Mohs micrographic surgery for the treatment of invasive melanoma: A systematic review with meta-analyses
- PMID: 38842170
- PMCID: PMC11760679
- DOI: 10.1111/jdv.20138
Mohs micrographic surgery for the treatment of invasive melanoma: A systematic review with meta-analyses
Abstract
Background: The use of Mohs micrographic surgery (MMS) in melanoma treatment has divided opinion and evidence-based guidelines are lacking.
Objectives: This systematic review aimed to analyse clinical outcomes for patients with invasive melanomas treated with Mohs rather than wide local excision (WLE).
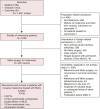
Methods: Embase, MEDLINE and Cochrane databases (to 30 August 2023) were searched for studies using Mohs to treat invasive melanoma. Outcomes of interest were local recurrence and death from melanoma.
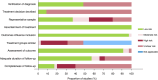
Results: Thirty-five articles involving 41,499 patients with invasive melanoma treated with Mohs were identified. Sixteen studies compared Mohs with WLE and 19 were Mohs-only, non-comparative studies. Patients treated with Mohs differed significantly from those undergoing WLE, in particular Mohs patients were older and had thinner melanomas. Two comparative studies using the same data source reported adjusted hazard ratios for melanoma-specific death and both showed no significant difference between Mohs and WLE-treated patients; 0.87 (95% CI 0.55-1.35) and 1.20 (95% CI 0.71-20.36). There was also no statistically significant difference in local recurrence risk; the unadjusted risk ratio for patients treated with Mohs was 0.46 (95% CI 0.14-1.51 p = 0.20) with moderate heterogeneity (I2 = 62%). No studies reported multivariable analyses for risk of local recurrence. Many studies generated from relatively few and often overlapping data sets have reported the use of Mohs to treat patients with invasive melanoma. Fewer studies were comparative between Mohs and WLE and these reported substantially different baseline risks of recurrence and death from melanoma between the groups. Mohs has generally been used for thinner melanomas in older patients; therefore, comparisons based on univariable analyses are likely to have been misleading.
Conclusions: On the basis of currently available data, it is not possible to reliably assess whether outcomes differ if invasive melanomas with comparable features are treated with Mohs or WLE, and randomized trial evidence will be required for reliable conclusions to be reached.
© 2024 The Author(s). Journal of the European Academy of Dermatology and Venereology published by John Wiley & Sons Ltd on behalf of European Academy of Dermatology and Venereology.
Conflict of interest statement
PG has received honoraria from MetaOptima and travel support from L'Oreal. RAS has received fees for professional services from MetaOptima Technology Inc., F. Hoffmann‐La Roche Ltd, Evaxion, Provectus Biopharmaceuticals Australia, Qbiotics, Novartis, Merck Sharp & Dohme, NeraCare, AMGEN Inc., Bristol‐Myers Squibb, Myriad Genetics and GlaxoSmithKline. JFT has received honoraria for advisory board participation from BMS Australia, MSD Australia, GSK and Provectus Biopharmaceuticals, and travel support from GSK and Provectus Biopharmaceuticals. Other authors have nothing to declare.
Figures
Similar articles
-
Sentinel lymph node biopsy followed by lymph node dissection for localised primary cutaneous melanoma.Cochrane Database Syst Rev. 2015 May 16;2015(5):CD010307. doi: 10.1002/14651858.CD010307.pub2. Cochrane Database Syst Rev. 2015. PMID: 25978975 Free PMC article.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
[Volume and health outcomes: evidence from systematic reviews and from evaluation of Italian hospital data].Epidemiol Prev. 2013 Mar-Jun;37(2-3 Suppl 2):1-100. Epidemiol Prev. 2013. PMID: 23851286 Italian.
-
Sertindole for schizophrenia.Cochrane Database Syst Rev. 2005 Jul 20;2005(3):CD001715. doi: 10.1002/14651858.CD001715.pub2. Cochrane Database Syst Rev. 2005. PMID: 16034864 Free PMC article.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
References
-
- Prieto VG, Argenyi ZB, Barnhill RL, Duray PH, Elenitsas R, From L, et al. Are en face frozen sections accurate for diagnosing margin status in melanocytic lesions? Am J Clin Pathol. 2003;120(2):203–208. - PubMed
-
- Pride RLD, Miller CJ, Murad MH, Erwin PJ, Brewer JD. Local recurrence of melanoma is higher after wide local excision versus Mohs micrographic surgery or staged excision: a systematic review and meta‐analysis. Dermatol Surg. 2022;48(2):164–170. - PubMed
-
- Bednar ED, Zon M, Abu‐Hilal M. Morbidity and mortality of melanoma on the trunk and extremities treated with Mohs surgery versus wide excision: a systematic review. Dermatol Surg. 2022;48(1):1–6. - PubMed
-
- Theunissen CCW, Lee MH, Murad FG, Waldman AH. Systematic review of the role of Mohs micrographic surgery in the Management of Early‐Stage Melanoma of the head and neck. Dermatol Surg. 2021;47(9):1185–1189. - PubMed
-
- Bittar PG, Bittar JM, Etzkorn JR, Brewer JD, Aizman L, Shin TM, et al. Systematic review and meta‐analysis of local recurrence rates of head and neck cutaneous melanomas after wide local excision, Mohs micrographic surgery, or staged excision. J Am Acad Dermatol. 2021;85(3):681–692. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical