Can left atrial diameter measured by computed tomography predict the presence and degree of left ventricular diastolic dysfunction?
- PMID: 38778493
- PMCID: PMC11700690
- DOI: 10.15441/ceem.24.194
Can left atrial diameter measured by computed tomography predict the presence and degree of left ventricular diastolic dysfunction?
Abstract
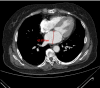
Objective: This study was conducted to determine whether the presence and degree of left ventricular diastolic dysfunction (LVDD) can be predicted by the simple computed tomography -measured left atrial diameter (CTLAD).
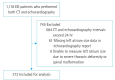
Methods: Among adult patients who underwent both chest CT imaging and echocardiography in the emergency department from January 2020 to December 2021, a retrospective cross-sectional study enrolled patients in whom the time interval between the two tests was <24 hours. Receiver operating characteristic (ROC) curve analysis was used to evaluate the diagnostic power of CTLAD for echocardiographic LVDD.
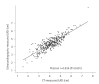
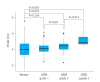
Results: In a study involving 373 patients, 192 (51.5%) had LVDD. Among them, 122 (63.5%) had grade 1, 61 (31.8%) had grade 2, and nine (4.7%) had ≥grade 3. Median CTLAD values were 4.1 cm for grade 1, 4.5 cm for grade 2, and 4.9 cm for ≥grade 3. The area under the ROC curve value of CTLAD in distinguishing ≥grade 1, ≥grade 2 (optimal cutoff ≥4.4 cm), and ≥grade 3 (optimal cutoff ≥4.5 cm) were 0.588, 0.657 (sensitivity, 61.4%; specificity, 66.0%, positive predictive value, 29.5%; negative predictive value, 88.1%; odds ratio, 3.1), and 0.834 (sensitivity, 88.9%; specificity, 70.1%; positive predictive value, 6.8%; negative predictive value, 99.6%, odds ratio, 18.7), respectively.
Conclusion: CTLAD ≥4.4 cm can be used as a rough reference value to distinguish LVDD of ≥grade 2, while CTLAD ≥4.5 cm can reliably distinguish LVDD of ≥grade 3. CTLAD might be a useful parameter for predicting LVDD in situations where echocardiography is not available.
Keywords: Computed tomography; Diastolic heart failure; Echocardiography; Left atrium; Left ventricular dysfunction.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures

Similar articles
-
Left Atrial Strain as a Single Parameter to Predict Left Ventricular Diastolic Dysfunction and Elevated Left Ventricular Filling Pressure in Patients Undergoing Off-Pump Coronary Artery Bypass Grafting.J Cardiothorac Vasc Anesth. 2021 Jun;35(6):1618-1625. doi: 10.1053/j.jvca.2020.11.066. Epub 2020 Dec 9. J Cardiothorac Vasc Anesth. 2021. PMID: 33384229
-
High-sensitive cardiac troponin T: a biomarker of left-ventricular diastolic dysfunction in hemodialysis patients.J Nephrol. 2018 Dec;31(6):967-973. doi: 10.1007/s40620-018-0540-0. Epub 2018 Oct 22. J Nephrol. 2018. PMID: 30350298
-
Prognostic significance of diastolic dysfunction in patients with systolic dysfunction undergoing atrial fibrillation ablation.Int J Cardiol Heart Vasc. 2022 Jul 4;41:101079. doi: 10.1016/j.ijcha.2022.101079. eCollection 2022 Aug. Int J Cardiol Heart Vasc. 2022. PMID: 35812132 Free PMC article.
-
Left ventricular end-diastolic diameter is an independent predictor of mortality in hemodialysis patients.Ther Apher Dial. 2012 Apr;16(2):134-41. doi: 10.1111/j.1744-9987.2011.01048.x. Epub 2012 Feb 2. Ther Apher Dial. 2012. PMID: 22458391
-
Left Atrial Structure and Function, and Left Ventricular Diastolic Dysfunction: JACC State-of-the-Art Review.J Am Coll Cardiol. 2019 Apr 23;73(15):1961-1977. doi: 10.1016/j.jacc.2019.01.059. J Am Coll Cardiol. 2019. PMID: 31000000 Review.
Cited by
-
Development and validation of a predictive model for cancer therapy-related cardiac dysfunction in breast cancer patients using echocardiographic indicators.Am J Cancer Res. 2025 May 15;15(5):2243-2258. doi: 10.62347/WPUW2205. eCollection 2025. Am J Cancer Res. 2025. PMID: 40520878 Free PMC article.
References
-
- Federmann M, Hess OM. Differentiation between systolic and diastolic dysfunction. Eur Heart J. 1994;15 Suppl D:2–6. - PubMed
-
- Kindermann M. How to diagnose diastolic heart failure: a consensus statement on the diagnosis of heart failure with normal left ventricular ejection fraction by the Heart Failure and Echocardiography Associations of the European Society of Cardiology. Eur Heart J. 2007;28:2686. - PubMed
-
- Vasan RS, Levy D. Defining diastolic heart failure: a call for standardized diagnostic criteria. Circulation. 2000;101:2118–21. - PubMed
LinkOut - more resources
Full Text Sources

