Interventions for postburn pruritus
- PMID: 38837237
- PMCID: PMC11152192
- DOI: 10.1002/14651858.CD013468.pub2
Interventions for postburn pruritus
Abstract
Background: Postburn pruritus (itch) is a common and distressing symptom experienced on healing or healed burn or donor site wounds. Topical, systemic, and physical treatments are available to control postburn pruritus; however, it remains unclear how effective these are.
Objectives: To assess the effects of interventions for treating postburn pruritus in any care setting.
Search methods: In September 2022, we searched the Cochrane Wounds Specialised Register, the Cochrane Central Register of Controlled Trials (CENTRAL), Ovid MEDLINE (including In-Process & Other Non-Indexed Citations), Ovid Embase, and EBSCO CINAHL Plus. We also searched clinical trials registries and scanned references of relevant publications to identify eligible trials. There were no restrictions with respect to language, publication date, or study setting.
Selection criteria: Randomised controlled trials (RCTs) that enrolled people with postburn pruritus to compare an intervention for postburn pruritus with any other intervention, placebo or sham intervention, or no intervention.
Data collection and analysis: We used the standard methodological procedures expected by Cochrane. We used GRADE to assess the certainty of the evidence.
Main results: We included 25 RCTs assessing 21 interventions with 1166 randomised participants. These 21 interventions can be grouped into six categories: neuromodulatory agents (such as doxepin, gabapentin, pregabalin, ondansetron), topical therapies (such as CQ-01 hydrogel, silicone gel, enalapril ointment, Provase moisturiser, beeswax and herbal oil cream), physical modalities (such as massage therapy, therapeutic touch, extracorporeal shock wave therapy, enhanced education about silicone gel sheeting), laser scar revision (pulsed dye laser, pulsed high-intensity laser, fractional CO2 laser), electrical stimulation (transcutaneous electrical nerve stimulation, transcranial direct current stimulation), and other therapies (cetirizine/cimetidine combination, lemon balm tea). Most RCTs were conducted at academic hospitals and were at a high risk of performance, attrition, and detection bias. While 24 out of 25 included studies reported change in burn-related pruritus, secondary outcomes such as cost-effectiveness, pain, patient perception, wound healing, and participant health-related quality of life were not reported or were reported incompletely. Neuromodulatory agents versus antihistamines or placebo There is low-certainty evidence that doxepin cream may reduce burn-related pruritus compared with oral antihistamine (mean difference (MD) -2.60 on a 0 to 10 visual analogue scale (VAS), 95% confidence interval (CI) -3.79 to -1.42; 2 studies, 49 participants). A change of 2 points represents a minimal clinically important difference (MCID). Due to very low-certainty evidence, it is uncertain whether doxepin cream impacts the incidence of somnolence as an adverse event compared to oral antihistamine (risk ratio (RR) 0.64, 95% CI 0.32 to 1.25; 1 study, 24 participants). No data were reported on pain in the included study. There is low-certainty evidence that gabapentin may reduce burn-related pruritus compared with cetirizine (MD -2.40 VAS, 95% CI -4.14 to -0.66; 1 study, 40 participants). A change of 2 points represents a MCID. There is low-certainty evidence that gabapentin reduces the incidence of somnolence compared to cetirizine (RR 0.02, 95% CI 0.00 to 0.38; 1 study, 40 participants). No data were reported on pain in the included study. There is low-certainty evidence that pregabalin may result in a reduction in burn-related pruritus intensity compared with cetirizine with pheniramine maleate (MD -0.80 VAS, 95% CI -1.24 to -0.36; 1 study, 40 participants). A change of 2 points represents a MCID. There is low-certainty evidence that pregabalin reduces the incidence of somnolence compared to cetirizine (RR 0.04, 95% CI 0.00 to 0.69; 1 study, 40 participants). No data were reported on pain in the included study. There is moderate-certainty evidence that ondansetron probably results in a reduction in burn-related pruritus intensity compared with diphenhydramine (MD -0.76 on a 0 to 10 numeric analogue scale (NAS), 95% CI -1.50 to -0.02; 1 study, 38 participants). A change of 2 points represents a MCID. No data were reported on pain and adverse events in the included study. Topical therapies versus relevant comparators There is moderate-certainty evidence that enalapril ointment probably decreases mean burn-related pruritus compared with placebo control (MD -0.70 on a 0 to 4 scoring table for itching, 95% CI -1.04 to -0.36; 1 study, 60 participants). No data were reported on pain and adverse events in the included study. Physical modalities versus relevant comparators Compared with standard care, there is low-certainty evidence that massage may reduce burn-related pruritus (standardised mean difference (SMD) -0.86, 95% CI -1.45 to -0.27; 2 studies, 166 participants) and pain (SMD -1.32, 95% CI -1.66 to -0.98). These SMDs equate to a 4.60-point reduction in pruritus and a 3.74-point reduction in pain on a 10-point VAS. A change of 2 VAS points in itch represents a MCID. No data were reported on adverse events in the included studies. There is low-certainty evidence that extracorporeal shock wave therapy (ESWT) may reduce burn-related pruritus compared with sham stimulation (SMD -1.20, 95% CI -1.65 to -0.75; 2 studies, 91 participants). This equates to a 5.93-point reduction in pruritus on a 22-point 12-item Pruritus Severity Scale. There is low-certainty evidence that ESWT may reduce pain compared with sham stimulation (MD 2.96 on a 0 to 25 pressure pain threshold (PPT), 95% CI 1.76 to 4.16; 1 study, 45 participants). No data were reported on adverse events in the included studies. Laser scar revision versus untreated or placebo controls There is moderate-certainty evidence that pulsed high-intensity laser probably results in a reduction in burn-related pruritus intensity compared with placebo laser (MD -0.51 on a 0 to 1 Itch Severity Scale (ISS), 95% CI -0.64 to -0.38; 1 study, 49 participants). There is moderate-certainty evidence that pulsed high-intensity laser probably reduces pain compared with placebo laser (MD -3.23 VAS, 95% CI -5.41 to -1.05; 1 study, 49 participants). No data were reported on adverse events in the included studies.
Authors' conclusions: There is moderate to low-certainty evidence on the effects of 21 interventions. Most studies were small and at a high risk of bias related to blinding and incomplete outcome data. Where there is moderate-certainty evidence, practitioners should consider the applicability of the evidence for their patients.
Trial registration: ClinicalTrials.gov NCT00731367 NCT00859547 NCT01214980 NCT00324311 NCT03777891.
