Short apneas and periodic breathing in preterm infants in the neonatal intensive care unit-Effects of sleep position, sleep state, and age
- PMID: 38837291
- PMCID: PMC11744229
- DOI: 10.1111/jsr.14253
Short apneas and periodic breathing in preterm infants in the neonatal intensive care unit-Effects of sleep position, sleep state, and age
Abstract
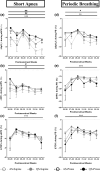
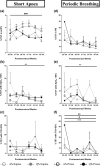
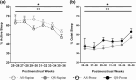
This observational study investigated the effects of sleep position and sleep state on short apneas and periodic breathing in hospitalized preterm infants longitudinally, in relation to postmenstrual age. Preterm infants (25-31 weeks gestation, n = 29) were studied fortnightly after birth until discharge, in prone and supine positions, and in quiet sleep and active sleep. The percentage of time spent in each sleep state (percentage of time in quiet sleep and percentage of time in active sleep), percentage of total sleep time spent in short apneas and periodic breathing, respectively, the percentage of falls from baseline in heart rate, arterial oxygen saturation and cerebral tissue oxygenation index during short apneas and periodic breathing, and the associated percentage of total sleep time with systemic (arterial oxygen saturation < 90%) and cerebral hypoxia (cerebral tissue oxygenation index < 55%) were analysed using a linear mixed model. Results showed that the prone position decreased (improved) the percentage of falls from baseline in arterial oxygen saturation during both short apneas and periodic breathing, decreased the proportion of infants with periodic breathing and the periodic breathing-associated percentage of total sleep time with cerebral hypoxia. The percentage of time in quiet sleep was higher in the prone position. Quiet sleep decreased the percentage of total sleep time spent in short apneas, the short apneas-associated percentage of falls from baseline in heart rate, arterial oxygen saturation, and proportion of infants with systemic hypoxia. Quiet sleep also decreased the proportion of infants with periodic breathing and percentage of total sleep time with cerebral hypoxia. The effects of sleep position and sleep state were not related to postmenstrual age. In summary, when sleep state is controlled for, the prone sleeping position has some benefits during both short apneas and periodic breathing. Quiet sleep improves cardiorespiratory stability and is increased in the prone position at the expense of active sleep, which is critical for brain maturation. This evidence should be considered in positioning preterm infants.
Keywords: NICU; periodic breathing; preterm infants; prone sleep position; short apneas.
© 2024 The Author(s). Journal of Sleep Research published by John Wiley & Sons Ltd on behalf of European Sleep Research Society.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Long Term Developmental Consequences of Short Apneas and Periodic Breathing in Preterm Infants.Pediatr Pulmonol. 2025 Jul;60(7):e71193. doi: 10.1002/ppul.71193. Pediatr Pulmonol. 2025. PMID: 40637462 Free PMC article.
-
The Effects of a Three-Stair Positioning Pillow Used for Preterm Infants on Physiologic Parameters and Sleep-Wakefulness Status: Randomized Controlled Trial.J Perinat Neonatal Nurs. 2025 Jul-Sep 01;39(3):275-283. doi: 10.1097/JPN.0000000000000867. Epub 2025 Jul 22. J Perinat Neonatal Nurs. 2025. PMID: 39374267 Clinical Trial.
-
Positioning for acute respiratory distress in hospitalised infants and children.Cochrane Database Syst Rev. 2022 Jun 6;6(6):CD003645. doi: 10.1002/14651858.CD003645.pub4. Cochrane Database Syst Rev. 2022. PMID: 35661343 Free PMC article.
-
Infant position in neonates receiving mechanical ventilation.Cochrane Database Syst Rev. 2016 Nov 7;11(11):CD003668. doi: 10.1002/14651858.CD003668.pub4. Cochrane Database Syst Rev. 2016. PMID: 27819747 Free PMC article.
-
Effects of targeting lower versus higher arterial oxygen saturations on death or disability in preterm infants.Cochrane Database Syst Rev. 2017 Apr 11;4(4):CD011190. doi: 10.1002/14651858.CD011190.pub2. Cochrane Database Syst Rev. 2017. PMID: 28398697 Free PMC article.
References
-
- Albani, M. , Bentele, K. H. , Budde, C. , & Schulte, F. J. (1985). Infant sleep apnea profile: Preterm vs. term infants. European Journal of Pediatrics, 143, 261–268. - PubMed
-
- Alderliesten, T. , Lemmers, P. M. , Smarius, J. J. , van de Vosse, R. E. , Baerts, W. , & van Bel, F. (2013). Cerebral oxygenation, extraction, and autoregulation in very preterm infants who develop peri‐intraventricular hemorrhage. The Journal of Pediatrics, 162, 698–704.e2. - PubMed
-
- Alderliesten, T. , van Bel, F. , van der Aa, N. E. , Steendijk, P. , van Haastert, I. C. , de Vries, L. S. , Groenendaal, F. , & Lemmers, P. (2019). Low cerebral oxygenation in preterm infants is associated with adverse neurodevelopmental outcome. The Journal of Pediatrics, 207, 109–116.e2. - PubMed
-
- Arditi‐Babchuk, H. , Feldman, R. , & Eidelman, A. I. (2009). Rapid eye movement (REM) in premature neonates and developmental outcome at 6 months. Infant Behavior & Development, 32, 27–32. - PubMed
-
- Aserinsky, E. , & Kleitman, N. (1953). Regularly occurring periods of eye motility, and concomitant phenomena, during sleep. Science, 118, 273–274. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

