Chronic Postsurgical Pain in Children and Adolescents: A Call for Action
- PMID: 38828088
- PMCID: PMC11144433
- DOI: 10.2147/JPR.S464009
Chronic Postsurgical Pain in Children and Adolescents: A Call for Action
Abstract
Chronic postsurgical pain (CPSP) affects a significant proportion of children and adolescents after major surgery and is a detriment to both short- and long-term recovery outcomes. While clinical characteristics and psychosocial risk factors for developing CPSP in children and adults are well established in the literature, there has been little progress on the prevention and management of CPSP after pediatric surgery. Limited evidence to support current pharmacologic approaches suggests a fundamentally new paradigm must be considered by clinicians to both conceptualize and address this adverse complication. This narrative review provides a comprehensive evaluation of both the known and emerging mechanisms that support our current understanding of CPSP. Additionally, we discuss the importance of optimizing perioperative analgesic strategies to mitigate CPSP based on individual patient risks. We highlight the importance of postoperative pain trajectories to identify those most at risk for developing CPSP, the early referral to multi-disciplinary pain clinics for comprehensive evaluation and treatment of CPSP, and additional work needed to differentiate CPSP characteristics from other chronic pain syndromes in children. Finally, we recognize ongoing challenges associated with the universal implementation of available knowledge about pediatric CPSP into practically useful care plans for clinicians.
Keywords: chronic postsurgical pain; pain management; pediatrics; perioperative care; secondary pain.
© 2024 Einhorn et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures

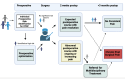
Similar articles
-
Identifying risk factors for chronic postsurgical pain and preventive measures: a comprehensive update.Expert Rev Neurother. 2023 Jul-Dec;23(12):1297-1310. doi: 10.1080/14737175.2023.2284872. Epub 2023 Dec 15. Expert Rev Neurother. 2023. PMID: 37999989 Review.
-
Practical strategies for the prevention and management of chronic postsurgical pain.Korean J Pain. 2023 Apr 1;36(2):149-162. doi: 10.3344/kjp.23080. Korean J Pain. 2023. PMID: 36973967 Free PMC article. Review.
-
Modeling the transition from acute to chronic postsurgical pain in youth: A narrative review of epidemiologic, perioperative, and psychosocial factors.Can J Pain. 2022 Jun 9;6(2):166-174. doi: 10.1080/24740527.2022.2059754. eCollection 2022. Can J Pain. 2022. PMID: 35711297 Free PMC article. Review.
-
Transition from Acute to Chronic Pain: Evaluating Risk for Chronic Postsurgical Pain.Pain Physician. 2019 Sep;22(5):479-488. Pain Physician. 2019. PMID: 31561647 Review.
-
Identification of Presurgical Risk Factors for the Development of Chronic Postsurgical Pain in Adults: A Comprehensive Umbrella Review.J Pain Res. 2024 Jul 30;17:2511-2530. doi: 10.2147/JPR.S466731. eCollection 2024. J Pain Res. 2024. PMID: 39100136 Free PMC article. Review.
Cited by
-
Chronic postsurgical pain after cardiac surgery: A narrative review.Saudi J Anaesth. 2025 Apr-Jun;19(2):181-189. doi: 10.4103/sja.sja_829_24. Epub 2025 Mar 25. Saudi J Anaesth. 2025. PMID: 40255354 Free PMC article. Review.
-
Multi-Institutional Study of Multimodal Analgesia Practice, Pain Trajectories, and Recovery Trends After Spine Fusion for Idiopathic Scoliosis.Anesth Analg. 2025 Jan 2:10.1213/ANE.0000000000007351. doi: 10.1213/ANE.0000000000007351. Online ahead of print. Anesth Analg. 2025. PMID: 39745877
-
Predicting postoperative pain in children: an observational study using the pain threshold Index.Front Pediatr. 2024 Jul 18;12:1398182. doi: 10.3389/fped.2024.1398182. eCollection 2024. Front Pediatr. 2024. PMID: 39091987 Free PMC article.
-
Somatosensory and prefrontal cortex activity relates to emotional outcomes and hair cortisol concentration in chronic postsurgical pain.Sci Rep. 2025 May 10;15(1):16304. doi: 10.1038/s41598-025-00685-0. Sci Rep. 2025. PMID: 40348822 Free PMC article.
References
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

