Usefulness of Impulse Oscillometry in Predicting the Severity of Bronchiectasis
- PMID: 38783483
- PMCID: PMC11222088
- DOI: 10.4046/trd.2023.0160
Usefulness of Impulse Oscillometry in Predicting the Severity of Bronchiectasis
Abstract
Background: Bronchiectasis is a chronic respiratory disease that leads to airway inflammation, destruction, and airflow limitation, which reflects its severity. Impulse oscillometry (IOS) is a non-invasive method that uses sound waves to estimate lung function and airway resistance. The aim of this study was to assess the usefulness of IOS in predicting the severity of bronchiectasis.
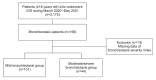
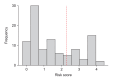
Methods: We retrospectively reviewed the IOS parameters and clinical characteristics in 145 patients diagnosed with bronchiectasis between March 2020 and May 2021. Disease severity was evaluated using the FACED score, and patients were divided into mild and moderate/severe groups.
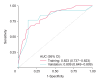
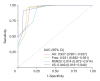
Results: Forty-four patients (30.3%) were in the moderate/severe group, and 101 (69.7%) were in the mild group. Patients with moderate/severe bronchiectasis had a higher airway resistance at 5 Hz (R5), a higher difference between the resistance at 5 and 20 Hz (R5-R20), a higher resonant frequency (Fres), and a higher area of reactance (AX) than patients with mild bronchiectasis. R5 ≥0.43, resistance at 20 Hz (R20) ≥0.234, R5-R20 ≥28.3, AX ≥1.02, reactance at 5 Hz (X5) ≤-0.238, and Fres ≥20.88 revealed significant univariable relationships with bronchiectasis severity (p<0.05). Among these, only X5 ≤-0.238 exhibited a significant multivariable relationship with bronchiectasis severity (p=0.039). The receiver operating characteristic curve for predicting moderate- to-severe bronchiectasis of FACED score based on IOS parameters exhibited an area under the curve of 0.809.
Conclusion: The IOS assessed by the disease severity of FACED score can effectively reflect airway resistance and elasticity in bronchiectasis patients and serve as valuable tools for predicting bronchiectasis severity.
Keywords: Bronchiectasis; Disease Severity; Impulse Oscillometry.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures

Similar articles
-
The Role of Impulse Oscillometry in Evaluating Disease Severity and Predicting the Airway Reversibility in Patients With Bronchiectasis.Front Med (Lausanne). 2022 Feb 25;9:796809. doi: 10.3389/fmed.2022.796809. eCollection 2022. Front Med (Lausanne). 2022. PMID: 36687424 Free PMC article.
-
Comparative evaluation of expiratory airflow limitation between patients with COPD and BE using IOS.Sci Rep. 2021 Feb 25;11(1):4524. doi: 10.1038/s41598-021-84028-9. Sci Rep. 2021. PMID: 33633234 Free PMC article.
-
Application Value of Broadband 3-Dimensional Impulse Oscillometry in COPD.Int J Chron Obstruct Pulmon Dis. 2021 Feb 4;16:215-223. doi: 10.2147/COPD.S285927. eCollection 2021. Int J Chron Obstruct Pulmon Dis. 2021. PMID: 33574662 Free PMC article.
-
What can we learn about COPD from impulse oscillometry?Respir Med. 2018 Jun;139:106-109. doi: 10.1016/j.rmed.2018.05.004. Epub 2018 May 16. Respir Med. 2018. PMID: 29857993 Review.
-
Exploring Pulmonary Dysfunction in Parkinson's Disease: The Role of Impulse Oscillometry-A Systematic Review.J Clin Med. 2025 May 26;14(11):3730. doi: 10.3390/jcm14113730. J Clin Med. 2025. PMID: 40507493 Free PMC article. Review.
References
-
- Chalmers JD, Chang AB, Chotirmall SH, Dhar R, McShane PJ. Bronchiectasis. Nat Rev Dis Primers. 2018;4:45. - PubMed
-
- Choi H, Yang B, Nam H, Kyoung DS, Sim YS, Park HY, et al. Population-based prevalence of bronchiectasis and associated comorbidities in South Korea. Eur Respir J. 2019;54:1900194. - PubMed
-
- Chalmers JD, Aliberti S, Filonenko A, Shteinberg M, Goeminne PC, Hill AT, et al. Characterization of the “frequent exacerbator phenotype” in bronchiectasis. Am J Respir Crit Care Med. 2018;197:1410–20. - PubMed

