Open tibial shaft fracture fixation strategies: intramedullary nailing, external fixation, and plating
- PMID: 38840705
- PMCID: PMC11149753
- DOI: 10.1097/OI9.0000000000000316
Open tibial shaft fracture fixation strategies: intramedullary nailing, external fixation, and plating
Abstract
Tibial shaft fractures are one of the most common orthopaedic injuries. Open tibial shaft fractures are relatively common because of the paucity of soft tissue surrounding the bone. Despite the prevalence of these injuries, the optimal fixation strategy is still a topic of debate. The purpose of this article was to review the current literature on open tibial shaft fracture fixation strategies including intramedullary nailing, external fixation, and plating.
Keywords: open fractures; outcomes; review article; tibia; trauma.
Copyright © 2024 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Orthopaedic Trauma Association.
Figures
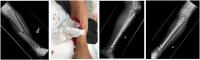


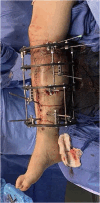

Similar articles
-
AO tubular external fixation vs. unreamed intramedullary nailing in open grade IIIA-IIIB tibial shaft fractures: a single-center randomized clinical trial.Pak J Biol Sci. 2011 Apr 15;14(8):490-5. doi: 10.3923/pjbs.2011.490.495. Pak J Biol Sci. 2011. PMID: 21936253 Clinical Trial.
-
Elastic Stable Intramedullary Nailing of Pediatric Tibial Fractures.JBJS Essent Surg Tech. 2020 Nov 19;10(4):e19.00063. doi: 10.2106/JBJS.ST.19.00063. eCollection 2020 Oct-Dec. JBJS Essent Surg Tech. 2020. PMID: 34055469 Free PMC article.
-
Functional outcomes of the knee and associated factors after intramedullary nailing of tibial diaphysial fractures at Addis Ababa Emergency, burn, and Trauma Hospital (AaEBT) hospital, Ethiopia.BMC Surg. 2023 Aug 23;23(1):250. doi: 10.1186/s12893-023-02155-8. BMC Surg. 2023. PMID: 37612685 Free PMC article.
-
Operative Fixation Versus Cast Immobilization: Tibial Shaft Fractures in Adolescents.J Pediatr Orthop. 2021 Jul 1;41(Suppl 1):S33-S38. doi: 10.1097/BPO.0000000000001806. J Pediatr Orthop. 2021. PMID: 34096535 Review.
-
Evidence-based update on the surgical treatment of pediatric tibial shaft fractures.Curr Opin Pediatr. 2019 Feb;31(1):92-102. doi: 10.1097/MOP.0000000000000704. Curr Opin Pediatr. 2019. PMID: 30461511 Review.
Cited by
-
Demographic Differences in the Surgical Management of Tibial Shaft Fractures: A Retrospective Study.Cureus. 2025 Feb 12;17(2):e78917. doi: 10.7759/cureus.78917. eCollection 2025 Feb. Cureus. 2025. PMID: 40092028 Free PMC article.
References
-
- Court-Brown CM, Caesar B. Epidemiology of adult fractures: a review. Injury. 2006;37:691–697. - PubMed
-
- Marsh JL, Slongo TF, Agel J, et al. . Fracture and dislocation classification compendium—2007: Orthopaedic Trauma Association classification, database and outcomes committee. J Orthop Trauma. 2007;21:S1. - PubMed
-
- Pape HC, Webb LX. History of open wound and fracture treatment. J Orthop Trauma. 2008;22:S133. - PubMed
-
- Egol K. Tibia and fibula shaft fractures. In: Kenneth Egol KK, Zuckerman J, eds Handbook of Fractures. Philadelphia, PA: Wolters Kluwer Health; 2020.
-
- Scott Ryan CB, O'Toole R. Open diaphyseal tibia fractures. In: Sethi M, ed. Orthopedic Traumatology: An Evidence-Based Approach. 2nd ed. Cham, Switzerland: Springer Nature; 2018.
Publication types
LinkOut - more resources
Full Text Sources