Copyright © 2024 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Conflict of interest statement
Figures
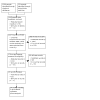
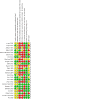
































Update of
References
References to studies included in this review
Ahuja 2011 {published data only}
Ahuja 2013 {published data only}
Allison 2003 {published data only}
Baker 2001 {published data only}
Blome‐Eberwein 2016 {published data only}
-
- Blome-Eberwein S, Gogal C, Weiss MJ, Boorse D, Pagella P. Prospective evaluation of fractional CO2 laser treatment of mature burn scars. Journal of Burn Care & Research 2016;37(6):379-87. - PubMed
Busch 2012 {published data only}
-
- Busch M, Visser A, Eybrechts M, Van Komen R, Oen I, Olff M, et al. The implementation and evaluation of therapeutic touch in burn patients: an instructive experience of conducting a scientific study within a non-academic nursing setting. Patient Education and Counseling 2012;89(3):439-46. [DOI: 10.1016/j.pec.2012.08.012] [PMID: ] - DOI - PubMed
Cho 2014 {published data only}
Demling 2003 {published data only}
-
- Demling RH, DeSanti L. Topical doxepin significantly decreases itching and erythema in the chronically pruritic burn scar. Wounds 2003;15(7):195-200.
Douglas 2019 {published data only}
Ebid 2017 {published data only}
Fayazi 2019 {published data only}
-
- Fayazi N, Rahzani K, Rezaei K, Ali Alizadeh S. The effect of complementary medicine-based intervention on burning patients' pruritus. International Journal of Pharmaceutical and Phytopharmacological Research 2019;9(5):51-6.
Field 2000 {published data only}
Gross 2007 {published data only}
-
- Gross S, Overbaugh R, Jansen R. Ondansetron for treating itch in healing burns. Internet Journal of Pain, Symptom Control and Palliative Care 2007;5(1):5-8.
Hettrick 2004 {published data only}
Joo 2018a {published data only}
Kwa 2019 {published data only}
-
- Kwa KA, Pijpe A, Middelkoop E, Van Baar ME, Niemeijer AS, Breederveld RS, et al. Comparing doxepin cream to oral antihistamines for the treatment of itch in burn patients: a multi-center triple-blind randomized controlled trial. Burns Open 2019;3(4):135-40. [DOI: 10.1016/j.burnso.2019.07.003] - DOI
Kwa 2020 {published data only}
Lewis 2012 {published data only}
-
- Lewis PA, Wright K, Webster A, Steer M, Rudd M, Doubrovsky A, et al. A randomized controlled pilot study comparing aqueous cream with a beeswax and herbal oil cream in the provision of relief from postburn pruritis. Journal of Burn Care & Research 2012;33(4):e195-200. [DOI: 10.1097/BCR.0b013e31825042e2] [PMID: ] - DOI - PubMed
Mohammadi 2018 {published data only}
Nedelec 2012 {published data only}
Samhan 2019 {published data only}
So 2003 {published data only}
-
- So K, Umraw N, Scott J, Campbell K, Musgrave M, Cartotto R. Effects of enhanced patient education on compliance with silicone gel sheeting and burn scar outcome: a randomized prospective study. Journal of Burn Care & Rehabilitation 2003;24(6):411-7. [DOI: 10.1097/01.BCR.0000095516.98523.04] [PMID: ] - DOI - PubMed
Thibaut 2019 {published data only}
Van der Wal 2010 {published data only}
Wu 2016 {published data only}
-
- Wu J, Xu R, Zhan R, Luo G, Niu X, Liu Y, et al. Effective symptomatic treatment for severe and intractable pruritus associated with severe burn-induced hypertrophic scars: a prospective, multicenter, controlled trial. Burns 2016;42(5):1059-66. [DOI: 10.1016/j.burns.2015.09.021] [PMID: ] - DOI - PubMed
References to studies excluded from this review
Abbasi 2020 {published data only}
-
- Abbasi MS, Rahmati J, Ehsani AH, Takzare A, Partoazar A, Takzaree N. Efficacy of a natural topical skin ointment for managing split-thickness skin graft donor sites: a pilot double-blind randomized controlled trial. Advances in Skin & Wound Care 2020;33(7):1-5. [DOI: 10.1097/01.ASW.0000666916.00983.64] [PMID: ] - DOI - PubMed
Abedini 2018 {published data only}
-
- Abedini R, Sasani P, Mahmoudi HR, Nasimi M, Teymourpour A, Shadlou Z. Comparison of intralesional verapamil versus intralesional corticosteroids in treatment of keloids and hypertrophic scars: a randomized controlled trial. Burns 2018;44(6):1482-8. - PubMed
Alizadeh 2020 {published data only}
-
- Alizadeh M, Dahmardehei M, Fahimi S, Sadeghi S. Comparing the effects of a herbal ointment (based on Persian medicine) and silver sulfadiazine ointment on the second-degree burn wounds: a single-blind randomized clinical trial. Research Journal of Pharmacognosy 2020;7(4):11-22. [DOI: 10.22127/RJP.2020.229457.1580] - DOI
Anthonissen 2018 {published data only}
-
- Anthonissen M, Meirte J, Moortgat P, Maertens K, Daly D, Fieuws S, et al. Influence on clinical parameters of depressomassage (part I): the effects of depressomassage on color and transepidermal water loss rate in burn scars: a pilot comparative controlled study. Burns 44;4:877-85. [DOI: 10.1016/j.burns.2017.11.004] [PMID: ] - DOI - PubMed
Asgarirad 2018 {published data only}
