Patterns of cognitive domain abnormalities enhance discrimination of dementia risk prediction: The ARIC study
- PMID: 38877664
- PMCID: PMC11247695
- DOI: 10.1002/alz.13876
Patterns of cognitive domain abnormalities enhance discrimination of dementia risk prediction: The ARIC study
Abstract
Introduction: The contribution of neuropsychological assessments to risk assessment for incident dementia is underappreciated.
Methods: We analyzed neuropsychological testing results in dementia-free participants in the Atherosclerosis Risk in Communities (ARIC) study. We examined associations of index domain-specific neuropsychological test performance with incident dementia using cumulative incidence curves and Cox proportional hazards models.
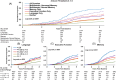
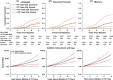
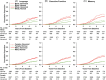
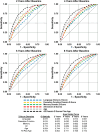
Results: Among 5296 initially dementia-free participants (mean [standard deviation] age of 75.8 [5.1] years; 60.1% women, 22.2% Black) over a median follow-up of 7.9 years, the covariate-adjusted hazard ratio varied substantially depending on the pattern of domain-specific performance and age, in an orderly manner from single domain language abnormalities (lowest risk) to single domain executive or memory abnormalities, to multidomain abnormalities including memory (highest risk).
Discussion: By identifying normatively defined cognitive abnormalities by domains based on neuropsychological test performance, there is a conceptually orderly and age-sensitive spectrum of risk for incident dementia that provides valuable information about the likelihood of progression.
Highlights: Domain-specific cognitive profiles carry enhanced prognostic value compared to mild cognitive impairment. Single-domain non-amnestic cognitive abnormalities have the most favorable prognosis. Multidomain amnestic abnormalities have the greatest risk for incident dementia. Patterns of domain-specific risks are similar by sex and race.
Keywords: incident dementia; mild cognitive impairment; neuropsychological testing.
© 2024 The Author(s). Alzheimer's & Dementia published by Wiley Periodicals LLC on behalf of Alzheimer's Association.
Conflict of interest statement
David S. Knopman reports no conflicts with respect to the current work. Knopman serves on a Data Safety Monitoring Board for the Dominantly Inherited Alzheimer Network Treatment Unit study and a study of nicorandil for the treatment of hippocampal sclerosis of aging sponsored by the University of Kentucky. He was a site investigator in clinical trials sponsored by Biogen, Lilly Pharmaceuticals, and the University of Southern California, and is currently a site investigator in a trial in frontotemporal degeneration with Alector. He has served as a consultant for Roche, Biovie, Linus Health, and Alzeca Biosciences but receives no personal compensation. James Russell Pike has no relationships to disclose. Rebecca F. Gottesman has no relationships to disclose. A. Richey Sharrett has no relationships to disclose. B. Gwen Windham has no relationships to disclose. Thomas H Mosley has no relationships to disclose. Kevin Sullivan has no relationships to disclose. Marilyn S. Albert has no relationships to disclose. Keenan A. Walker has no relationships to disclose. Sevil Yasar has no relationships to disclose. Sheila Burgard has no relationships to disclose. David Li has no relationships to disclose. Alden L Gross has no relationships to disclose. Author disclosures are available in the supporting information.
Figures

Similar articles
-
Spectrum of cognition short of dementia: Framingham Heart Study and Mayo Clinic Study of Aging.Neurology. 2015 Nov 10;85(19):1712-21. doi: 10.1212/WNL.0000000000002100. Epub 2015 Oct 9. Neurology. 2015. PMID: 26453643 Free PMC article. Review.
-
Mild cognitive impairment in a community sample: the Sydney Memory and Ageing Study.Alzheimers Dement. 2013 May;9(3):310-317.e1. doi: 10.1016/j.jalz.2011.11.010. Epub 2012 Oct 27. Alzheimers Dement. 2013. PMID: 23110866
-
Neuropsychological Criteria for Mild Cognitive Impairment and Dementia Risk in the Framingham Heart Study.J Int Neuropsychol Soc. 2016 Oct;22(9):937-943. doi: 10.1017/S1355617716000199. Epub 2016 Mar 31. J Int Neuropsychol Soc. 2016. PMID: 27029348 Free PMC article.
