High stress hyperglycemia ratio predicts adverse clinical outcome in patients with coronary three-vessel disease: a large-scale cohort study
- PMID: 38824608
- PMCID: PMC11144339
- DOI: 10.1186/s12933-024-02286-z
High stress hyperglycemia ratio predicts adverse clinical outcome in patients with coronary three-vessel disease: a large-scale cohort study
Abstract
Background: Coronary three-vessel disease (CTVD) accounts for one-third of the overall incidence of coronary artery disease, with heightened mortality rates compared to single-vessel lesions, including common trunk lesions. Dysregulated glucose metabolism exacerbates atherosclerosis and increases cardiovascular risk. The stress hyperglycemia ratio (SHR) is proposed as an indicator of glucose metabolism status but its association with cardiovascular outcomes in CTVD patients undergoing percutaneous coronary intervention (PCI) remains unclear.
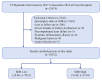
Methods: 10,532 CTVD patients undergoing PCI were consecutively enrolled. SHR was calculated using the formula: admission blood glucose (mmol/L)/[1.59×HbA1c (%)-2.59]. Patients were divided into two groups (SHR Low and SHR High) according to the optimal cutoff value of SHR. Multivariable Cox regression models were used to assess the relationship between SHR and long-term prognosis. The primary endpoint was cardiovascular (CV) events, composing of cardiac death and non-fatal myocardial infarction (MI).
Results: During the median follow-up time of 3 years, a total of 279 cases (2.6%) of CV events were recorded. Multivariable Cox analyses showed that high SHR was associated with a significantly higher risk of CV events [Hazard Ratio (HR) 1.99, 95% Confidence interval (CI) 1.58-2.52, P < 0.001). This association remained consistent in patients with (HR 1.50, 95% CI 1.08-2.10, P = 0.016) and without diabetes (HR 1.97, 95% CI 1.42-2.72, P < 0.001). Additionally, adding SHR to the base model of traditional risk factors led to a significant improvement in the C-index, net reclassification and integrated discrimination.
Conclusions: SHR was a significant predictor for adverse CV outcomes in CTVD patients with or without diabetes, which suggested that it could aid in the risk stratification in this particular population regardless of glucose metabolism status.
Keywords: Coronary artery disease; Coronary three-vessel disease; Prognosis; Stress hyperglycemia ratio.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures



Similar articles
-
Association of stress hyperglycemia ratio with short-term and long-term prognosis in patients undergoing coronary artery bypass grafting across different glucose metabolism states: a large-scale cohort study.Cardiovasc Diabetol. 2025 Apr 24;24(1):179. doi: 10.1186/s12933-025-02682-z. Cardiovasc Diabetol. 2025. PMID: 40275310 Free PMC article.
-
Relationship between stress hyperglycaemic ratio (SHR) and critical illness: a systematic review.Cardiovasc Diabetol. 2025 May 2;24(1):188. doi: 10.1186/s12933-025-02751-3. Cardiovasc Diabetol. 2025. PMID: 40317019 Free PMC article.
-
Effects of the stress hyperglycemia ratio on long-term mortality in patients with triple-vessel disease and acute coronary syndrome.Cardiovasc Diabetol. 2024 Apr 25;23(1):143. doi: 10.1186/s12933-024-02220-3. Cardiovasc Diabetol. 2024. PMID: 38664806 Free PMC article.
-
Prognostic Significance of Relative Hyperglycemia after Percutaneous Coronary Intervention in Patients with and without Recognized Diabetes.Curr Vasc Pharmacol. 2021;19(1):91-101. doi: 10.2174/1570161118666200317145540. Curr Vasc Pharmacol. 2021. PMID: 32183677
-
The association between the stress hyperglycaemia ratio and mortality in cardiovascular disease: a meta-analysis and systematic review.Cardiovasc Diabetol. 2024 Nov 16;23(1):412. doi: 10.1186/s12933-024-02454-1. Cardiovasc Diabetol. 2024. PMID: 39550575 Free PMC article.
Cited by
-
Association of stress hyperglycemia ratio with short-term and long-term prognosis in patients undergoing coronary artery bypass grafting across different glucose metabolism states: a large-scale cohort study.Cardiovasc Diabetol. 2025 Apr 24;24(1):179. doi: 10.1186/s12933-025-02682-z. Cardiovasc Diabetol. 2025. PMID: 40275310 Free PMC article.
-
Retrospective Analysis of Gut Microbiota and Metabolomic Profiles in Pregnant Women: Association with Cesarean Section Risk.Int J Womens Health. 2025 Jun 12;17:1763-1770. doi: 10.2147/IJWH.S526040. eCollection 2025. Int J Womens Health. 2025. PMID: 40530360 Free PMC article.
-
SGLT2 Inhibitors: From Structure-Effect Relationship to Pharmacological Response.Int J Mol Sci. 2025 Jul 19;26(14):6937. doi: 10.3390/ijms26146937. Int J Mol Sci. 2025. PMID: 40725186 Free PMC article. Review.
-
Relationship between stress hyperglycaemic ratio (SHR) and critical illness: a systematic review.Cardiovasc Diabetol. 2025 May 2;24(1):188. doi: 10.1186/s12933-025-02751-3. Cardiovasc Diabetol. 2025. PMID: 40317019 Free PMC article.
-
Predictive factors for multivessel disease in patients with acute coronary syndrome: analysis from the CCC-ACS project in China.BMC Cardiovasc Disord. 2024 Nov 4;24(1):617. doi: 10.1186/s12872-024-04300-4. BMC Cardiovasc Disord. 2024. PMID: 39497069 Free PMC article.
References
-
- D’Ascenzo F, Presutti DG, Picardi E, Moretti C, Omede P, Sciuto F, et al. Prevalence and non-invasive predictors of left main or three-vessel coronary disease: evidence from a collaborative international meta-analysis including 22 740 patients. Heart. 2012;98(12):914–9. doi: 10.1136/heartjnl-2011-301596. - DOI - PubMed
-
- Thuijs D, Kappetein AP, Serruys PW, Mohr FW, Morice MC, Mack MJ, et al. Percutaneous coronary intervention versus coronary artery bypass grafting in patients with three-vessel or left main coronary artery disease: 10-year follow-up of the multicentre randomised controlled SYNTAX trial. Lancet. 2019;394(10206):1325–34. doi: 10.1016/S0140-6736(19)31997-X. - DOI - PubMed
-
- Guo L, Wang J, Ding H, Meng S, Zhang X, Lv H, et al. Long-term outcomes of medical therapy versus successful recanalisation for coronary chronic total occlusions in patients with and without type 2 diabetes mellitus. Cardiovasc Diabetol. 2020;19(1):100. doi: 10.1186/s12933-020-01087-4. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