Ayaz 2014 {published data only}
Bairagi 2019 {published data only}
-
- Bairagi A, Griffin B, Tyack Z, Vagenas D, McPhail SM, Kimble R. Comparative effectiveness of Biobrane®, RECELL® Autologous skin Cell suspension and Silver dressings in partial thickness paediatric burns: BRACS randomised trial protocol. Burns & Trauma 2019;7(33):1-12. [DOI: 10.1186/s41038-019-0165-0] [PMID: ] - DOI - PMC - PubMed
Barone 1993 {published data only}
Barret 2017 {published data only}
-
- Barret JP, Podmelle F, Lipový B, Rennekampff HO, Schumann H, Schwieger-Briel A, et al. Accelerated re-epithelialization of partial-thickness skin wounds by a topical betulin gel: results of a randomized phase III clinical trials program. Burns 2017;43(6):1284-94. [DOI: 10.1016/j.burns.2017.03.005] [PMID: ] - DOI - PubMed
Belie 2021 {published data only}
Blome‐Eberwein 2010 {published data only}
Blome‐Eberwein 2013 {published data only}
-
- Blome-Eberwein S, Abboud M, Lozano DD, Sharma R, Eid S, Gogal C. Effect of subcutaneous epinephrine/saline/local anesthetic versus saline-only injection on split-thickness skin graft donor site perfusion, healing, and pain. Journal of Burn Care & Research 2013;34(2):e80-6. [DOI: 10.1097/BCR.0b013e31825d5414] [PMID: ] - DOI - PubMed
Blome‐Eberwein 2014 {published data only}
Borland 2005 {published data only}
Campanati 2013 {published data only}
-
- Campanati A, De Blasio S, Giuliano A, Ganzetti G, Giuliodori K, Pecora T, et al. Topical ozonated oil versus hyaluronic gel for the treatment of partial- to full-thickness second-degree burns: a prospective, comparative, single-blind, non-randomised, controlled clinical trial. Burns 2013;39(6):1178-83. [DOI: 10.1016/j.burns.2013.03.002] [PMID: ] - DOI - PubMed
Caruso 2009 {published data only}
-
- Caruso DM, Johnson RM, Blome-Eberwein S, Milner S, Luterman A, Tredget EE, et al. Phase II trial of carboxymethylcellulose silver dressing reinforced with nylon to treat partial thickness burns. Burns 2009;35 Suppl 1:S32. [DOI: 10.1016/j.burns.2009.06.128] [PMID: ] - DOI
Chi 2015 {published data only}
Cho 2012 {published data only}
Cuignet 2004 {published data only}
-
- Cuignet O, Pirson J, Boughrouph J, Duville D. The efficacy of continuous fascia iliaca compartment block for pain management in burn patients undergoing skin grafting procedures. Anesthesia & Analgesia 2004;98(4):1077-81. [DOI: 10.1213/01.ane.0000105863.04140.ae] [PMID: ] - DOI - PubMed
Cuignet 2015 {published data only}
Demling 2001 {published data only}
-
- Demling R, DeSanti L. Topical doxepin significantly decreases itching and erythema in the healed burn wound. Wounds 2001;14(9):334-9.
De Oliveira 2018 {published data only}
-
- De Oliveira RA, Boson LL, Portela SM, Maia Filho AL, De Oliveira Santiago D. Low-intensity LED therapy (658 nm) on burn healing: a series of cases. Lasers in Medical Science 2018;33(4):729-35. [PMID: ] - PubMed
Foster 2011 {published data only}
Gaida 2004 {published data only}
Gardien 2014 {published data only}
-
- Gardien KL, Olde Damink LH, Heschel I, Vloemans AF, Tempelman FR, Van Zuijlen PP, et al, Euroskingraft Study Group. A novel dermal substitute in combination with a split-thickness skin autograft for burn wound treatment: preliminary results of a safety trial. Wound Repair and Regeneration 2014;22(5):A80. [DOI: 10.1111/wrr.12242] [PMID: ] - DOI - PubMed
Girard 1998 {published data only}
-
- Girard P, Beraud A, Goujon C, Sirvent A, Foyatier J‐L, Alleaume B, et al. Effect of Bepanthen(TM) ointment on the graft-donor site wound-healing model: double-blind biometrological and clinical study, with assessment by the patient, versus the vehicle. Nouvelles Dermatologiques 1998;17(9):559‐70. [EMBASE 28566458]
Goutos 2010 {published data only}
-
- Goutos I, Eldardiri M, Khan AA, Dziewulski P, Richardson PM. Comparative evaluation of antipruritic protocols in acute burns. The emerging value of gabapentin in the treatment of burns pruritus. Journal of Burn Care & Research 2010;31(1):57-63. [PMID: ] - PubMed
Gray 2011 {published data only}
-
- Gray P, Kirby J, Williams B, Cramond T, Doecke J, Cabot P, et al. Pregabalin reduces neuropathic-like pain after burn injury - a randomized, double-blind, placebo-controlled trial. Pain Medicine 2009;10(6):1151-8. [DOI: 10.1111/j.1526-4637.2009.00693.x] - DOI
Greenhalgh 1994 {published data only}
Guo 2010 {published data only}
-
- Guo X, Tan M, Guo L, Xiong A, Li Y, He X. Clinical study on repair of burn wounds of degree II with recombinant human epidermal growth factor in elderly patients. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi [Chinese Journal of Reparative and Reconstructive Surgery] 2010;24(4):462-4. [PMID: ] - PubMed
Hernández 2011 {published data only}
-
- Hernández R, Garibay M. Silver sulfadiazine cream versus topical application in second degree burns [Sulfadiazina de plata en crema versus suspensión tópica en quemaduras de segundo grado]. Revista Mexicana de Pediatría 2011;78(2):56-9.
Heydarikhayat 2018 {published data only}
Hindy 2009 {published data only}
Hultman 2013b {published data only}
-
- Hultman CS, Friedstat JS, Edkins RE, Saou MA, Roach ST, Cairns BA. There is a light that never goes out: impact of timing after injury on efficacy of laser treatment of burn scars, using a prospective, before-after cohort model. Journal of Burn Care & Research 2013;34(Suppl 1):S64-197. [DOI: 10.1097/BCR.0b013e31828d5efd] [PMID: ] - DOI - PubMed
Hultman 2014 {published data only}
-
- Hultman CS, Friedstat JS, Edkins RE, Cairns BA, Meyer AA. Laser resurfacing and remodeling of hypertrophic burn scars: the results of a large, prospective, before-after cohort study, with long-term follow-up. Annals of Surgery 2014;260(3):519-29. [DOI: 10.1097/SLA.0000000000000893] [PMID: ] - DOI - PubMed
Ioannovich 2003 {published data only}
-
- Ioannovich JD, Magliacani G, Costagliola M, Attiyeh B, Dahm R, Berger A, et al. Moist exposed therapy of partial-thickness burn wounds. A multi-center study. European Journal of Plastic Surgery 2003;26(7):338-45. [DOI: ]
Issler‐Fisher 2020 {published data only}
Johansen 1970 {published data only}
Joo 2017 {published data only}
Joo 2018b {published data only}
-
- Joo SY, Kim JB, Cho YS, Cho YS, Seo CH. Effect of cold pack therapy for management of burn scar pruritus: a pilot study. Burns 2018;44(4):1005-10. [PMID: ] - PubMed
Jung 2009 {published data only}
Kemp‐Offenberg 2015 {published data only}
Ki 2019 {published data only}
Kisch 2021 {published data only}
Kono 2005 {published data only}
LaSalle 2008 {published data only}
Lee 2021 {published data only}
Li 2015 {published data only}
-
- Li S, Min S, Wu B, Tang W. Application of patient-controlled intravenous analgesia of dezocine combined with sufentanil in burn patients after surgery. Zhonghua Shao Shang Za Zhi [Chinese Journal of Burns] 2015;31(1):48-51. [PMID: ] - PubMed
Li 2018 {published data only}
Li‐Tsang 2006 {published data only}
-
- Li-Tsang CW, Lau JC, Choi J, Chan CC, Jianan L. A prospective randomized clinical trial to investigate the effect of silicone gel sheeting (Cica-Care) on post-traumatic hypertrophic scar among the Chinese population. Burns 2006;32(6):678-83. - PubMed
Lv 2019 {published data only}
-
- Lv K, Liu H, Xiao S, Xia Z. 318 Efficacy of whole scar ablative fractional carbon dioxide laser treatment in patients with large area of burn scar: a prospective cohort study. Journal of Burn Care & Research 2019;40:S136-7. [DOI: 10.1093/jbcr/irz013.231] - DOI
Lv 2021 {published data only}
Marck 2016 {published data only}
-
- Marck RE, Gardien KL, Stekelenburg CM, Vehmeijer M, Baas D, Tuinebreijer WE, et al. The application of platelet‐rich plasma in the treatment of deep dermal burns: a randomized, double‐blind, intra‐patient controlled study. Wound Repair and Regeneration 2016;24(4):712-20. [DOI: 10.1111/wrr.12443] [PMID: ] - DOI - PubMed
Matheson 2001 {published data only}
Matuszczak 2020 {published data only}
-
- Matuszczak E, Weremijewicz A, Koper-Lenkiewicz OM, Kamińska J, Hermanowicz A, Dębek W, et al. Effects of combined pulsed dye laser and fractional CO2 laser treatment of burn scars and correlation with plasma levels of collagen type I, MMP-2 and TIMP-1. Burns 2021;47(6):1342-51. [DOI: 10.1016/j.burns.2020.12.011] [PMID: ] - DOI - PubMed
McBride 2018 {published data only}
Memon 2005 {published data only}
-
- Memon AR, Tahir SM, Khushk IA, Memon GA. Therapeutic effects of honey versus silver sulphadiazine in the management of burn injuries. Journal of Liaquat University of Medical & Health Sciences 2005;4:100-4.
Mileski 2003 {published data only}
-
- Mileski WJ, Burkhart D, Hunt JL, Kagan RJ, Saffle JR, Herndon DN, et al. Clinical effects of inhibiting leukocyte adhesion with monoclonal antibody to intercellular adhesion molecule-1 (enlimomab) in the treatment of partial-thickness burn injury. Journal of Trauma and Acute Care Surgery 2003;54(5):950-8. [DOI: 10.1097/01.TA.0000030626.84680.11] [PMID: ] - DOI - PubMed
Miletta 2019 {published data only}
-
- Miletta N, Siwy K, Hivnor C, Clark J, Shofner J, Zurakowski D, et al. Fractional ablative laser therapy is an effective treatment for hypertrophic burn scars: a prospective study of objective and subjective outcomes. Annals of Surgery 2019;274(6):e574-80. [DOI: 10.1097/SLA.0000000000003576] [PMID: ] - DOI - PubMed
Mohammadi 2017 {published data only}
Moons 2011 {published data only}
-
- Moons P, Casaer M, Haest C, Morren M-A. Profile of itch experience in patients with atopic dermatitis, chronic urticaria and burns: direct comparison using the Leuven itch scale. Acta Dermato-Venereologica 2011;91(5):631-2.
Moortgat 2015 {published data only}
-
- Moortgat P, Van Daele U, Anthonissen M, Meirte J, Lafaire C, De Cuyper L, et al. Tension reducing taping as a mechanotherapy for hypertrophic burn scars-a proof of concept (170). Annals of Burns and Fire Disasters 2015;28:300.
Mumtaz 2008 {published data only}
-
- Mumtaz F, Memon AR, Tahir SM, Shaikh BF. The therapeutic efficacy of pharmacological versus non-pharmacological measures in the management of post burn itch. Pakistan Armed Forces Medical Journal 2008;58(3):312-8.
Namviriyachote 2012 {published data only}
-
- Namviriyachote N, Aramwit P, Muangman P. PSS3 the efficacy of epidermal growth factor in burn wound treatment. Value in Health 2012;15(7):A568. [DOI: 10.1016/j.jval.2012.08.2050] - DOI
Nasiri 2016 {published data only}
Nedelec 2019 {published data only}
Nedelec 2020 {published data only}
-
- Nedelec B, LaSalle L, De Oliveira A, Correa JA. Within-patient, single-blinded, randomized controlled clinical trial to evaluate the efficacy of triamcinolone acetonide injections for the treatment of hypertrophic scar in adult burn survivors. Journal of Burn Care & Research 2020;41(4):761-9. [DOI: 10.1093/jbcr/iraa057] [PMID: ] - DOI - PubMed
Ogawa 2008 {published data only}
-
- Ogawa R, Hyakusoku H, Ogawa K, Nakao C. Effectiveness of mugwort lotion for the treatment of post-burn hypertrophic scars. Journal of Plastic, Reconstructive & Aesthetic Surgery 2008;61(2):210-2. [PMID: ] - PubMed
Parlak 2010 {published data only}
-
- Parlak Gürol A, Polat S, Nuran Akçay M. Itching, pain, and anxiety levels are reduced with massage therapy in burned adolescents. Journal of Burn Care & Research 2010;31(3):429-32. - PubMed
Patiño 1999 {published data only}
-
