Metabolomics and Cardiovascular Risk in Patients with Heart Failure: A Systematic Review and Meta-Analysis
- PMID: 38891881
- PMCID: PMC11172189
- DOI: 10.3390/ijms25115693
Metabolomics and Cardiovascular Risk in Patients with Heart Failure: A Systematic Review and Meta-Analysis
Abstract
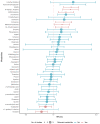
The associations of plasma metabolites with adverse cardiovascular (CV) outcomes are still underexplored and may be useful in CV risk stratification. We performed a systematic review and meta-analysis to establish correlations between blood metabolites and adverse CV outcomes in patients with heart failure (HF). Four cohorts were included, involving 83 metabolites and 37 metabolite ratios, measured in 1158 HF patients. Hazard ratios (HR) of 42 metabolites and 3 metabolite ratios, present in at least two studies, were combined through meta-analysis. Higher levels of histidine (HR 0.74, 95% CI [0.64; 0.86]) and tryptophan (HR 0.82 [0.71; 0.96]) seemed protective, whereas higher levels of symmetric dimethylarginine (SDMA) (HR 1.58 [1.30; 1.93]), N-methyl-1-histidine (HR 1.56 [1.27; 1.90]), SDMA/arginine (HR 1.38 [1.14; 1.68]), putrescine (HR 1.31 [1.06; 1.61]), methionine sulfoxide (HR 1.26 [1.03; 1.52]), and 5-hydroxylysine (HR 1.25 [1.05; 1.48]) were associated with a higher risk of CV events. Our findings corroborate important associations between metabolic imbalances and a higher risk of CV events in HF patients. However, the lack of standardization and data reporting hampered the comparison of a higher number of studies. In a future clinical scenario, metabolomics will greatly benefit from harmonizing sample handling, data analysis, reporting, and sharing.
Keywords: biomarkers; cardiovascular disease; heart failure; metabolomics; prognosis.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Effects of a gluten-reduced or gluten-free diet for the primary prevention of cardiovascular disease.Cochrane Database Syst Rev. 2022 Feb 24;2(2):CD013556. doi: 10.1002/14651858.CD013556.pub2. Cochrane Database Syst Rev. 2022. PMID: 35199850 Free PMC article.
-
Plasma metabolites associated with endometriosis in adolescents and young adults.Hum Reprod. 2025 May 1;40(5):843-854. doi: 10.1093/humrep/deaf040. Hum Reprod. 2025. PMID: 40107296
-
Beta-blockers in patients without heart failure after myocardial infarction.Cochrane Database Syst Rev. 2021 Nov 5;11(11):CD012565. doi: 10.1002/14651858.CD012565.pub2. Cochrane Database Syst Rev. 2021. PMID: 34739733 Free PMC article.
-
First-line drugs inhibiting the renin angiotensin system versus other first-line antihypertensive drug classes for hypertension.Cochrane Database Syst Rev. 2015 Jan 11;1:CD008170. doi: 10.1002/14651858.CD008170.pub2. Cochrane Database Syst Rev. 2015. Update in: Cochrane Database Syst Rev. 2018 Nov 14;11:CD008170. doi: 10.1002/14651858.CD008170.pub3. PMID: 25577154 Updated.
-
Dipeptidyl peptidase-4 inhibitors, glucagon-like peptide 1 receptor agonists and sodium-glucose co-transporter-2 inhibitors for people with cardiovascular disease: a network meta-analysis.Cochrane Database Syst Rev. 2021 Oct 25;10(10):CD013650. doi: 10.1002/14651858.CD013650.pub2. Cochrane Database Syst Rev. 2021. PMID: 34693515 Free PMC article.
Cited by
-
Dissecting causal networks of inflammatory factors and metabolites in heart failure: A mediation Mendelian randomization study.Medicine (Baltimore). 2025 Aug 8;104(32):e43801. doi: 10.1097/MD.0000000000043801. Medicine (Baltimore). 2025. PMID: 40797443 Free PMC article.
-
Nontargeted and targeted metabolic profile of metabolic syndrome patients: a study based on Yi and Han populations in Yunnan.Front Endocrinol (Lausanne). 2025 May 14;16:1488099. doi: 10.3389/fendo.2025.1488099. eCollection 2025. Front Endocrinol (Lausanne). 2025. PMID: 40438394 Free PMC article.
References
-
- Norhammar A., Bodegard J., Vanderheyden M., Tangri N., Karasik A., Maggioni A.P., Sveen K.A., Taveira-Gomes T., Botana M., Hunziker L., et al. Prevalence, Outcomes and Costs of a Contemporary, Multinational Population with Heart Failure. Heart. 2023;109:548–556. doi: 10.1136/heartjnl-2022-321702. - DOI - PMC - PubMed
-
- Tsutsui H., Albert N.M., Coats A.J.S., Anker S.D., Bayes-Genis A., Butler J., Chioncel O., Defilippi C.R., Drazner M.H., Felker G.M., et al. Natriuretic Peptides: Role in the Diagnosis and Management of Heart Failure: A Scientific Statement from the Heart Failure Association of the European Society of Cardiology, Heart Failure Society of America and Japanese Heart Failure Society. Eur. J. Heart Fail. 2023;25:616–631. doi: 10.1002/ejhf.2848. - DOI - PubMed
-
- Buchan T.A., Ching C., Foroutan F., Malik A., Daza J.F., Hing N.N.F., Siemieniuk R., Evaniew N., Orchanian-Cheff A., Ross H.J., et al. Prognostic Value of Natriuretic Peptides in Heart Failure: Systematic Review and Meta-Analysis. Heart Fail. Rev. 2022;27:645–654. doi: 10.1007/s10741-021-10136-3. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous