Prognostic factors and treatment impact on overall survival in patients with renal neuroendocrine tumour
- PMID: 38873350
- PMCID: PMC11168774
- DOI: 10.1002/bco2.341
Prognostic factors and treatment impact on overall survival in patients with renal neuroendocrine tumour
Erratum in
-
Erratum.BJUI Compass. 2024 Dec 30;5(12):1324-1329. doi: 10.1002/bco2.482. eCollection 2024 Dec. BJUI Compass. 2024. PMID: 39744071 Free PMC article.
Abstract
Background: Renal neuroendocrine neoplasms (R-NEN) are exceptionally rare tumours characterized by high mortality rates.
Objective: The objective of this study is to analyse prognostic factors and treatment impact on overall survival in patients with R-NEN.
Design setting and participants: We identified all patients with R-NEN in the National Cancer Database (NCDB) from 2004 to 2019 and identified prognostic factors for improved survival.
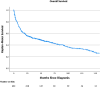
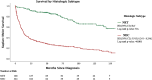
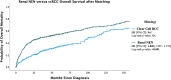
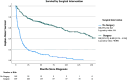
Results and limitations: Of 542 R-NEN cases, 166 (31%) were neuroendocrine tumour grade 1 (NET-G1), 14 (3%) were neuroendocrine tumour grade 2 (NET-G2), 169 (31%) were neuroendocrine carcinoma (NEC-NOS), 18 (3%) were large cell neuroendocrine carcinoma (LC-NEC) and 175 (32%) were small cell neuroendocrine carcinoma (SC-NEC). Median overall survival for all patients in the study was 44.88 months (SE, 4.265; 95% CI, 27.57-62.19). Median overall survival was 7.89 months (SE 0.67; 95% CI, 6.58-9.20) for patients without surgical intervention and 136.61 months (SE 16.44; 95% CI, 104.38-168.84, p < 0.001) for patients who underwent surgery. Increased age (HR, 1.05; 95% CI, 1.03-1.06; p < 0.001), T4 stage disease (HR, 3.17; 95% CI, 1.96-5.1; p < 0.001), NEC-NOS histology (HR, 2.82; 95% CI, 1.64-4.86; p < 0.001), LC-NEC histology (HR, 2.73; 95% CI, 1.04-7.17; p = 0.041) and SC-NEC histology (HR, 5.17; 95% CI, 2.95-9.05; p < 0.001) were all positive predictors of worsening overall survival. The main limitation of the study is its retrospective design.
Conclusion: R-NEN is an aggressive tumour characterized by high mortality rates. Surgery continues to be the mainstay of treatment and has shown to provide a survival benefit for most patients.
Patient summary: R-NEN is composed of several tumour histologies that differ based on their aggressiveness with NEC-NOS and SC-NEC being the most lethal. Surgery, predominantly through minimally invasive approaches, is the mainstay of treatment and has a clear survival benefit.
Keywords: kidney tumours; neuroendocrine carcinoma; partial nephrectomy; radical nephrectomy; renal cancer.
© 2024 The Authors. BJUI Compass published by John Wiley & Sons Ltd on behalf of BJU International Company.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
LinkOut - more resources
Full Text Sources