- Patiño O, Novick C, Merlo A, Benaim F. Massage in hypertrophic scars. Journal of Burn Care & Rehabilitation 1999;20(3):268-71. [PMID: ] - PubMed
Prather 2015 {published data only}
-
- Prather J, Tummel E, Nichols J, Patel A, Gould LJ. A prospective, randomized, controlled pilot study of noncontact low-frequency ultrasound (NLFU) to accelerate healing of split thickness donor sites. Journal of the American College of Surgeons 2014;219(3):S89. [DOI: 10.1016/j.jamcollsurg.2014.07.211] - DOI - PubMed
-
- Prather JL, Tummel EK, Patel AB, Smith DJ, Gould LJ. Prospective randomized controlled trial comparing the effects of noncontact low-frequency ultrasound with standard care in healing split-thickness donor sites. Journal of the American College of Surgeons 2015;221(2):309-18. [DOI: 10.1016/j.jamcollsurg.2015.02.031] [PMID: ] - DOI - PubMed
Rashaan 2019 {published data only}
-
- Rashaan ZM, Krijnen P, Kwa KA, Van der Vlies CH, Schipper IB, Breederveld RS. Flaminal® versus Flamazine® in the treatment of partial thickness burns: a randomized controlled trial on clinical effectiveness and scar quality (FLAM study). Wound Repair and Regeneration 2019;27(3):257-67. [DOI: 10.1111/wrr.12699] [PMC6850327] [PMID: ] - DOI - PMC - PubMed
Ren 2021 {published data only}
Robert 2008 {published data only}
-
- Robert R, Tcheung WJ, Rosenberg L, Rosenberg M, Mitchell C, Villarreal C, et al. Treating thermally injured children suffering symptoms of acute stress with imipramine and fluoxetine: a randomized, double-blind study. Burns 2008;34(7):919-28. [DOI: 10.1016/j.burns.2008.04.009] [PMID: ] - DOI - PubMed
Roh 2007 {published data only}
Rosenberg 2014 {published data only}
Saeidinia 2017 {published data only}
-
- Saeidinia A, Keihanian F, Lashkari AP, Lahiji HG, Mobayyen M, Heidarzade A, et al. Partial-thickness burn wounds healing by topical treatment: a randomized controlled comparison between silver sulfadiazine and centiderm. Medicine 2017;96(9):e6168. [DOI: 10.1097/MD.0000000000006168] - DOI - PMC - PubMed
Saravanan 2017 {published data only}
-
- Saravanan P, Chenthamarai G. A randomized, open-label, comparative study of lysine cream with standard treatment in patients with second-degree superficial burns. Asian Journal of Pharmaceutical and Clinical Research 2017;10(5):219-21. [DOI: 10.22159/ajpcr.2017.v10i5.16431] - DOI
Sheridan 1997 {published data only}
-
- Sheridan RL, MacMillan K, Donelan M, Choucair R, Grevelink J, Petras L, et al. Tunable dye laser neovessel ablation as an adjunct to the management of hypertrophic scarring in burned children: pilot trial to establish safety. Journal of Burn Care & Rehabilitation 1997;18(4):317-20. [DOI: 10.1097/00004630-199707000-00007] [PMID: ] - DOI - PubMed
Srivastava 2019 {published data only}
Taheri 2018 {published data only}
-
- Taheri P, Khosrawi S, Mazaheri M, Parsa MA, Mokhtarian A. Effect of extracorporeal shock wave therapy on improving burn scar in patients with burnt extremities in Isfahan, Iran. Journal of Research in Medical Sciences 2018;23:81. [DOI: 10.4103/jrms.JRMS_681_17] [PMC6161486] [PMID: ] - DOI - PMC - PubMed
Tang 2015 {published data only}
-
- Tang D, Li-Tsang CW, Au RK, Li KC, Yi XF, Liao LR, et al. Functional outcomes of burn patients with or without rehabilitation in mainland China. Hong Kong Journal of Occupational Therapy 2015;26(1):15-23. [DOI: 10.1016/j.hkjot.2015.08.003] - DOI
Tawfic 2019 {published data only}
Verbelen 2014 {published data only}
Vitale 1991 {published data only}
-
- Vitale M, Fields-Blache C, Luterman A. Severe itching in the patient with burns. Journal of Burn Care & Research 1991;12(4):330-3. [PMID: ] - PubMed
Vloemans 2003 {published data only}
Voinchet 2006 {published data only}
Wahba 2019 {published data only}
-
- Wahba E, Hamada H, Khatib A. Effect of silicone gel versus Contractubex or corticosteroid phonophoresis for post-burn hypertrophic scars: a single-blind randomized controlled trial. Physiotherapy Quarterly 2019;28(1):1-5. [DOI: 10.5114/pq.2019.83054] - DOI
Wang 2017 {published data only}
Wasiak 2011 {published data only}
-
- Wasiak J, Spinks A, Costello V, Ferraro F, Paul E, Konstantatos A, et al. Adjuvant use of intravenous lidocaine for procedural burn pain relief: a randomized double-blind, placebo-controlled, cross-over trial. Burns 2011;37(6):951-7. [PMID: ] - PubMed
Welling 2007 {published data only}
Wiseman 2020 {published data only}
-
- Wiseman J, Ware RS, Simons M, McPhail S, Kimble R, Dotta A, et al. Effectiveness of topical silicone gel and pressure garment therapy for burn scar prevention and management in children: a randomized controlled trial. Clinical Rehabilitation 2020;34(1):120-31. [DOI: 10.1177/0269215519877516] [PMID: ] - DOI - PMC - PubMed
Wittenberg 1999 {published data only}
-
- Wittenberg GP, Fabian BG, Bogomilsky JL, Schultz LR, Rudner EJ, Chaffins ML, et al. Prospective, single-blind, randomized, controlled study to assess the efficacy of the 585-nm flashlamp-pumped pulsed-dye laser and silicone gel sheeting in hypertrophic scar treatment. Archives of Dermatology 1999;135(9):1049-55. [DOI: 10.1001/archderm.135.9.1049] [PMID: ] - DOI - PubMed
Xian‐zhong 2010 {published data only}
-
- Xian-zhong Z, Kee-yan S, Yong-liang G, Dong-bo Z, Dong-jing Y. Skin regeneration following scar removal and in situ replantation for treating hypertrophic scar. Journal of Clinical Rehabilitative Tissue Engineering Research 2010;14(18):3327-30. [DOI: 10.3969/j.issn.1673-8225.2010.18.023] - DOI
Xie 2018 {published data only}
Yaron 2018 {published data only}
-
- Yaron HS. Intralesional cryosurgery for the treatment of hypertrophic scars and keloids: an evidence-based novel technology. Journal of the American Academy of Dermatology 2018;79(3):AB170. [DOI: 10.1016/j.jaad.2018.05.693] - DOI
Zheng 2016 {published data only}
-
- Zheng X, Chen T, Zhang L, Cheng R, Chang F, Ji S, et al. Clinical therapeutic effect of sheet split-thickness skin graft with micropores in repairing third-degree burn wounds on the hands. Medical Science and Technology 2016;57:74-80. [DOI: 10.12659/MST.900085] - DOI
References to studies awaiting assessment
Harada 1995 {published data only}
-
- Harada S, Ohara K, Takemura T, Niimura M, Nishikawa T, Kukita A. Clinical evaluation of M-1011G (lysozyme hydrochloride ointment-gauze) in patients with burn: a multi-centered double-blind comparative study with placebo. Rinsho Iyaku [Journal of Clinical Therapeutics and Medicine] 1995;11(2):415‐29.
