Management of cardiopulmonary bypass in patients with ischemic and hemorrhagic strokes in surgery for active infective endocarditis
- PMID: 38827558
- PMCID: PMC11139828
- DOI: 10.1007/s12055-023-01642-0
Management of cardiopulmonary bypass in patients with ischemic and hemorrhagic strokes in surgery for active infective endocarditis
Abstract
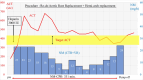
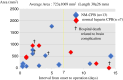
Stroke and intracranial hemorrhage (ICH) are serious complications that are difficult to manage during surgery for active infectious endocarditis (AIE). Relevant society guidelines still recommend delaying the cardiac surgery for AIE with ICH for 4 weeks. Some early studies indicated that the mortality rate decreases when cardiac surgery for ICH is delayed. In contrast, some reported that surgical intervention should not be delayed if an early operation is demanded, even in patients with ICH. The current literature on early vs. late surgery for infectious endocarditis (IE) with ICH is conflicting. Changing the cardiopulmonary bypass (CPB) strategy might be necessary to improve the surgical outcomes of IE with ICH. Some studies reported that cardiac surgery using nafamostat mesylate (NM) as an alternative anticoagulant during CPB was performed successfully. The combination of NM and low-dose heparin was beneficial for early surgery in patients with AIE complicated by cerebral infarction and ICH, without worsening cerebral lesions. In this report, we review and discuss the management of CPB in patients with ischemic and hemorrhagic stroke during surgery for AIE.
Keywords: Cardiopulmonary bypass; Intracranial hemorrhage; Low-dose heparin; Nafamostat mesylate; Neurological complication.
© Indian Association of Cardiovascular-Thoracic Surgeons 2023. Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
Conflict of interest statement
Conflict of interestAll authors declared that there are no conflicts of interest.
Figures


Similar articles
-
Aggressive early surgical strategy in patients with intracranial hemorrhage: a new cardiopulmonary bypass option.Gen Thorac Cardiovasc Surg. 2022 Jul;70(7):602-610. doi: 10.1007/s11748-021-01743-w. Epub 2021 Nov 23. Gen Thorac Cardiovasc Surg. 2022. PMID: 34813003
-
Efficacy of nafamostat mesilate as anticoagulation during cardiopulmonary bypass for early surgery in patients with active infective endocarditis complicated by stroke.J Heart Valve Dis. 2014 Nov;23(6):744-51. J Heart Valve Dis. 2014. PMID: 25790622
-
Is preoperative intracranial hemorrhage a surgical contraindication in infective endocarditis with stroke?J Thorac Dis. 2023 Sep 28;15(9):4765-4774. doi: 10.21037/jtd-23-695. Epub 2023 Aug 30. J Thorac Dis. 2023. PMID: 37868861 Free PMC article.
-
What is the optimal timing for surgery in infective endocarditis with cerebrovascular complications?Interact Cardiovasc Thorac Surg. 2012 Jan;14(1):72-80. doi: 10.1093/icvts/ivr010. Epub 2011 Nov 18. Interact Cardiovasc Thorac Surg. 2012. PMID: 22108925 Free PMC article. Review.
-
Impact of stroke on therapeutic decision making in infective endocarditis.J Neurol. 2010 Mar;257(3):315-21. doi: 10.1007/s00415-009-5364-3. Epub 2009 Oct 30. J Neurol. 2010. PMID: 19876684 Review.
References
-
- Pettersson GB, Coselli JS, Pettersson GB, Coselli JS, Hussain ST, Griffin B, et al. 2016 The American Association for Thoracic Surgery (AATS) consensus guidelines: surgical treatment of infective endocarditis: executive summary. J Thorac Cardiovasc Surg. 2017;153:1241–58.e29. doi: 10.1016/j.jtcvs.2016.09.093. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
