Polymicrobial brain abscesses: A complex condition with diagnostic and therapeutic challenges
- PMID: 38874452
- PMCID: PMC11413443
- DOI: 10.1093/jnen/nlae058
Polymicrobial brain abscesses: A complex condition with diagnostic and therapeutic challenges
Abstract
Brain abscesses (BA) are focal parenchymal infections that remain life-threatening conditions. Polymicrobial BAs (PBAs) are complex coinfections of bacteria or bacterial and nonbacterial pathogens such as fungi or parasites, with diagnostic and therapeutic challenges. In this article, we comprehensively review the prevalence, pathogenesis, clinical manifestations, and microbiological, histopathological, and radiological features of PBAs, as well as treatment and prognosis. While PBAs and monomicrobial BAs have some similarities such as nonspecific clinical presentations, PBAs are more complex in their pathogenesis, pathological, and imaging presentations. The diagnostic challenges of PBAs include nonspecific imaging features at early stages and difficulties in identification of some pathogens by routine techniques without the use of molecular analysis. Imaging of late-stage PBAs demonstrates increased heterogeneity within lesions, which corresponds to variable histopathological features depending on the dominant pathogen-induced changes in different areas. This heterogeneity is particularly marked in cases of coinfections with nonbacterial pathogens such as Toxoplasma gondii. Therapeutic challenges in the management of PBAs include initial medical therapy for possibly underrecognized coinfections prior to identification of multiple pathogens and subsequent broad-spectrum antimicrobial therapy to eradicate identified pathogens. PBAs deserve more awareness to facilitate prompt and appropriate treatment.
Keywords: abscess stage; brain abscess; coinfection; lesion heterogeneity; pathogen; pathogenic complexity; polymicrobial.
© The Author(s) 2024. Published by Oxford University Press on behalf of American Association of Neuropathologists, Inc.
Conflict of interest statement
None declared.
Figures
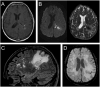

Similar articles
-
Clinicopathological heterogeneity and complexity of polymicrobial brain abscesses.J Neurol Sci. 2025 Jun 15;473:123525. doi: 10.1016/j.jns.2025.123525. Epub 2025 May 2. J Neurol Sci. 2025. PMID: 40334432
-
Idiopathic (Genetic) Generalized Epilepsy.2024 Feb 12. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2024 Feb 12. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 31536218 Free Books & Documents.
-
Uncommon Non-MS Demyelinating Disorders of the Central Nervous System.Curr Neurol Neurosci Rep. 2025 Jul 1;25(1):45. doi: 10.1007/s11910-025-01432-8. Curr Neurol Neurosci Rep. 2025. PMID: 40591029 Review.
-
Signs and symptoms to determine if a patient presenting in primary care or hospital outpatient settings has COVID-19.Cochrane Database Syst Rev. 2022 May 20;5(5):CD013665. doi: 10.1002/14651858.CD013665.pub3. Cochrane Database Syst Rev. 2022. PMID: 35593186 Free PMC article.
-
Short-Term Memory Impairment.2024 Jun 8. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2024 Jun 8. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 31424720 Free Books & Documents.
References
-
- Brouwer MC, Tunkel AR, van de Beek D. Brain abscess. N Engl J Med. 2014;371(18):1758. - PubMed
-
- Mathisen GE, Johnson JP. Brain abscess. Clin Infect Dis. 1997;25(4):763-779. - PubMed
-
- Kameda-Smith MM, Duda T, Duncan DB, et al. Retrospective review of the clinical outcomes of surgically managed patients with intracranial abscesses: a single-center review. World Neurosurg. 2022;165:e697-e711. - PubMed
-
- Su TM, Lan CM, Tsai YD, et al. Multiloculated pyogenic brain abscess: experience in 25 patients. Neurosurgery. 2008;62(Suppl 2):556-561. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