Huang 2021a {published data only}
Huang 2021b {published data only}
-
- Huang Z, Chen Y, Wang P, Zheng DW, Zong YL, Lyu GZ. A prospective randomized controlled clinical study on the treatment of hypertrophic scar after burn by fractional carbon dioxide laser combined with autologous fat injection. Zhonghua Shao Shang Za Zhi [Chinese Journal of Burns] 2021;37(1):49-56. [DOI: 10.3760/cma.j.cn501120-20200104-00002] [PMID: ] - DOI - PubMed
Lee 2017 {published data only}
-
- Lee SY, Joo SY, Cho YS, Seo CH. Effects of extracorporeal shock wave therapy for the management of burn pruritus. Journal of Wound Care 2017;26(Suppl 6b):269. [DOI: 10.12968/jowc.2017.26.Sup6b.1] - DOI
Ohrtman 2019 {published data only}
-
- Ohrtman E, Thibaut A, Morales-Quezada L, Simko L, Zafonte R, Ryan C, et al. 416 Effects of transcranial direct current stimulation on pain and itch after burn injury. Journal of Burn Care & Research 2019;40(Suppl 1):S180-1. [DOI: 10.1093/jbcr/irz013.314] - DOI
Still 2000 {published data only}
-
- Still J, Hickerson W, Lett D, Klein M, Bishop J. A study to measure and compare the efficacy of integrity technologies hydration formulas (physics plus process) to Elta, a conventional moisturizing lotion for the burn and scarred patient in the relief of pruritis. In: 10th Conference of the European Wound Management Association. Stockholm, Sweden, 2000.
Waked 2013 {published data only}
-
- Waked IS, Nagib SH, Ashm HN. Triamcinolone acetonide phonophoresis versus transcutanous electrical nerve stimulation in the treatment of post-burn pruritus-a randomised controlled study. Indian Journal of Physiotherapy & Occupational Therapy 2013;7(2):87-92.
Zhang 2018 {published data only}
-
- Zhang YQ, Dong JY, Wang C, Yan M, Yao M. Clinical effects of a combination treatment with narrow-spectrum intense pulsed light and fractional carbon dioxide laser on hypertrophic scar pruritus. Zhonghua Shao Shang Za Zhi [Chinese Journal of Burns] 2018;34(9):608-14. [DOI: 10.3760/cma.j.issn.1009-2587.2018.09.010] [PMID: ] - DOI - PubMed
Zheng 2015 {published data only}
-
- Zheng L, Bing Z, Wei L, Qiang W. Clinical effects of gabapentin on the treatment of pruritus of scar resulting from deep partial-thickness burn. Zhonghua Shao Shang Za Zhi [Chinese Journal of Burns] 2015;31(3):177-80. [PMID: ] - PubMed
References to ongoing studies
IRCT20170609034406N7 {published data only}
-
- Evaluation of anti-pruritic effects of curcumin in treatment resistant burn patients. www.irct.ir/trial/54335.
IRCT20180609040016N2 {published data only}
-
- Evaluation the effect of Fumaria Parviflora L. on post burn pruritus: a randomized double-blind clinical trial. en.irct.ir/trial/49636.
IRCT20210306050596N1 {published data only}
-
- The effect of aloe vera on post burns pruritus. www.irct.ir/trial/54852.
ISRCTN10393098 {published data only}ISRCTN10393098
-
- ISRCTN10393098. Comparing the effectiveness of post-burn itchy skin treatment with cetirizine or gabapentin. https://www.isrctn.com/ISRCTN10393098.
Additional references
Ahuja 2011
Ahuja 2013
Ahuja 2014
-
- Ahuja RB, Chatterjee P. Postburn pruritus: a practical review. Indian Journal of Burns 2014;22(1):13.
Ahuja 2016
Andrade 2023
Andrew 2001
-
- Andrew D, Craig AD. Spinothalamic lamina I neurons selectively sensitive to histamine: a central neural pathway for itch. Nature Neuroscience 2001;4(1):72. - PubMed
Aziz 2012
Badwy 2022
Baker 2001
-
- Baker RA, Zeller RA, Klein RL, Thornton RJ, Shuber JH, Marshall RE, et al. Burn wound itch control using H1 and H2 antagonists. Journal of Burn Care & Rehabilitation 2001;22(4):263-8. [PMID: ] - PubMed
Ballantyne 1988
-
- Ballantyne JC, Loach AB, Carr DB. Itching after epidural and spinal opiates. Pain 1988;33(2):149-60. [PMID: ] - PubMed
Bell 1988
-
- Bell L, McAdams T, Morgan R, Parshley PF, Pike RC, Riggs P, et al. Pruritus in burns: a descriptive study. Journal of Burn Care & Rehabilitation 1988;9(3):305-8. [PMID: ] - PubMed
Bell 2009
Bennett 2004
Biró 2005
-
- Biró T, Ko MC, Bromm B, Wei ET, Bigliardi P, Siebenhaar F, et al. How best to fight that nasty itch – from new insights into the neuroimmunological, neuroendocrine, and neurophysiological bases of pruritus to novel therapeutic approaches. Experimental Dermatology 2005;14(3):225-40. [DOI: 10.1111/j.0906-6705.2005.0321a.x] [PMID: ] - DOI - PubMed
Bockbrader 2010
Bowsher 1991
Bromma 1995
-
- Bromma B, Scharein E, Darsow U, Ring J. Effects of menthol and cold on histamine-induced itch and skin reactions in man. Neuroscience Letters 1995;187(3):157-60. [PMID: ] - PubMed
Brooks 2007
Carrougher 2013
-
- Carrougher GJ, Martinez EM, McMullen KS, Fauerbach JA, Holavanahalli RK, Herndon DN, et al. Pruritus in adult burn survivors: postburn prevalence and risk factors associated with increased intensity. Journal of Burn Care & Research 2013;34(1):94-101. [DOI: 10.1097/BCR.0b013e3182644c25] [PMID: ] - DOI - PubMed
Chaussy 1980
-
- Chaussy C, Brendel W, Schmiedt E. Extracorporeally induced destruction of kidney stones by shock waves. Lancet 1980;2(8207):1265-8. [PMID: ] - PubMed
Choi 2013
Chung 2020
Dallos 2006
-
- Dallos A, Kiss M, Polyánka H, Dobozy A, Kemény L, Husz S. Effects of the neuropeptides substance P, calcitonin gene-related peptide, vasoactive intestinal polypeptide and galanin on the production of nerve growth factor and inflammatory cytokines in cultured human keratinocytes. Neuropeptides 2006;40(4):251-63. [DOI: 10.1016/j.npep.2006.06.002] [PMID: ] - DOI - PubMed
Deeks 2020
-
- Deeks JJ, Higgins JP, Altman DG, editor(s). Chapter 10: Analysing data and undertaking meta-analyses. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.1 (updated September 2020). Cochrane, 2020. Available from training.cochrane.org/handbook.
