Surgical Management of Hidradenitis Suppurativa
- PMID: 38872991
- PMCID: PMC11175856
- DOI: 10.1097/GOX.0000000000005860
Surgical Management of Hidradenitis Suppurativa
Abstract
Hidradenitis suppurativa (HS) is a chronic, relapsing inflammatory disease of the skin, characterized by recurrent draining sinuses and abscesses, predominantly in skin folds carrying terminal hairs and apocrine glands. Treatment for this debilitating disease has been medical management with antibiotics and immune modulators. With the advent of better reconstructive surgical techniques, the role of surgery in the treatment of HS has expanded, from being a last resort to a modality that is deployed earlier. Larger defects can be more easily reconstructed, allowing for a more radical excision of diseased areas. Locoregional flaps, perforator flaps, and propeller flaps that use the fasciocutaneous tissue allow reconstruction of defects with similar tissue, and provide better cosmetic and functional outcomes. They are easy to execute and can be performed even in resource-poor settings with concurrent use of immune modulators and postoperative antibiotics. Hidradenitis can be successfully treated with surgery in early stages as well as severe disease, due to the advances in understanding disease behavior, multidisciplinary care, and advanced reconstructive techniques. Coupled with a multidisciplinary care team, surgery offers a durable, lasting cure for HS, significantly reducing disease morbidity.
Copyright © 2024 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of The American Society of Plastic Surgeons.
Conflict of interest statement
The authors have no financial interest to declare in relation to the content of this article.
Figures
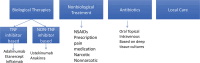



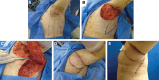



References
-
- Sachdeva M, Shah M, Alavi A. Race-specific prevalence of hidradenitis suppurativa. J Cutan Med Surg. 2021;25:177–187. - PubMed
-
- Yang EJ, Beck KM, Bhutani T, et al. . Pharmacy costs of systemic medications for hidradenitis suppurativa in the United States. J Dermatol Treat. 2018;30:519–521. - PubMed
-
- Kirby JS, Miller JJ, Adams DR, et al. . Health care utilization patterns and costs for patients with hidradenitis suppurativa. JAMA Dermatol. 2014;150:937–944. - PubMed
-
- Zouboulis CC, Desai N, Emtestam L, et al. . European S1 guideline for the treatment of hidradenitis suppurativa/acne inversa. J Eur Acad Dermatol Venereol. 2015;29:619–644. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
