Consumption of soya isoflavones improved polycystic ovary syndrome-associated metabolic disorders in a rat model
- PMID: 38826091
- PMCID: PMC11499085
- DOI: 10.1017/S0007114524001296
Consumption of soya isoflavones improved polycystic ovary syndrome-associated metabolic disorders in a rat model
Abstract
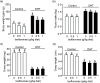
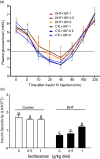
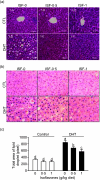
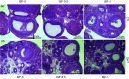
Polycystic ovary syndrome is associated with increased risks for certain metabolic disorders such as insulin resistance, non-alcoholic fatty liver disease and suppressed ovarian follicular development. This study aimed to examine whether soya isoflavones (ISF) mitigate these polycystic ovary syndrome-associated metabolic disorders in a rat model. Weanling Sprague-Dawley female rats were randomly divided into six groups and were treated with either 0 or 83 µg/d dihydrotestosterone (DHT) to induce polycystic ovary syndrome and fed diets containing 0, 0·5, or 1 g ISF/kg diet for 8 weeks. DHT treatment increased food intake, body weight gain (P < 0·001), percentage of primordial follicles (60 % v. 50·9 %, P < 0·05) and accumulation of lipid droplets in the livers. It also elevated serum total cholesterol, free cholesterol, TAG, NEFA and leptin and hepatic total cholesterol and NEFA. Additionally, DHT treatment reduced the percentage of primary follicles (13·8 % v. 30·2 %, P < 0·05), ovary weight and length (P < 0·001), as well as insulin sensitivity (P < 0·01) compared with the Control. ISF intake at 1 g/kg reduced body weight gain, serum total cholesterol, free cholesterol, NEFA, leptin and hepatic TAG and DHT-induced insulin resistance (P < 0·01). ISF intake at both levels decreased DHT-induced lipid droplet accumulation in the livers and changes in the percentages of primordial and primary follicles. Dietary soya ISF alleviated DHT-induced body weight gain, insulin resistance and hepatic lipid droplet accumulation, as well as suppressed ovarian follicular development. This suggests that the consumption of soya foods or ISF supplements may be beneficial for individuals with polycystic ovary syndrome, mitigating the associated metabolic disorders such as diabetes and non-alcoholic fatty liver disease.
Keywords: Insulin resistance; Non-alcoholic fatty liver disease; Polycystic ovary syndrome; Rat; Soya isoflavones.
Figures
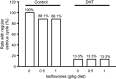
References
-
- Hoyt KL & Schmidt MC (2004) Polycystic ovary (Stein-Leventhal) syndrome: etiology, complications, and treatment. Clin Lab Sci 17, 155–163. - PubMed
-
- Paschou SA, Polyzos SA, Anagnostis P, et al. (2020) Nonalcoholic fatty liver disease in women with polycystic ovary syndrome. Endocrine 67, 1–8. - PubMed
-
- King J (2006) Polycystic ovary syndrome. J Midwifery Womens Health 51, 415–422. - PubMed
-
- Meier RK (2018) Polycystic ovary syndrome. Nurs Clin North Am 53, 407–420. - PubMed
LinkOut - more resources
Full Text Sources

