Spinopelvic Motion: A Simplified Approach to a Complex Subject
- PMID: 38825817
- PMCID: PMC11162876
- DOI: 10.5371/hp.2024.36.2.77
Spinopelvic Motion: A Simplified Approach to a Complex Subject
Abstract
Knowledge of the relationship between the hip and spine is essential in the effort to minimize instability and improve outcomes following total hip arthroplasty (THA). A detailed yet straightforward preoperative imaging workup can provide valuable information on pelvic positioning, which may be helpful for optimum placement of the acetabular cup. For a streamlined preoperative assessment of THA candidates, classification systems with a capacity for providing a more personalized approach to performance of THA have been introduced. Familiarity with these systems and their clinical application is important in the effort to optimize component placement and reduce the risk of instability. Looking ahead, the principles of the hip-spine relationship are being integrated using emerging innovative technologies, promising further streamlining of the evaluation process.
Keywords: Arthroplasty; Hip; Spinal curvatures; Spine; Spinopelvic mobility.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures

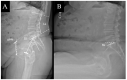

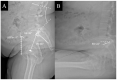
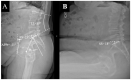
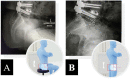


Similar articles
-
The Hip-Spine Relationship in Total Hip Arthroplasty: How to Execute the Plan.J Arthroplasty. 2021 Jul;36(7S):S111-S120. doi: 10.1016/j.arth.2021.01.008. Epub 2021 Jan 11. J Arthroplasty. 2021. PMID: 33526398
-
Does obesity affect acetabular cup position, spinopelvic function and sagittal spinal alignment? A prospective investigation with standing and sitting assessment of primary hip arthroplasty patients.J Orthop Surg Res. 2021 Oct 26;16(1):640. doi: 10.1186/s13018-021-02716-8. J Orthop Surg Res. 2021. PMID: 34702301 Free PMC article.
-
A Preoperative Workup of a "Hip-Spine" Total Hip Arthroplasty Patient: A Simplified Approach to a Complex Problem.J Arthroplasty. 2019 Jul;34(7S):S57-S70. doi: 10.1016/j.arth.2019.01.012. Epub 2019 Jan 18. J Arthroplasty. 2019. PMID: 30755374
-
Acetabular cup positioning in primary routine total hip arthroplasty-a review of current concepts and technologies.Arthroplasty. 2023 Dec 1;5(1):59. doi: 10.1186/s42836-023-00213-3. Arthroplasty. 2023. PMID: 38037156 Free PMC article. Review.
-
Total Hip Instability and the Spinopelvic Link.Curr Rev Musculoskelet Med. 2020 Aug;13(4):425-434. doi: 10.1007/s12178-020-09648-6. Curr Rev Musculoskelet Med. 2020. PMID: 32524531 Free PMC article. Review.
Cited by
-
Anterior Hip Dislocation Following Total Hip Arthroplasty, Caused by Broken Trial Femoral Head Particles: A Case Report.J Orthop Case Rep. 2025 Mar;15(3):76-79. doi: 10.13107/jocr.2025.v15.i03.5340. J Orthop Case Rep. 2025. PMID: 40092245 Free PMC article.
References
-
- Sloan M, Premkumar A, Sheth NP. Projected volume of primary total joint arthroplasty in the U.S., 2014 to 2030. J Bone Joint Surg Am. 2018;100:1455–60. doi: 10.2106/JBJS.17.01617. https://doi.org/10.2106/JBJS.17.01617. - DOI - PubMed
-
- Kurtz S, Ong K, Lau E, Mowat F, Halpern M. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;89:780–5. doi: 10.2106/JBJS.F.00222. https://doi.org/10.2106/JBJS.F.00222. - DOI - PubMed
-
- Singh JA, Yu S, Chen L, Cleveland JD. Rates of total joint replacement in the United States: future projections to 2020-2040 using the national inpatient sample. J Rheumatol. 2019;46:1134–40. doi: 10.3899/jrheum.170990. https://doi.org/10.3899/jrheum.170990. - DOI - PubMed
-
- Park JW, Won SH, Moon SY, Lee YK, Ha YC, Koo KH. Burden and future projection of revision Total hip Arthroplasty in South Korea. BMC Musculoskelet Disord. 2021;22:375. doi: 10.1186/s12891-021-04235-3. https://doi.org/10.1186/s12891-021-04235-3. - DOI - PMC - PubMed
-
- Gwam CU, Mistry JB, Mohamed NS, et al. Current epidemiology of revision Total Hip Arthroplasty in the United States: national inpatient sample 2009 to 2013. J Arthroplasty. 2017;32:2088–92. doi: 10.1016/j.arth.2017.02.046. https://doi.org/10.1016/j.arth.2017.02.046. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources

