The potential mechanism of treating IC/BPS with hyperbaric oxygen by reducing vascular endothelial growth inhibitor and hypoxia-inducible factor-1α
- PMID: 38812622
- PMCID: PMC11031152
- DOI: 10.55730/1300-0144.5762
The potential mechanism of treating IC/BPS with hyperbaric oxygen by reducing vascular endothelial growth inhibitor and hypoxia-inducible factor-1α
Abstract
Background/aim: To investigate the roles of vascular endothelial growth inhibitor (VEGI) and hypoxia-inducible factor-1α (HIF-1α) in the treatment of refractory interstitial cystitis/bladder pain syndrome (IC/BPS) with hyperbaric oxygen (HBO).
Materials and methods: A total of 38 patients were included. They were assessed before and 6 months after HBO treatment. Three-day voiding diaries were recorded, and O'leary-Sant scores, visual analog scale (VAS) scores, quality of life (QoL) scores, pelvic pain, and urgency/frequency (PUF) scores were evaluated. Bladder capacity was assessed by cystoscopy. Bladder mucosa was collected for Western blot, qRT-PCR, and immunofluorescence staining to compare the expression of VEGI and HIF-1α before and after treatment.
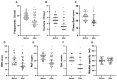
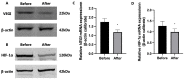
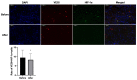
Results: Compared with before treatment, patients showed significant improvements in 24-h voiding frequency (15.32 ± 5.38 times), nocturia (3.71 ± 1.80 times), O'leary-Sant score (20.45 ± 5.62 points), VAS score (41.76 ± 17.88 points), QoL score (3.03 ± 1.44 points), and PUF score (19.95 ± 6.46 points) after treatment (p < 0.05). There was no significant difference in bladder capacity before and after treatment (p ≥ 0.05). The expression levels of VEGI and HIF-1α protein and mRNA were significantly decreased 6 months after treatment compared with before treatment. Immunofluorescence staining results showed that the double positive expression of VEGI and HIF-1α protein in bladder tissue of IC/BPS patients after HBO treatment quantitatively decreased significantly.
Conclusion: This study identified a possible mechanism by which VEGI and HIF-1α expression decreased after HBO treatment due to hypoxia reversal, which improved symptoms in IC/BPS patients.
Keywords: Interstitial cystitis/bladder pain syndrome; hyperbaric oxygen; hypoxia-inducible factor-1α; vascular endothelial growth inhibitor.
© TÜBİTAK.
Conflict of interest statement
Conflict of interest: The authors declare they have no conflicts of interest associated with this study.
Figures
Similar articles
-
Increased Transient Receptor Potential Melastatin 8 Expression in the Development of Bladder Pain in Patients With Interstitial Cystitis/Bladder Pain Syndrome.Urology. 2020 Dec;146:301.e1-301.e6. doi: 10.1016/j.urology.2020.09.037. Epub 2020 Oct 10. Urology. 2020. PMID: 33045289
-
Angiogenesis in bladder tissues is strongly correlated with urinary frequency and bladder pain in patients with interstitial cystitis/bladder pain syndrome.Int J Urol. 2019 Jun;26 Suppl 1:35-40. doi: 10.1111/iju.13972. Int J Urol. 2019. PMID: 31144750
-
Effects of electroacupuncture on refractory interstitial cystitis/bladder pain syndrome: A one-year follow-up case report.Explore (NY). 2024 Jul-Aug;20(4):602-605. doi: 10.1016/j.explore.2023.12.001. Epub 2023 Dec 6. Explore (NY). 2024. PMID: 38072764
-
Current status of patient-reported outcome measures and other subjective assessment grading tools in bladder pain syndrome.Int Urogynecol J. 2023 Aug;34(8):1677-1687. doi: 10.1007/s00192-023-05551-z. Epub 2023 May 2. Int Urogynecol J. 2023. PMID: 37129626 Review.
-
The integration of biomarkers and patient-reported outcomes improves prediction of interstitial cystitis syndrome.Expert Rev Mol Diagn. 2025 Jun;25(6):217-232. doi: 10.1080/14737159.2025.2502035. Epub 2025 May 6. Expert Rev Mol Diagn. 2025. PMID: 40319375 Review.
Cited by
-
Hypoxic ischemic encephalopathy (HIE).Front Neurol. 2024 Jul 23;15:1389703. doi: 10.3389/fneur.2024.1389703. eCollection 2024. Front Neurol. 2024. PMID: 39108657 Free PMC article. Review.
References
-
- Bendrick TR, Sitenga GL, Booth C, Sacco MP, Erie C, et al. The implications of mental health and trauma in interstitial cystitis. Health Psychology Research. 2022;10(4):40321. https://doi:10.52965/001c.40321 . - DOI - PMC - PubMed
-
- Tamaki M, Saito R, Ogawa O, Yoshimura N, Ueda T. Possible mechanisms inducing glomerulations in interstitial cystitis: relationship between endoscopic findings and expression of angiogenic growth factors. Journal of Urology. 2004;172(3):945–948. https://doi:10.1097/01.ju.0000135009.55905.cb . - DOI - PubMed
-
- Jiang YH, Jhang JF, Ho HC, Chiou DY, Kuo HC. Urine oxidative stress biomarkers as novel biomarkers in interstitial cystitis/bladder pain syndrome. Biomedicines. 2022;10(7):1701. https://doi:10.3390/biomedicines10071701 . - DOI - PMC - PubMed
-
- Cox A, Golda N, Nadeau G, Curtis NJ, Carr L, et al. CUA guideline: Diagnosis and treatment of interstitial cystitis/bladder pain syndrome. Canadian Urological Association Journal. 2016;10(5–6):E136–E155. https://doi:10.5489/cuaj.3786 . - DOI - PMC - PubMed
-
- Minami A, Tanaka T, Otoshi T, Kuratsukuri K, Nakatani T. Hyperbaric oxygen significantly improves frequent urination, hyperalgesia, and tissue damage in a mouse long-lasting cystitis model induced by an intravesical instillation of hydrogen peroxide. Neurourology and Urodynamics. 2019;38(1):97–106. https://doi:10.1002/nau.23822 . - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

