Clinical Practice Guideline: Microhematuria in Children and Young Adults
- PMID: 38775222
- PMCID: PMC11635810
- DOI: 10.3238/arztebl.m2024.0070
Clinical Practice Guideline: Microhematuria in Children and Young Adults
Abstract
Background: Occult blood in the urine, or microhematuria, is a common finding (about 10%) in children and young adults. It is often of brief duration and therefore harmless. In persistent microhematuria, acanthocytes in the urine are a frequently unrecognized early marker of glomerular kidney disease. The purpose of this guideline is to promote the early detection of kidney disease in children and young adults with practical, evidence-based recommendations.
Methods: A systematic search for pertinent publications up to January 2023 was conducted in Pubmed, the Cochrane Database, and Livivo. 474 publications were retrieved, summarized in terms of method and content, and classified by Oxford (2011) evidence level.
Results: Approximately 1% of children and young adults have undiagnosed chronic kidney disease. Microhematuria is an early warning sign. A timely nephrological evaluation is indicated if microhematuria persists for 3 to 6 months, if ≥ 5% acanthocytes are detectable in the urine, and if there is also proteinuria, hypertension, or impaired renal function. Ultrasonography of the kidneys and urinary tract is the imaging method of choice; cystoscopy should be avoided. For patients with glomerular microhematuria, molecular genetic testing is recommended. Renal biopsy is recommended in case of florid glomerular diseases, after the determination of various laboratory param eters and clinical findings, including molecular genet ic testing especially in children.
Conclusion: In the absence of a guideline until now, findings have often been incorrectly assessed, leading either to an inadequate work-up or to excessive diagnostics. As a result, in approximately 30% of young patients, valuable opportunities for early treatment to protect the kidneys have been missed.
Figures
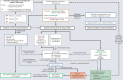

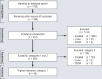
References
-
- Gross O, Licht C, Anders HJ, et al. Early angiotensin-converting enzyme inhibition in Alport syndrome delays renal failure and improves life expectancy. Kidney Int. 2012;81:494–501. - PubMed
-
- Kashtan CE, Gross O. Clinical practice recommendations for the diagnosis and management of Alport syndrome in children, adolescents, and young adults. Pediatr Nephrol. 2021;36:711–719. - PubMed
-
- Calderon-Margalit R, Golan E, Twig G, et al. History of childhood kidney disease and risk of adult end-stage renal disease. N Engl J Med. 2018;378:428–438. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials

