Ethnic Disparities for Survival and Mortality in New Zealand Patients With Head and Neck Cancer
- PMID: 38833253
- PMCID: PMC11151153
- DOI: 10.1001/jamanetworkopen.2024.13004
Ethnic Disparities for Survival and Mortality in New Zealand Patients With Head and Neck Cancer
Abstract
Importance: It is essential to identify inequitable cancer care for ethnic minority groups, which may allow policy change associated with improved survival and decreased mortality and morbidity.
Objective: To investigate ethnic disparities in survival and mortality among New Zealand (NZ) patients with head and neck cancer (HNC) and the association of other variables, including socioeconomic status, tumor stage, and age at diagnosis, with survival rates.
Design, setting, and participants: This retrospective cohort study was conducted among NZ patients diagnosed with specific HNCs from 2010 to 2020. Anonymized data were obtained from the NZ Cancer Registry, including patients diagnosed from International Statistical Classification of Diseases and Related Health Problems, Tenth Revision (ICD-10) codes C00-C14 and C30-C32. Data were analyzed from July 2020 through January 2024.
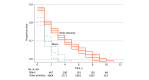
Main outcomes and measures: Censored Kaplan-Meier estimates were used to analyze survival distribution. Cox regression models were used to estimate the association of age, tumor stage at diagnosis, and socioeconomic status with survival rates. Age-standardized mortality rates were assessed.
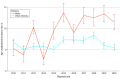
Results: Among 6593 patients with HNCs (4590 males [69.6%]; 4187 patients aged 51-75 years [63.5%]), there were 706 Māori individuals (10.7%) and 5887 individuals with other ethnicity (89.3%), including 4327 NZ European individuals (65.6%; defined as New Zealanders of European descent). Māori individuals had a decreased survival proportion at all years after diagnosis compared with individuals with other ethnicity (eg, 66.1% [95% CI, 62.6%% to 69.8%] vs 71.2% [95% CI, 70.0% to 72.4%] at 2 years). At 1 year after diagnosis, Māori individuals did not have a significantly increased mortality rate compared with 5795 individuals with other ethnicity with data (193 deaths [27.3%] vs 1400 deaths [24.2%]; P = .06), but the rate was significantly increased at 5 years after diagnosis (277 deaths [39.3%] vs 2034 deaths [35.1%]; P = .03); there was greater disparity compared with NZ European individuals (1 year: 969 deaths [22.4%]; P = .003; 5 years: 1441 deaths [33.3%]; P = .002). There were persistent age-adjusted mortality rate disparities: 40.1% (95% CI, -25.9% to 71.2%) for Māori individuals and 18.8% (95% CI, -15.4% to 24.4%) for individuals with other ethnicity. Māori individuals were diagnosed at a mean age of 58.0 years (95% CI, 57.1-59.1 years) vs 64.3 years. (95% CI, 64.0-64.7 years) for individuals with other ethnicity, or 5 to 7 years younger, and died at mean age of 63.5 years (95% CI, 62.0-64.9 years) compared with 72.3 years (95% CI, 71.8-72.9 years) for individuals with other ethnicity, or 7 to 10 years earlier. Māori individuals presented with proportionally more advanced disease (only localized disease, 102 patients [14.5%; 95% CI, 12.0%-17.4%] vs 1413 patients [24.0%; 95% CI, 22.9%-25.1%]; P < .001) and showed an increase in regional lymph nodes (276 patients [39.1%; 95% CI, 35.5%-42.9%] vs 1796 patients [30.5%; 95% CI, 29.3%-31.8%]; P < .001) at diagnosis compared with individuals with other ethnicity. Socioeconomic status was not associated with survival.
Conclusions and relevance: This study found that Māori individuals experienced worse survival outcomes and greater mortality rates from HNC in NZ and presented with more advanced disease at a younger age. These findings suggest the need for further research to alleviate these disparities, highlight the importance of research into minority populations with HNC globally, and may encourage equity research for all cancers.
Conflict of interest statement
Figures
Similar articles
-
Breast cancer biology and ethnic disparities in breast cancer mortality in new zealand: a cohort study.PLoS One. 2015 Apr 7;10(4):e0123523. doi: 10.1371/journal.pone.0123523. eCollection 2015. PLoS One. 2015. PMID: 25849101 Free PMC article.
-
Ethnic disparities in the quality of hospital care in New Zealand, as measured by 30-day rate of unplanned readmission/death.Int J Qual Health Care. 2013 Jul;25(3):248-54. doi: 10.1093/intqhc/mzt012. Epub 2013 Feb 14. Int J Qual Health Care. 2013. PMID: 23411833
-
Differential Outcomes Among Survivors of Head and Neck Cancer Belonging to Racial and Ethnic Minority Groups.JAMA Otolaryngol Head Neck Surg. 2022 Feb 1;148(2):119-127. doi: 10.1001/jamaoto.2021.3425. JAMA Otolaryngol Head Neck Surg. 2022. PMID: 34940784 Free PMC article.
-
Ethnic differences in acute hospitalisations for otitis media and elective hospitalisations for ventilation tubes in New Zealand children aged 0-14 years.N Z Med J. 2015 Jun 12;128(1416):10-20. N Z Med J. 2015. PMID: 26117671
-
Systematic review of disparities in surgical care for Māori in New Zealand.ANZ J Surg. 2018 Jul-Aug;88(7-8):683-689. doi: 10.1111/ans.14310. Epub 2017 Nov 18. ANZ J Surg. 2018. PMID: 29150888
References
-
- Houkamau CA. What you can’t see can hurt you: how do stereotyping, implicit bias and stereotype threat affect Māori health? MAI Journal. 2016;5(2):124-136. doi:10.20507/MAIJournal.2016.5.2.3 - DOI
-
- Gurney JK, Robson B, Koea J, Scott N, Stanley J, Sarfati D. The most commonly diagnosed and most common causes of cancer death for Māori New Zealanders. N Z Med J. 2020;133(1521):77-96. - PubMed
-
- Robson B, Purdie G, Cormack D. Unequal Impact II: Māori and Non-Māori Cancer Statistics by Deprivation and Rural-Urban Status, 2002-2006. New Zealand Ministry of Health; 2010. Accessed April 12, 2024. https://www.health.govt.nz/publication/unequal-impact-ii-maori-and-non-m...
MeSH terms
LinkOut - more resources
Full Text Sources
Medical