Demling 2001
-
- Demling RH, DeSanti L. Topical doxepin cream is effective in relieving severe pruritus caused by burn injury: a preliminary study. Wounds 2001;13(6):210-5.
Demling 2003
-
- Demling RH, DeSanti L. Topical doxepin significantly decreases itching and erythema in the chronically pruritic burn scar. Wounds: a compendium of clinical research and practice 2003;15(6):195-200.
Dunn 2004
-
- Dunn K, Edwards-Jones V. The role of Acticoat™ with nanocrystalline silver in the management of burns. Burns 2004;30(Suppl 1):S1-9. [PMID: ] - PubMed
Egger 1997
Elman 2010
Engin 2009
Esselman 2006
Esselman 2007
Farzam 2023
-
- Farzam K, Sabir S, O'Rourke MC. Antihistamines. In: StatPearls. StatPearls Publishing, 2023. [BOOKSHELF ID: NBK538188] - PubMed
Field 2000
-
- Field T, Peck M, Hernandez-Reif M, Krugman S, Burman I, Ozment-Schenck L. Postburn itching, pain, and psychological symptoms are reduced with massage therapy. Journal of Burn Care & Rehabilitation 2000;21(3):189-93. [PMID: ] - PubMed
Fischer 1982
-
- Fischer HB, Scott PV. Spinal opiate analgesia and facial pruritus. Anaesthesia 1982;37(7):777-8. - PubMed
Galeotti 2002
-
- Galeotti N, Mannelli LD, Mazzanti G, Bartolini A, Ghelardini C. Menthol: a natural analgesic compound. Neuroscience Letters 2002;322(3):145-8. [PMID: ] - PubMed
Geronemus 2006
Glanville 2019
-
- Glanville J, Dooley G, Wisniewski S, Foxlee R, Noel-Storr A. Development of a search filter to identify reports of controlled clinical trials within CINAHL Plus. Health Information & Libraries Journal 2019;36(1):73-90. - PubMed
Goutos 2009
Goutos 2010
-
- Goutos I, Clarke M, Upson C, Richardson PM, Ghosh SJ. Review of therapeutic agents for burns pruritus and protocols for management in adult and paediatric patients using the GRADE classification. Indian Journal of Plastic Surgery 2010;43(Suppl):S51–62. [DOI: 10.4103/0970-0358.70721] [PMID: ] - DOI - PMC - PubMed
Goutos 2013
GRADE 2013
-
- Schünemann H, Brożek J, Guyatt G, Oxman A, editor(s). Handbook for grading the quality of evidence and the strength of recommendations using the GRADE approach (updated October 2013). GRADE Working Group, 2013. Available from gdt.guidelinedevelopment.org/app/handbook/handbook.html. [DOI: ]
Gross 2007
-
- Gross S, Overbaugh R, Jansen R. Ondansetron for treating itch in healing burns. Internet Journal of Pain, Symptom Control and Palliative Care 2007;5:4.
Hahn 2005
Hettrick 2004
-
- Hettrick HH, O'Brien K, Laznick H, Sanchez J, Gorga D, Nagler W, et al. Effect of transcutaneous electrical nerve stimulation for the management of burn pruritus: a pilot study. Journal of Burn Care & Rehabilitation 2004;25(3):236-40. [10.1097/01.bcr.0000124745.22170.86] [PMID: ] - PubMed
Higgins 2003
Higgins 2017
-
- Higgins JP, Altman DG, Sterne JA (editors). Chapter 8: Assessing risk of bias in included studies. Higgins JP, Churchill R, Chandler J, Cumpston MS (editors), Cochrane Handbook for Systematic Reviews of Interventions Version 5.2.0 (updated June 2017). The Cochrane Collaboration, 2017. Available from training.cochrane.org/handbook/archive/v5.1/. [AVAILABLE FROM: www.training.cochrane.org/handbook2017]
Higgins 2022
-
- Higgins JP, Eldridge S, Li T, editor(s). Chapter 23: Including variants on randomized trials. In: Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA, editor(s). Cochrane Handbook for Systematic Reviews of Interventions Version 6.3 (updated February 2022). Cochrane, 2022. Available from training.cochrane.org/handbook.
Hróbjartsson 2012
Inagaki 2000
Jeffry 2011
Joo 2017
Kamei 2001
-
- Kamei J, Nagase H. Norbinaltorphimine, a selective kappaopioid receptor antagonist, induces an itch-associated response in mice. European Journal of Pharmacology 2001;418(1-2):141–5. [PMID: ] - PubMed
Kaul 2018
Kim 2013
Kwa 2021
-
- Kwa KAA. Scratching Beneath the Surface: Innovative Treatment Modalities for Burn Patients. Leiden University, 2021. [HANDLE.NET REGISTRY: https://hdl.handle.net/1887/3216971] [ISBN: 9789464167924]
LaSalle 2008
Lefebvre 2022
-
- Lefebvre C, Glanville J, Briscoe S, Featherstone R, Littlewood A, Marshall C, et al. Chapter 4: Searching for and selecting studies. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). Cochrane, 2022. Available from training.cochrane.org/handbook. [AVAILABLE FROM: www.training.cochrane.org/handbook]
Lesaffre 2009
Levi 2016
Liberati 2009
-
- Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLOS Medicine 2009;6(7):e1000100. [DOI: 10.1016/j.jclinepi.2009.06.006] [PMID: ] - DOI - PMC - PubMed
Manstein 2004
Melzack 1965
-
- Melzack R, Wall PD. Pain mechanisms: a new theory. Science 1965;150(3699):971-9. [PMID: ] - PubMed
Mendham 2004
Mohammad Ali 2015
Murphy 2005
-
- Murphy KD, Lee JO, Herndon DN. Current pharmacotherapy for the treatment of severe burns. Expert Opinion on Pharmacotherapy 2003;4(3):369-84. - PubMed
Nedelec 2018
-
- Nedelec B, LaSalle L. Postburn itch: a review of the literature. Wounds: a compendium of clinical research and practice 2018;30(1):E118-24. - PubMed
Nedoszytko 2014
-
- Nedoszytko B, Sokołowska-Wojdyło M, Ruckemann-Dziurdzińska K, Roszkiewicz J, Nowicki R. Chemokines and cytokines network in the pathogenesis of the inflammatory skin diseases: atopic dermatitis, psoriasis and skin mastocytosis. Advances in Dermatology and Allergology 2014;31(2):84-91. [DOI: 10.5114/pdia.2014.40920] - DOI - PMC - PubMed
NHS Inform 2018
-
- NHS Inform. Burns and scalds. Types of burn. Updated 1 May 2018. www.nhsinform.scot/illnesses-and-conditions/injuries/skin-injuries/burns-and-scalds (accessed 31 October 2018).
