Insulin resistance assessed by estimated glucose disposal rate and risk of incident cardiovascular diseases among individuals without diabetes: findings from a nationwide, population based, prospective cohort study
- PMID: 38844981
- PMCID: PMC11157942
- DOI: 10.1186/s12933-024-02256-5
Insulin resistance assessed by estimated glucose disposal rate and risk of incident cardiovascular diseases among individuals without diabetes: findings from a nationwide, population based, prospective cohort study
Abstract
Background: Recent studies have suggested that insulin resistance (IR) contributes to the development of cardiovascular diseases (CVD), and the estimated glucose disposal rate (eGDR) is considered to be a reliable surrogate marker of IR. However, most existing evidence stems from studies involving diabetic patients, potentially overstating the effects of eGDR on CVD. Therefore, the primary objective of this study is to examine the relationship of eGDR with incidence of CVD in non-diabetic participants.
Method: The current analysis included individuals from the China Health and Retirement Longitudinal Study (CHARLS) who were free of CVD and diabetes mellitus but had complete data on eGDR at baseline. The formula for calculating eGDR was as follows: eGDR (mg/kg/min) = 21.158 - (0.09 × WC) - (3.407 × hypertension) - (0.551 × HbA1c) [WC (cm), hypertension (yes = 1/no = 0), and HbA1c (%)]. The individuals were categorized into four subgroups according to the quartiles (Q) of eGDR. Crude incidence rate and hazard ratios (HRs) with 95% confidence intervals (CIs) were computed to investigate the association between eGDR and incident CVD, with the lowest quartile of eGDR (indicating the highest grade of insulin resistance) serving as the reference. Additionally, the multivariate adjusted restricted cubic spine (RCS) was employed to examine the dose-response relationship.
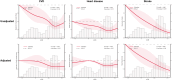
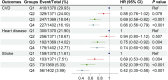
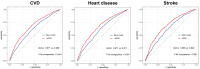
Results: We included 5512 participants in this study, with a mean age of 58.2 ± 8.8 years, and 54.1% were female. Over a median follow-up duration of 79.4 months, 1213 incident CVD cases, including 927 heart disease and 391 stroke, were recorded. The RCS curves demonstrated a significant and linear relationship between eGDR and all outcomes (all P for non-linearity > 0.05). After multivariate adjustment, the lower eGDR levels were founded to be significantly associated with a higher risk of CVD. Compared with participants with Q1 of eGDR, the HRs (95% CIs) for those with Q2 - 4 were 0.88 (0.76 - 1.02), 0.69 (0.58 - 0.82), and 0.66 (0.56 - 0.79). When assessed as a continuous variable, per 1.0-SD increase in eGDR was associated a 17% (HR: 0.83, 95% CI: 0.78 - 0.89) lower risk of CVD, with the subgroup analyses indicating that smoking status modified the association (P for interaction = 0.012). Moreover, the mediation analysis revealed that obesity partly mediated the association. Additionally, incorporating eGDR into the basic model considerably improve the predictive ability for CVD.
Conclusion: A lower level of eGDR was found to be associated with increased risk of incident CVD among non-diabetic participants. This suggests that eGDR may serve as a promising and preferable predictor and intervention target for CVD.
Keywords: Cardiovascular diseases; Estimated glucose disposal rate; Insulin resistance; Non-diabetes; Predictive performance.
© 2024. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

References
-
- Roth GA, Mensah GA, Johnson CO, Addolorato G, Ammirati E, Baddour LM, Barengo NC, Beaton AZ, Benjamin EJ, Benziger CP, et al. Global burden of cardiovascular diseases and risk factors, 1990–2019: update from the GBD 2019 study. J Am Coll Cardiol. 2020;76(25):2982–3021. doi: 10.1016/j.jacc.2020.11.010. - DOI - PMC - PubMed
-
- GBD 2017 Causes of Death Collaborators Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392(10159):1736–1788. doi: 10.1016/S0140-6736(18)32203-7. - DOI - PMC - PubMed
-
- Zhang Z, Zhao L, Lu Y, Meng X, Zhou X. Association between non-insulin-based insulin resistance indices and cardiovascular events in patients undergoing percutaneous coronary intervention: a retrospective study. Cardiovasc Diabetol. 2023;22(1):161. doi: 10.1186/s12933-023-01898-1. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

