Juvenile dermatomyositis with Anti-SAE antibodies in a Moroccan child associated with pseudo-angioedema: a case report
- PMID: 38773611
- PMCID: PMC11107000
- DOI: 10.1186/s12969-023-00921-9
Juvenile dermatomyositis with Anti-SAE antibodies in a Moroccan child associated with pseudo-angioedema: a case report
Abstract
Background: Juvenile Dermatomyositis (JDM) is the leading cause of non-infectious inflammatory myopathy in children. It is a heterogeneous group of autoimmune diseases characterized by a variable combination of muscular, dermatological, and visceral involvement. Myositis-specific autoantibodies help define homogeneous subgroups with common clinical characteristics and prognoses. Anti-SAE (small ubiquitin-like modifier 1 (SUMO-1) activating enzyme) antibodies are among the most recently discovered specific autoantibodies. The presence of these antibodies is very rare, making it challenging to define clinical features and prognosis in the juvenile form. We report the first case of an African patient with juvenile dermatomyositis and positive anti-SAE antibodies.
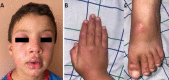
Case report: A 5-year-3-month-old Moroccan boy presented to the pediatric emergency department with dysphagia that had been evolving for two days, preceded two months earlier by facial erythema associated with fatigue, lower limb pain, difficulty walking, and progressive inflammatory polyarthralgia. On admission, the child had a heliotrope rash with predominant pseudo-angioedema on the lips, periungual telangiectasia, and Gottron's papules over the bilateral interphalangeal and metatarsophalangeal joints. The patient had a more pronounced proximal muscle weakness in the lower limbs. He had no urticaria, fever, arthritis, calcinosis, cutaneous ulcers, or lipodystrophy. The Joint examination was normal, as was the pleuropulmonary examination. The electroneuromyography showed myogenic changes in all four limbs. Laboratory findings showed elevated levels of creatine phosphokinase and lactate dehydrogenase and a mild inflammatory syndrome. The electrocardiogram was normal. The anti-SAE antibodies were positive. The boy was diagnosed with juvenile dermatomyositis. He received methylprednisolone bolus therapy followed by oral prednisone. The latter was gradually tapered in combination with weekly intramuscular methotrexate. As a result, dysphagia disappeared within 48 h. After two weeks, there was an improvement in the muscular score and a significant regression of facial pseudo-angioedema.
Conclusion: We report the first African patient with anti-SAE autoantibody-positive JDM. He had a typical dermatological manifestation of JDM associated with pseudo-angioedema predominant on the lips; a rarely reported sign in DM and JDM patients. The patient responded well to corticosteroid therapy and methotrexate.
Keywords: Anti-SAE autoantibody; Juvenile dermatomyositis; Myositis-specific autoantibody; Pseudo-angioedema.
© 2024. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
Similar articles
-
Anti-SAE autoantibody-positive Japanese patient with juvenile dermatomyositis complicated with interstitial lung disease - a case report.Pediatr Rheumatol Online J. 2021 Mar 19;19(1):34. doi: 10.1186/s12969-021-00532-2. Pediatr Rheumatol Online J. 2021. PMID: 33740993 Free PMC article.
-
Juvenile dermatomyositis associated with autoantibodies to small ubiquitin-like modifier activating enzyme: a report of 4 cases from North India and a review of literature.Immunol Res. 2023 Feb;71(1):112-120. doi: 10.1007/s12026-022-09334-4. Epub 2022 Oct 24. Immunol Res. 2023. PMID: 36278969 Review.
-
A Case of Juvenile Dermatomyositis Presenting with Inverse Gottron's Papules: A Case Report.Case Rep Dermatol. 2025 Mar 11;17(1):80-85. doi: 10.1159/000544816. eCollection 2025 Jan-Dec. Case Rep Dermatol. 2025. PMID: 40161489 Free PMC article.
-
Low prevalence of anti-small ubiquitin-like modifier activating enzyme antibodies in dermatomyositis patients.Autoimmunity. 2013 Jun;46(4):279-84. doi: 10.3109/08916934.2012.755958. Epub 2013 Feb 8. Autoimmunity. 2013. PMID: 23215730
-
Juvenile Dermatomyositis: Advances in Pathogenesis, Assessment, and Management.Curr Pediatr Rev. 2021;17(4):273-287. doi: 10.2174/1573396317666210426105045. Curr Pediatr Rev. 2021. PMID: 33902423 Review.
Cited by
-
Pseudoangioedema as a presenting symptom of dermatomyositis with antinuclear matrix protein 2 autoantibodies.JAAD Case Rep. 2025 Jan 29;58:18-20. doi: 10.1016/j.jdcr.2024.12.018. eCollection 2025 Apr. JAAD Case Rep. 2025. PMID: 40099171 Free PMC article. No abstract available.
-
Juvenile Dermatomyositis in a Two-Year-Old Yemeni Girl in a Resource-Limited Setting: A Case Report.Cureus. 2025 Mar 10;17(3):e80376. doi: 10.7759/cureus.80376. eCollection 2025 Mar. Cureus. 2025. PMID: 40213710 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials