Lung Metastasectomy: Where Do We Stand? Results from an Italian Multicentric Prospective Database
- PMID: 38892816
- PMCID: PMC11172471
- DOI: 10.3390/jcm13113106
Lung Metastasectomy: Where Do We Stand? Results from an Italian Multicentric Prospective Database
Abstract
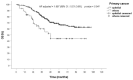
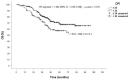
Background/Objectives: The surgical resection of pulmonary metastases is considered a therapeutic option in selected cases. In light of this, we present the results from a national multicenter prospective registry of lung metastasectomy. Methods: This retrospective analysis involves data collected prospectively and consecutively in a national multicentric Italian database, including patients who underwent lung metastasectomy. The primary endpoints were the analysis of morbidity and overall survival (OS), with secondary endpoints focusing on the analysis of potential risk factors affecting both morbidity and OS. Results: A total 470 lung procedures were performed (4 pneumonectomies, 46 lobectomies/bilobectomies, 13 segmentectomies and 407 wedge resections) on 461 patients (258 men and 203 women, mean age of 63.1 years). The majority of patients had metastases from colorectal cancer (45.8%). In most cases (63.6%), patients had only one lung metastasis. A minimally invasive approach was chosen in 143 cases (30.4%). The mean operative time was 118 min, with no reported deaths. Morbidity most frequently consisted of prolonged air leaking and bleeding, but no re-intervention was required. Statistical analysis revealed that morbidity was significantly affected by operative time and pulmonary comorbidities, while OS was significantly affected by disease-free interval (DFI) > 24 months (p = 0.005), epithelial histology (p = 0.001) and colorectal histology (p = 0.004) during univariate analysis. No significant correlation was found between OS and age, gender, surgical approach, surgical extent, surgical device, the number of resected metastases, lesion diameter, the site of lesions and nodal involvement. Multivariate analysis of OS confirmed that only epithelial histology and DFI were risk-factors, with p-values of 0.041 and 0.031, respectively. Conclusions: Lung metastasectomy appears to be a safe procedure, with acceptable morbidity, even with a minimally invasive approach. However, it remains a local treatment of a systemic disease. Therefore, careful attention should be paid to selecting patients who could truly benefit from surgical intervention.
Keywords: lung metastasis; lung surgery; metastasectomy; thoracic surgery.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Surgical Resection of Pulmonary Metastases from Melanoma in Oligometastatic Patients: Results from a Multicentric Study in the Era of Immunoncology and Targeted Therapy.Cancers (Basel). 2023 Apr 25;15(9):2462. doi: 10.3390/cancers15092462. Cancers (Basel). 2023. PMID: 37173927 Free PMC article.
-
Long-term results of percutaneous radiofrequency ablation of pulmonary metastases: a single institution experience.Interact Cardiovasc Thorac Surg. 2016 Jul;23(1):57-64. doi: 10.1093/icvts/ivw089. Epub 2016 Apr 7. Interact Cardiovasc Thorac Surg. 2016. PMID: 27059068 Free PMC article.
-
[Surgical therapy of pulmonary metastases of colorectal cancer--ten-year results].Rozhl Chir. 2012 Feb;91(2):81-6. Rozhl Chir. 2012. PMID: 22746086 Czech.
-
Impact of the extent of lung resection on postoperative outcomes of pulmonary metastasectomy for colorectal cancer metastases: an exploratory systematic review.J Thorac Dis. 2022 Jul;14(7):2677-2688. doi: 10.21037/jtd-22-239. J Thorac Dis. 2022. PMID: 35928602 Free PMC article. Review.
-
[Lung Metastasectomy in Pulmonary Metastatic Colorectal Carcinoma].Zentralbl Chir. 2018 Apr;143(2):193-204. doi: 10.1055/s-0043-114734. Epub 2017 Sep 25. Zentralbl Chir. 2018. PMID: 28946155 German.
Cited by
-
Reply to Treasure et al. Comment on "Ambrogi et al. Lung Metastasectomy: Where Do We Stand? Results from an Italian Multicentric Prospective Database. J. Clin. Med. 2024, 13, 3106".J Clin Med. 2024 Nov 27;13(23):7183. doi: 10.3390/jcm13237183. J Clin Med. 2024. PMID: 39685642 Free PMC article.
-
Comments on Ambrogi et al. Lung Metastasectomy: Where Do We Stand? Results from an Italian Multicentric Prospective Database. J. Clin. Med. 2024, 13, 3106.J Clin Med. 2024 Nov 26;13(23):7142. doi: 10.3390/jcm13237142. J Clin Med. 2024. PMID: 39685601 Free PMC article.
References
-
- Pastorino U., Buyse M., Friedel G., Ginsberg R.J., Girard P., Goldstraw P., Johnston M., McCormack P., Pass H., Putnam J.B., Jr. Long-term results of lung metastasectomy: Prognostic analyses based on 5206 cases. J. Thorac. Cardiovasc. Surg. 1997;113:37–49. doi: 10.1016/S0022-5223(97)70397-0. - DOI - PubMed
-
- Rolle A., Pereszlenyi A., Koch R., Richard M., Baier B. Is surgery for multiple lung metastases reasonable? A total of 328 consecutive patients with multiple-laser metastasectomies with a new 1318-nm Nd:YAG laser. J. Thorac. Cardiovasc. Surg. 2006;131:1236–1242. doi: 10.1016/j.jtcvs.2005.11.053. - DOI - PubMed
LinkOut - more resources
Full Text Sources