Improving medical students recognizing surgery of glioblastoma removal/decompressive craniectomy via physical lifelike brain simulator training
- PMID: 38844925
- PMCID: PMC11155129
- DOI: 10.1186/s12909-024-05621-w
Improving medical students recognizing surgery of glioblastoma removal/decompressive craniectomy via physical lifelike brain simulator training
Abstract
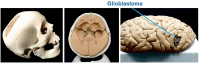
Background: This study aims to investigate the benefits of employing a Physical Lifelike Brain (PLB) simulator for training medical students in performing craniotomy for glioblastoma removal and decompressive craniectomy.
Methods: This prospective study included 30 medical clerks (fifth and sixth years in medical school) at a medical university. Before participating in the innovative lesson, all students had completed a standard gross anatomy course as part of their curriculum. The innovative lesson involved PLB Simulator training, after which participants completed the Learning Satisfaction/Confidence Perception Questionnaire and some received qualitative interviews.
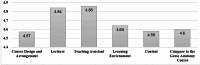
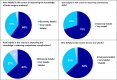
Results: The average score of students' overall satisfaction with the innovative lesson was 4.71 out of a maximum of 5 (SD = 0.34). After the lesson, students' confidence perception level improved significantly (t = 9.38, p < 0.001, effect size = 1.48), and the average score improved from 2,15 (SD = 1.02) to 3.59 (SD = 0.93). 60% of the students thought that the innovative lesson extremely helped them understand the knowledge of surgical neuroanatomy more, 70% believed it extremely helped them improve their skills in burr hole, and 63% thought it was extremely helpful in improving the patient complications of craniotomy with the removal of glioblastoma and decompressive craniectomy after completing the gross anatomy course.
Conclusion: This innovative lesson with the PLB simulator successfully improved students' craniotomy knowledge and skills.
Keywords: Additive Manufacturing; Decompressive Craniectomy; Glioblastoma removal; Medical Education; Physical lifelike Brain Simulator.
© 2024. The Author(s).
Conflict of interest statement
The authors declare no conflict of interest.
Figures


References
-
- Fernandes C, De Vleeschouwer S. Glioblastoma. Codon Publications Copyright: The Authors.: Brisbane (AU); 2017. Current standards of Care in Glioblastoma Therapy. - PubMed
-
- Fava A, Gorgoglione N, De Angelis M, Esposito V, di Russo P. Key role of microsurgical dissections on cadaveric specimens in neurosurgical training: setting up a new research anatomical laboratory and defining neuroanatomical milestones. Front Surg. 2023;10:1145881. doi: 10.3389/fsurg.2023.1145881. - DOI - PMC - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