-
Memory Binding Test Predicts Incident Amnestic Mild Cognitive Impairment.J Alzheimers Dis. 2016 Jul 14;53(4):1585-1595. doi: 10.3233/JAD-160291. J Alzheimers Dis. 2016. PMID: 27540964
-
Motoric cognitive risk syndrome, incident cognitive impairment and morphological brain abnormalities: Systematic review and meta-analysis.Maturitas. 2019 May;123:45-54. doi: 10.1016/j.maturitas.2019.02.006. Epub 2019 Feb 18. Maturitas. 2019. PMID: 31027677
Cited by
-
Population Attributable Fraction of Incident Dementia Associated With Hearing Loss.JAMA Otolaryngol Head Neck Surg. 2025 Jun 1;151(6):568-575. doi: 10.1001/jamaoto.2025.0192. JAMA Otolaryngol Head Neck Surg. 2025. PMID: 40244612
-
Lifetime risk and projected burden of dementia.Nat Med. 2025 Mar;31(3):772-776. doi: 10.1038/s41591-024-03340-9. Epub 2025 Jan 13. Nat Med. 2025. PMID: 39806070
-
COVID-19 and Cognitive Change in a Community-Based Cohort.JAMA Netw Open. 2025 Jun 2;8(6):e2518648. doi: 10.1001/jamanetworkopen.2025.18648. JAMA Netw Open. 2025. PMID: 40587126 Free PMC article.
-
Cognitive benefits of hearing intervention vary by risk of cognitive decline: A secondary analysis of the ACHIEVE trial.Alzheimers Dement. 2025 May;21(5):e70156. doi: 10.1002/alz.70156. Alzheimers Dement. 2025. PMID: 40369891 Free PMC article. Clinical Trial.
-
Contribution of Modifiable Midlife and Late-Life Vascular Risk Factors to Incident Dementia.JAMA Neurol. 2025 Jul 1;82(7):644-654. doi: 10.1001/jamaneurol.2025.1495. JAMA Neurol. 2025. PMID: 40455489
References
-
- Albert M, DeKosky ST, Dickson D, et al. The diagnosis of mild cognitive impairment due to Alzheimer's disease: recommendations from the National Institute on Aging–Alzheimer's Association workgroups on diagnostic guidelines for Alzheimer's disease. Alzheimers Dement. 2011;7(3):270‐279. - PMC - PubMed
-
- Mitchell AJ, Shiri‐Feshki M. Rate of progression of mild cognitive impairment to dementia–meta‐analysis of 41 robust inception cohort studies. Acta Psychiatr Scand. 2009;119(4):252‐265. - PubMed
Publication types
MeSH terms
Grants and funding
- DC/NIDCD NIH HHS/United States
- 75N92022D00002/HL/NHLBI NIH HHS/United States
- U01 HL096917/HL/NHLBI NIH HHS/United States
- U01HL096902/ARIC Neurocognitive Study
- National Institute of Neurological Disease and Stroke Intramural Research Program
- U01HL096917/ARIC Neurocognitive Study
- 75N92022D00004/HL/NHLBI NIH HHS/United States
- U01HL096812/ARIC Neurocognitive Study
- U01 HL096814/HL/NHLBI NIH HHS/United States
- 75N92022D00003/HL/NHLBI NIH HHS/United States
- U01 HL096899/HL/NHLBI NIH HHS/United States
- 75N92022D00001/HL/NHLBI NIH HHS/United States
- U01 HL096812/HL/NHLBI NIH HHS/United States
- AG/NIA NIH HHS/United States
- U01 HL096902/HL/NHLBI NIH HHS/United States
- U01HL096814/ARIC Neurocognitive Study
- National Institute on Aging's Intramural Research Program
- NS/NINDS NIH HHS/United States
- 75N92022D00005/HL/NHLBI NIH HHS/United States
- NH/NIH HHS/United States
- U01HL096899/ARIC Neurocognitive Study
LinkOut - more resources
Full Text Sources
Medical

