Bleeding Outcomes of Direct Oral Anticoagulants and Vitamin K Antagonists for Acute Venous Thromboembolism: A Cross-Sectional Study
- PMID: 38894767
- PMCID: PMC11185851
- DOI: 10.7759/cureus.60616
Bleeding Outcomes of Direct Oral Anticoagulants and Vitamin K Antagonists for Acute Venous Thromboembolism: A Cross-Sectional Study
Abstract
Background: Venous thromboembolism (VTE) is a widespread and significant cause of morbidity and mortality on a global scale. The primary objective of this cross-sectional study is to examine the impact of anticoagulant therapy on major organ hemorrhage events in patients diagnosed with acute venous thromboembolism (VTE). Specifically, this research compares the effects of vitamin K antagonists (VKAs) and direct oral anticoagulants (DOACs).
Materials and methods: This retrospective observational study examined the medical records of 46 patients who had been diagnosed with VTE and were receiving treatment with DOACs or VKAs. The documentation of patient characteristics encompassed demographic information, comorbidities, and treatment particulars. Within 30 days of hospital admission, the incidence of significant organ bleeding events, with an emphasis on gastrointestinal and intracranial hemorrhage, was the primary outcome evaluated.
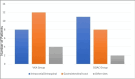
Results: Overall, 46 patients with VTE who were treated with oral anticoagulation therapy participated in the study. Twenty-four and 22 patients were administered VKAs and DOACs, respectively. The similarity in baseline characteristics between the DOAC and VKA groups ensured that the analyses were well-matched. The examination of bleeding sites unveiled subtle variations, as the DOAC group exhibited a progressive increase in the incidence of intracranial bleeding (12, 55.5%), while the VKA group demonstrated a surge in upper gastrointestinal bleeding (12, 50%) as well. While lacking statistical significance, these observed patterns are consistent with prior research that indicates that DOACs may have a lower risk of catastrophic hemorrhage in comparison to VKAs. The overall in-hospital mortality rate for patients treated with VKA was 33.3% (n=8), while that treated with DOAC was 18.2% (n=4). These differences did not reach statistical significance (P>0.05). In a similar vein, the evaluation of mortality associated with hemorrhage revealed six (25%) in the group receiving VKA and three (13.6%) in the group receiving DOAC; the P value was not statistically significant (P>0.05).
Conclusions: This study contributes valuable insights into bleeding outcomes associated with anticoagulant therapy for acute VTE. The nuanced differences in bleeding patterns highlight the complexity of anticoagulant selection, emphasizing the importance of considering bleeding site considerations. The comparable mortality rates support existing evidence regarding the favorable safety profile of DOACs.
Keywords: anticoagulants; doac; major organ bleeding; vka; vte.
Copyright © 2024, Javaid et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
-
- Venous thromboembolism research priorities: a scientific statement from the American Heart Association and the International Society on Thrombosis and Haemostasis. Cushman M, Barnes GD, Creager MA, et al. Circulation. 2020;142:0–94. - PubMed
-
- Trends in hospitalization and in-hospital mortality from VTE, 2007 to 2016, in China. Zhang Z, Lei J, Shao X, et al. Chest. 2019;155:342–353. - PubMed
-
- Antithrombotic management of venous thromboembolism: JACC focus seminar. Renner E, Barnes GD. J Am Coll Cardiol. 2020;76:2142–2154. - PubMed
-
- Trends in mortality related to pulmonary embolism in the European Region, 2000-15: analysis of vital registration data from the WHO Mortality Database. Barco S, Mahmoudpour SH, Valerio L, et al. Lancet Respir Med. 2020;8:277–287. - PubMed
LinkOut - more resources
Full Text Sources