Nilsson 2004
-
- Nilsson HJ, Psouni E, Carstam R, Schouenborg J. Profound inhibition of chronic itch induced by stimulation of thin cutaneous nerve fibres. Journal of the European Academy of Dermatology and Venereology 2004;18(1):37-43. [PMID: ] - PubMed
O'Donoghue 2005
Opriessnig 2023
Parmar 1998
-
- Parmar MK, Torri V, Stewart L. Extracting summary statistics to perform meta-analyses of the published literature for survival endpoints. Statistics in Medicine 1998;17(24):2815-34. [PMID: ] - PubMed
Patel 2007
Paul 2015
-
- Paul JC. Wound pruritus: pathophysiology and management. Chronic Wound Care Management and Research 2015;2:119–27.
Procter 2010
Qu 2012
Reich 2006
-
- Reich A, Riepe C, Anastasiadou Z, Mędrek K, Augustin M, Szepietowski JC, et al. Itch assessment with visual analogue scale and numerical rating scale: determination of minimal clinically important difference in chronic itch. Acta Dermato-venereologica 2016;96(7):978-80. [DOI: 10.2340/00015555-2433] [PMID: ] - DOI - PubMed
Review Manager 2014 [Computer program]
-
- Review Manager 5 (RevMan 5). Version 5.3. Copenhagen: Nordic Cochrane Centre, The Cochrane Collaboration, 2014.
Roh 2007
-
- Roh YS, Cho H, Oh JO, Yoon CJ. Effects of skin rehabilitation massage therapy on pruritus, skin status, and depression in burn survivors. Journal of Korean Academy of Nursing 2007;37(2):221-6. [PMID: ] - PubMed
Rybarczyk 2017
-
- Rybarczyk MM, Schafer JM, Elm CM, Sarvepalli S, Vaswani PA, Balhara KS, et al. A systematic review of burn injuries in low- and middle-income countries: epidemiology in the WHO-defined African Region. African Journal of Emergency Medicine 2017;7(1):30-7. [DOI: 10.1016/j.burns.2018.01.015] - DOI - PMC - PubMed
Santuzzi 2023
Schmelz 2001
Schünemann 2022a
-
- Schünemann HJ, Higgins JPT, Vist GE, Glasziou P, Akl EA, Skoetz N, et al. Chapter 14: Completing ‘Summary of findings’ tables and grading the certainty of the evidence. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). Cochrane, 2022. Available from training.cochrane.org/handbook.
Schünemann 2022b
-
- Schünemann HJ, Vist GE, Higgins JPT, Santesso N, Deeks JJ, Glasziou P, Akl EA, Guyatt GH. Chapter 15: Interpreting results and drawing conclusions. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). Cochrane, 2022. Available from training.cochrane.org/handbook.
Sinha 2017
Sinha 2018a
-
- Sinha S, Biernaskie JA, Nickerson D, Gabriel VA. Nitrogen-containing bisphosphonates for burn-related heterotopic ossification. Burns Open 2018;2(3):160-3. [DOI: 10.1016/j.burnso.2017.12.004] - DOI
Sinha 2018b
Smolle 2017
Steinhoff 2009
-
- Steinhoff A, Steinhoff M. Neuroimmunology of atopic dermatitis. In: Granstein RD, Luger TA, editors(s). Neuroimmunology of the Skin. Springer Berlin, Heidelberg, 2009:197–207. [DOI: 10.1007/978-3-540-35989-0_18] - DOI
Sterne 2022
-
- Sterne JAC, Hernán MA, McAleenan A, Reeves BC, Higgins JPT. Chapter 25: Assessing risk of bias in a non-randomized study. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). Cochrane, 2022. Available from training.cochrane.org/handbook.
Tierney 2007
Tu 2017
Twycross 2003
-
- Twycross R, Greaves MW, Handwerker H, Jones EA, Libretto SE, Szepietowski JC, et al. Itch: scratching more than the surface. QJM 2003;96(1):7-26. [PMID: ] - PubMed
Van Loey 2008
Waibel 2008
-
- Waibel J, Beer K. Fractional laser resurfacing for thermal burns. Journal of Drugs in Dermatology 2008;7(1):59-61. [PMID: ] - PubMed
Wang 2003
-
- Wang CJ. An overview of shock wave therapy in musculoskeletal disorders. Chang Gung Medical Journal 2003;26(4):220-32. [PMID: ] - PubMed
Weisshaar 2003
-
- Weisshaar E, Kucenic MJ, Fleischer AB Jr. Pruritus: a review. Acta Dermato-Venereologica: Supplementum 2003;213:5–32. [PMID: ] - PubMed
Wilde 1996
-
- Wilde MI, Markham A. Ondansetron: a review of its pharmacology and preliminary clinical findings in novel applications. Drugs 1996;52:773-94. [PMID: ] - PubMed
Yakupu 2022
Yosipovitch 2013
Yüksek 2011
Zachariah 2012
Zuccaro 2022
Zylicz 2003
-
- Zylicz Z, Krajnik M, Van Sorge AA, Costantini M. Paroxetine in the treatment of severe non-dermatological pruritus: a randomized, controlled trial. Journal of Pain and Symptom Management 2003;26(6):1105-12. - PubMed
References to other published versions of this review
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials

