al.. Association of Amyloid Positron Emission Tomography With Changes in Diagnosis and Patient Treatment in an Unselected Memory Clinic Cohort: The ABIDE Project. JAMA Neurol. 2018;75(9):1062–70. Epub 2018/06/12. doi: 10.1001/jamaneurol.2018.1346 . - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous

