This is a preprint.
Comparative analysis of within-host dynamics of acute infection and viral rebound dynamics in postnatally SHIV-infected ART-treated infant rhesus macaques
- PMID: 38826467
- PMCID: PMC11142125
- DOI: 10.1101/2024.05.21.595130
Comparative analysis of within-host dynamics of acute infection and viral rebound dynamics in postnatally SHIV-infected ART-treated infant rhesus macaques
Update in
-
Assessing the impact of autologous virus neutralizing antibodies on viral rebound time in postnatally SHIV-infected ART-treated infant rhesus macaques.Epidemics. 2024 Sep;48:100780. doi: 10.1016/j.epidem.2024.100780. Epub 2024 Jun 27. Epidemics. 2024. PMID: 38964130 Free PMC article.
Abstract
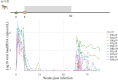
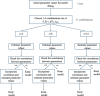
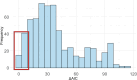
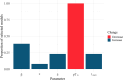
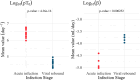
Viral dynamics of acute HIV infection and HIV rebound following suspension of antiretroviral therapy may be qualitatively similar but must differ given, for one, development of adaptive immune responses. Understanding the differences of acute HIV infection and viral rebound dynamics in pediatric populations may provide insights into the mechanisms of viral control with potential implications for vaccine design and the development of effective targeted therapeutics for infants and children. Mathematical models have been a crucial tool to elucidate the complex processes driving viral infections within the host. Traditionally, acute HIV infection has been modeled with a standard model of viral dynamics initially developed to explore viral decay during treatment, while viral rebound has necessitated extensions of that standard model to incorporate explicit immune responses. Previous efforts to fit these models to viral load data have underscored differences between the two infection stages, such as increased viral clearance rate and increased death rate of infected cells during rebound. However, these findings have been predicated on viral load measurements from disparate adult individuals. In this study, we aim to bridge this gap, in infants, by comparing the dynamics of acute infection and viral rebound within the same individuals by leveraging an infant nonhuman primate Simian/Human Immunodeficiency Virus (SHIV) infection model. Ten infant Rhesus macaques (RMs) orally challenged with SHIV.C.CH505 375H dCT and given ART at 8 weeks post-infection. These infants were then monitored for up to 60 months post-infection with serial viral load and immune measurements. We use the HIV standard viral dynamics model fitted to viral load measurements in a nonlinear mixed effects framework. We find that the primary difference between acute infection and rebound is the increased death rate of infected cells during rebound. We use these findings to generate hypotheses on the effects of adaptive immune responses. We leverage these findings to formulate hypotheses to elucidate the observed results and provide arguments to support the notion that delayed viral rebound is characterized by a stronger CD8+ T cell response.
Figures
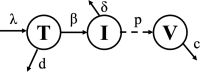
References
-
- WHO. HIV. World Health Organization, 2022. www.who.int/data/gho/data/themes/HIV-AIDS.
-
- UNAIDS. Global HIV & AIDS Statistics — Fact sheet. Available at: www.unaids.org/en/resources/fact-sheet, 2021. Accessed July 11 2022.
-
- Berendam SJ, Nelson AN, Yagnik B, Goswami R, Styles TM, Neja MA, Phan CT, Dankwa S, Byrd AU, Garrido C, Amara RR, Chahroudi A, Permar SR, and Fouda GG. Challenges and opportunities of therapies targeting early life immunity for pediatric HIV cure. Front. Immunol, 13:885272, 2022. doi: 10.3389/fimmu.2022.885272. - DOI - PMC - PubMed
-
- European Collaborative Study. Level and pattern of HIV-1-RNA viral load over age: differences between girls and boys? AIDS (London, England), 16(1):97–104, 2002. - PubMed
-
- HIV Paediatric Prognostic Markers Collaborative Study Group and others. Short-term risk of disease progression in HIV-1-infected children receiving no antiretroviral therapy or zidovudine monotherapy: a meta-analysis. The Lancet, 362(9396):1605–1611, 2003. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
