Evaluation of the Effect of Morphological Structure on Dilatational Tracheostomy Interference Location and Complications with Ultrasonography and Fiberoptic Bronchoscopy
- PMID: 38792330
- PMCID: PMC11122435
- DOI: 10.3390/jcm13102788
Evaluation of the Effect of Morphological Structure on Dilatational Tracheostomy Interference Location and Complications with Ultrasonography and Fiberoptic Bronchoscopy
Abstract
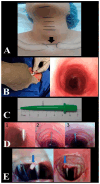
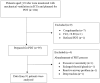
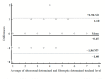
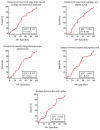
Background: Percutaneous dilatational tracheostomy (PDT) is the most commonly performed minimally invasive intensive care unit procedure worldwide. Methods: This study evaluated the percentage of consistency between the entry site observed with fiberoptic bronchoscopy (FOB) and the prediction for the PDT level based on pre-procedural ultrasonography (USG) in PDT procedures performed using the forceps dilatation method. The effect of morphological features on intervention sites was also investigated. Complications that occurred during and after the procedure, as well as the duration, site, and quantity of the procedures, were recorded. Results: Data obtained from a total of 91 patients were analyzed. In 57 patients (62.6%), the USG-estimated tracheal puncture level was consistent with the intercartilaginous space observed by FOB, while in 34 patients (37.4%), there was a discrepancy between these two methods. According to Bland Altman, the agreement between the tracheal spaces determined by USG and FOB was close. Regression formulas for PDT procedures defining the intercartilaginous puncture level based on morphologic measurements of the patients were created. The most common complication related to PDT was cartilage fracture (17.6%), which was proven to be predicted with maximum relevance by punctured tracheal level, neck extension limitation, and procedure duration. Conclusions: In PDT procedures using the forceps dilatation method, the prediction of the PDT intervention level based on pre-procedural USG was considerably in accordance with the entry site observed by FOB. The intercartilaginous puncture level could be estimated based on morphological measurements.
Keywords: complications; fiberoptic bronchoscopy; morphology; percutaneous dilatational tracheostomy; ultrasonography.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures

Similar articles
-
Percutaneous dilatational tracheostomy versus fibre optic bronchoscopy-guided percutaneous dilatational tracheostomy in critically ill patients: a randomised controlled trial.Ir J Med Sci. 2019 May;188(2):675-681. doi: 10.1007/s11845-018-1881-3. Epub 2018 Aug 11. Ir J Med Sci. 2019. PMID: 30099716 Clinical Trial.
-
Comparison of the percutaneous dilatational tracheostomy with and without flexible bronchoscopy guidance in intensive care units.BMC Anesthesiol. 2025 Mar 31;25(1):142. doi: 10.1186/s12871-025-03022-0. BMC Anesthesiol. 2025. PMID: 40165086 Free PMC article.
-
Comparison of Bronchoscopy-Guided and Real-Time Ultrasound-Guided Percutaneous Dilatational Tracheostomy: Safety, Complications, and Effectiveness in Critically Ill Patients.J Intensive Care Med. 2019 Mar;34(3):191-196. doi: 10.1177/0885066617705641. Epub 2017 Apr 27. J Intensive Care Med. 2019. PMID: 28446075
-
Ultrasound-Guided Percutaneous Dilational Tracheostomy: A Systematic Review of Randomized Controlled Trials and Meta-Analysis.J Intensive Care Med. 2020 May;35(5):445-452. doi: 10.1177/0885066618755334. Epub 2018 Feb 7. J Intensive Care Med. 2020. PMID: 29409380
-
Percutaneous tracheostomy.Ann Card Anaesth. 2017 Jan;20(Supplement):S19-S25. doi: 10.4103/0971-9784.197793. Ann Card Anaesth. 2017. PMID: 28074819 Free PMC article. Review.
References
LinkOut - more resources
Full Text Sources

