Male Breast Cancer: Imaging Considerations for Diagnosis and Surveillance
- PMID: 38855781
- PMCID: PMC11161189
- DOI: 10.14740/jocmr5169
Male Breast Cancer: Imaging Considerations for Diagnosis and Surveillance
Abstract
Male breast cancer accounts for less than 1% of all breast cancer cases. The important risk factors for the development of male breast cancer are family history, genetic mutations, obesity, liver disease, alcoholism, exogenous estrogen administration, and radiation exposure to the chest area. Despite its rarity, numerous studies have investigated the data on imaging considerations (mammogram, ultrasound, and magnetic resonance imaging (MRI)), but have addressed only certain aspects of male breast cancer. A comprehensive approach on the imaging characteristics, timing of imaging, prognostication based on imaging characteristics, and follow-up strategies in male breast cancer are still lacking. The purpose of this review article was to provide a comprehensive overview of the imaging findings, optimal timing to obtain imaging, and the appropriate follow-up strategies in male breast cancer survivors. This article also describes how imaging modalities can aid in determining prognosis. By addressing this knowledge gap, the article provides valuable insights for clinicians managing this uncommon yet clinically significant disease.
Keywords: MRI in male breast cancer; Male breast cancer; Mammogram; Screening; Sonogram; Surveillance.
Copyright 2024, Thomas et al.
Conflict of interest statement
None to declare.
Figures


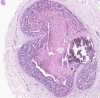
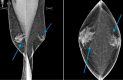
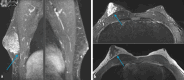

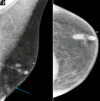
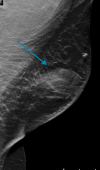


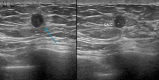
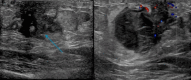
Similar articles
-
Cancer screening with digital mammography for women at average risk for breast cancer, magnetic resonance imaging (MRI) for women at high risk: an evidence-based analysis.Ont Health Technol Assess Ser. 2010;10(3):1-55. Epub 2010 Mar 1. Ont Health Technol Assess Ser. 2010. PMID: 23074406 Free PMC article.
-
Prospective study of the efficacy of breast magnetic resonance imaging and mammographic screening in survivors of Hodgkin lymphoma.J Clin Oncol. 2013 Jun 20;31(18):2282-8. doi: 10.1200/JCO.2012.46.5732. Epub 2013 Apr 22. J Clin Oncol. 2013. PMID: 23610104
-
Screening mammography for women aged 40 to 49 years at average risk for breast cancer: an evidence-based analysis.Ont Health Technol Assess Ser. 2007;7(1):1-32. Epub 2007 Jan 1. Ont Health Technol Assess Ser. 2007. PMID: 23074501 Free PMC article.
-
Current and Emerging Therapies for HER2-Positive Women With Metastatic Breast Cancer.J Adv Pract Oncol. 2017 Mar;8(2):164-168. Epub 2017 Mar 1. J Adv Pract Oncol. 2017. PMID: 29900024 Free PMC article. Review.
-
Breast MRI: Clinical Indications, Recommendations, and Future Applications in Breast Cancer Diagnosis.Curr Oncol Rep. 2023 Apr;25(4):257-267. doi: 10.1007/s11912-023-01372-x. Epub 2023 Feb 7. Curr Oncol Rep. 2023. PMID: 36749493 Review.
References
-
- BREASTCANCER.ORG. U.S. Breast Cancer Statistics. 2022. Available from: https://www.breastcancer.org/symptoms/understand_bc/statistics#:∼:text=A....
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous
