Pharmaceutical targeting of the cannabinoid type 1 receptor impacts the crosstalk between immune cells and islets to reduce insulitis in humans
- PMID: 38864887
- PMCID: PMC11410908
- DOI: 10.1007/s00125-024-06193-6
Pharmaceutical targeting of the cannabinoid type 1 receptor impacts the crosstalk between immune cells and islets to reduce insulitis in humans
Erratum in
-
Correction: Pharmaceutical targeting of the cannabinoid type 1 receptor impacts the crosstalk between immune cells and islets to reduce insulitis in humans.Diabetologia. 2025 Apr;68(4):902. doi: 10.1007/s00125-025-06372-z. Diabetologia. 2025. PMID: 39954060 Free PMC article. No abstract available.
Abstract
Aims/hypothesis: Insulitis, a hallmark of inflammation preceding autoimmune type 1 diabetes, leads to the eventual loss of functional beta cells. However, functional beta cells can persist even in the face of continuous insulitis. Despite advances in immunosuppressive treatments, maintaining functional beta cells to prevent insulitis progression and hyperglycaemia remains a challenge. The cannabinoid type 1 receptor (CB1R), present in immune cells and beta cells, regulates inflammation and beta cell function. Here, we pioneer an ex vivo model mirroring human insulitis to investigate the role of CB1R in this process.
Methods: CD4+ T lymphocytes were isolated from peripheral blood mononuclear cells (PBMCs) from male and female individuals at the onset of type 1 diabetes and from non-diabetic individuals, RNA was extracted and mRNA expression was analysed by real-time PCR. Single beta cell expression from donors with type 1 diabetes was obtained from data mining. Patient-derived human islets from male and female cadaveric donors were 3D-cultured in solubilised extracellular matrix gel in co-culture with the same donor PBMCs, and incubated with cytokines (IL-1β, TNF-α, IFN-γ) for 24-48 h in the presence of vehicle or increasing concentrations of the CB1R blocker JD-5037. Expression of CNR1 (encoding for CB1R) was ablated using CRISPR/Cas9 technology. Viability, intracellular stress and signalling were assayed by live-cell probing and real-time PCR. The islet function measured as glucose-stimulated insulin secretion was determined in a perifusion system. Infiltration of immune cells into the islets was monitored by microscopy. Non-obese diabetic mice aged 7 weeks were treated for 1 week with JD-5037, then euthanised. Profiling of immune cells infiltrated in the islets was performed by flow cytometry.
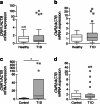
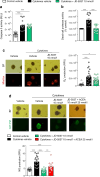
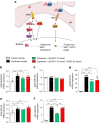
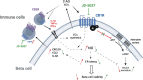
Results: CNR1 expression was upregulated in circulating CD4+ T cells from individuals at type 1 diabetes onset (6.9-fold higher vs healthy individuals) and in sorted islet beta cells from donors with type 1 diabetes (3.6-fold higher vs healthy counterparts). The peripherally restricted CB1R inverse agonist JD-5037 arrested the initiation of insulitis in humans and mice. Mechanistically, CB1R blockade prevented islet NO production and ameliorated the ATF6 arm of the unfolded protein response. Consequently, cyto/chemokine expression decreased in human islets, leading to sustained islet cell viability and function.
Conclusions/interpretation: These results suggest that CB1R could be an interesting target for type 1 diabetes while highlighting the regulatory mechanisms of insulitis. Moreover, these findings may apply to type 2 diabetes where islet inflammation is also a pathophysiological factor.
Data availability: Transcriptomic analysis of sorted human beta cells are from Gene Expression Omnibus database, accession no. GSE121863, available at https://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSM3448161 .
Keywords: CB1R; Cannabinoid receptor; Endocannabinoid; Insulitis; Islet of Langerhans; Peripheral CB1R inverse agonist; Type 1 diabetes.
© 2024. The Author(s).
Figures




References
-
- International Diabetes Federation IDF Diabetes Atlas. https://www.idf.org/e-library/epidemiology-research/diabetes-atlas.html. Accessed 15 May 2018
MeSH terms
Substances
Grants and funding
- ANR-10-LABX-0046/Agence Nationale de la Recherche (Laboratoire d'excellence European Genomic Institute for Diabetes)
- C-0070-2012/Consejeria de Salud y Familias, Junta de Andalucia
- C1-0018-2019/Consejeria de Salud y Familias, Junta de Andalucia
- PI-0318-2018/Consejeria de Salud y Familias, Junta de Andalucia
- CPC22133/Sociedad Española de Diabetes
LinkOut - more resources
Full Text Sources
Medical
Research Materials

