Efficacy of Baclofen as Add-on Therapy for Refractory Gastroesophageal Reflux Disease: A Meta-analysis
- PMID: 38869961
- PMCID: PMC12165541
- DOI: 10.1097/MCG.0000000000002021
Efficacy of Baclofen as Add-on Therapy for Refractory Gastroesophageal Reflux Disease: A Meta-analysis
Abstract
Objectives: As a GABAB receptor agonist, baclofen has demonstrated efficacy in alleviating symptoms of refractory gastroesophageal reflux disease (r-GERD). This meta-analysis aims to evaluate the safety and effectiveness of baclofen as an add-on therapy for this condition.
Method: We conducted a comprehensive search of the PubMed, Embase, and Web of Science databases for studies published up until October 2023. Subsequently, we performed a meta-analysis encompassing all eligible trials.
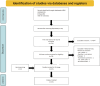
Results: From 719 records, 10 studies were included, most of these studies were moderate risk. The findings demonstrated that the addition of baclofen as a supplementary treatment effectively improves symptoms (GERD Q score) in r-GERD (standardized mean difference=-0.78, 95% CI: -1.06 to -0.51, I2 =0%). The addition of this treatment also resulted in a decrease in the frequency of nonacidic reflux episodes (standardized mean difference=-0.93, 95% CI: -1.49 to -0.37, I2 =63%) and an improvement in DeMeester scores (standardized mean difference=-0.82, 95% CI: -1.61 to -0.04, I2 =81%) among patients with r-GERD when compared with the use of proton pump inhibitor (PPI) drugs alone. However, no significant disparity was observed in terms of reducing acid reflux episodes (standardized mean difference=-0.12, 95% CI: -0.49 to 0.19, I2 =0%) and proximal reflux (standardized mean difference=-0.47, 95% CI: -1.08 to 0.14, I2 =60%).
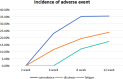
Conclusion: Baclofen as an add-on treatment can effectively improve the symptoms of patients with r-GERD and reduce the incidence of nonacidic reflux and improve DeMeester score. However, long-term use of baclofen leads to an increased incidence of side effects and is not effective in reducing the occurrence of acid reflux.
Keywords: MII-PH; baclofen; gastroesophageal reflux disease; medical treatment; refractory gastroesophageal reflux disease.
Copyright © 2024 The Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
Supported by: Natural Science Foundation of Beijing Province (L182048).
Figures
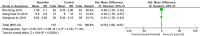



Similar articles
-
Alginate therapy is effective treatment for gastroesophageal reflux disease symptoms: a systematic review and meta-analysis.Dis Esophagus. 2017 Feb 1;30(2):1-8. doi: 10.1111/dote.12535. Dis Esophagus. 2017. PMID: 27671545
-
Alginate therapy is effective treatment for GERD symptoms: a systematic review and meta-analysis.Dis Esophagus. 2017 May 1;30(5):1-9. doi: 10.1093/dote/dow020. Dis Esophagus. 2017. PMID: 28375448 Free PMC article.
-
Treatment of PPI-resistant gastro-oesophageal reflux: A systematic review.Arab J Gastroenterol. 2018 Jun;19(2):51-55. doi: 10.1016/j.ajg.2018.02.007. Epub 2018 Jun 20. Arab J Gastroenterol. 2018. PMID: 29935866
-
Does treatment with proton pump inhibitors for gastroesophageal reflux disease (GERD) improve asthma symptoms in children with asthma and GERD? A systematic review.J Investig Allergol Clin Immunol. 2009;19(1):1-5. J Investig Allergol Clin Immunol. 2009. PMID: 19274922
-
Efficacy of proton-pump inhibitors in children with gastroesophageal reflux disease: a systematic review.Pediatrics. 2011 May;127(5):925-35. doi: 10.1542/peds.2010-2719. Epub 2011 Apr 4. Pediatrics. 2011. PMID: 21464183
References
-
- Spechler SJ, Hunter JG, Jones KM, et al. Randomized trial of medical versus surgical treatment for refractory heartburn. N Engl J Med. 2019;381:1513–1523. - PubMed
-
- Roman S, Mion F. Refractory GERD, beyond proton pump inhibitors. Curr Opin Pharmacol. 2018;43:99–103. - PubMed
-
- Mittal RK, Holloway RH, Penagini R, et al. Transient lower esophageal sphincter relaxation. Gastroenterology. 1995;109:601–610. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

