Drug-resistant oral candidiasis in patients with HIV infection: a systematic review and meta-analysis
- PMID: 38822256
- PMCID: PMC11143751
- DOI: 10.1186/s12879-024-09442-6
Drug-resistant oral candidiasis in patients with HIV infection: a systematic review and meta-analysis
Abstract
Background: Oral candidiasis (OC) is a prevalent opportunistic infection in patients with human immunodeficiency virus (HIV) infection. The increasing resistance to antifungal agents in HIV-positive individuals suffering from OC raised concerns. Thus, this study aimed to investigate the prevalence of drug-resistant OC in HIV-positive patients.
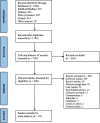
Methods: Pubmed, Web of Science, Scopus, and Embase databases were systematically searched for eligible articles up to November 30, 2023. Studies reporting resistance to antifungal agents in Candida species isolated from HIV-positive patients with OC were included. Baseline characteristics, clinical features, isolated Candida species, and antifungal resistance were independently extracted by two reviewers. The pooled prevalence with a 95% confidence interval (CI) was calculated using the random effect model or fixed effect model.
Results: Out of the 1942 records, 25 studies consisting of 2564 Candida species entered the meta-analysis. The pooled prevalence of resistance to the antifungal agents was as follows: ketoconazole (25.5%, 95% CI: 15.1-35.8%), fluconazole (24.8%, 95% CI: 17.4-32.1%), 5-Flucytosine (22.9%, 95% CI: -13.7-59.6%), itraconazole (20.0%, 95% CI: 10.0-26.0%), voriconazole (20.0%, 95% CI: 1.9-38.0%), miconazole (15.0%, 95% CI: 5.1-26.0%), clotrimazole (13.4%, 95% CI: 2.3-24.5%), nystatin (4.9%, 95% CI: -0.05-10.3%), amphotericin B (2.9%, 95% CI: 0.5-5.3%), and caspofungin (0.1%, 95% CI: -0.3-0.6%). Furthermore, there were high heterogeneities among almost all included studies regarding the resistance to different antifungal agents (I2 > 50.00%, P < 0.01), except for caspofungin (I2 = 0.00%, P = 0.65).
Conclusions: Our research revealed that a significant number of Candida species found in HIV-positive patients with OC were resistant to azoles and 5-fluocytosine. However, most of the isolates were susceptible to nystatin, amphotericin B, and caspofungin. This suggests that initial treatments for OC, such as azoles, may not be effective. In such cases, healthcare providers may need to consider prescribing alternative treatments like polyenes and caspofungin.
Registration: The study protocol was registered in the International Prospective Register of Systematic Reviews as PROSPERO (Number: CRD42024497963).
Keywords: Candida; Drug Resistance; HIV; Opportunistic infections; Oral candidiasis.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
Cross-sectional study of the susceptibility of Candida isolates to antifungal drugs and in vitro-in vivo correlation in HIV-infected patients.AIDS. 1994 Jul;8(7):945-50. doi: 10.1097/00002030-199407000-00011. AIDS. 1994. PMID: 7946104
-
Iranian HIV/AIDS patients with oropharyngeal candidiasis: identification, prevalence and antifungal susceptibility of Candida species.Lett Appl Microbiol. 2018 Oct;67(4):392-399. doi: 10.1111/lam.13052. Epub 2018 Aug 16. Lett Appl Microbiol. 2018. PMID: 30019443
-
Are Candida albicans isolates from people living with HIV more resistant to antifungals? A systematic review and meta-analysis.Microb Pathog. 2025 Oct;207:107913. doi: 10.1016/j.micpath.2025.107913. Epub 2025 Jul 15. Microb Pathog. 2025. PMID: 40675507
-
The prevalence, risk factors and antifungal sensitivity pattern of oral candidiasis in HIV/AIDS patients in Kumba District Hospital, South West Region, Cameroon.Pan Afr Med J. 2020 May 19;36:23. doi: 10.11604/pamj.2020.36.23.18202. eCollection 2020. Pan Afr Med J. 2020. PMID: 32774600 Free PMC article.
-
Therapeutic options for the management of oropharyngeal and esophageal candidiasis in HIV/AIDS patients.HIV Clin Trials. 2000 Jul-Aug;1(1):47-59. doi: 10.1310/T7A7-1E63-2KA0-JKWD. HIV Clin Trials. 2000. PMID: 11590489 Review.
Cited by
-
Copper-Induced Stimulation of Ectophosphatase Activity of Candida albicans.Pathogens. 2025 Jul 8;14(7):667. doi: 10.3390/pathogens14070667. Pathogens. 2025. PMID: 40732714 Free PMC article.
-
Prevalence, associated factors and etiologic agents of oral candidiasis among HIV-positive patients in a Vietnamese general hospital.Curr Med Mycol. 2024 Dec 31;10:e2025.345307.1583. doi: 10.22034/cmm.2025.345307.1583. eCollection 2024. Curr Med Mycol. 2024. PMID: 40662152 Free PMC article.
-
Non-Pharmacological Interventions to Prevent Oropharyngeal Candidiasis in Patients Using Inhaled Corticosteroids: A Narrative Review.Healthcare (Basel). 2025 Jul 17;13(14):1718. doi: 10.3390/healthcare13141718. Healthcare (Basel). 2025. PMID: 40724743 Free PMC article. Review.
References
-
- Mardani M, Abolghasemi S, Darvishnia D, Lotfali E, Ghasemi R, Rabiei MM, et al. Oral candidiasis in hematological malignancy patients: identification and antifungal susceptibility patterns of isolates. Jundishapur J Microbiol. 2020;13(8):e103290.
-
- Mushi MF, Bader O, Taverne-Ghadwal L, Bii C, Groß U, Mshana SE. Oral candidiasis among African human immunodeficiency virus-infected individuals: 10 years of systematic review and meta-analysis from Sub-saharan Africa. J oral Microbiol. 2017;9(1):1317579. doi: 10.1080/20002297.2017.1317579. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical