Nonalcoholic Fatty Liver Disease in Shift Workers and Its Effect on Peripheral Nerve Conduction: A Cross-Sectional Study
- PMID: 38899241
- PMCID: PMC11185990
- DOI: 10.7759/cureus.60632
Nonalcoholic Fatty Liver Disease in Shift Workers and Its Effect on Peripheral Nerve Conduction: A Cross-Sectional Study
Abstract
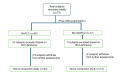
Introduction Nonalcoholic fatty liver disease (NAFLD) presents as a multisystem disorder, heightening the risk of developing type 2 diabetes mellitus (T2DM) and cardiovascular diseases (CVDs). Occupation emerges as a significant factor influencing the occurrence of NAFLD. Research indicates that individuals engaged in shift work face an elevated risk of NAFLD, alongside obesity and T2DM, attributed to disruptions in their circadian rhythm, which precipitate hepatic steatosis and inflammation. Remarkably, peripheral neuropathy has been observed in conjunction with advanced liver disorders and NAFLD in the general population. However, the correlation between NAFLD and peripheral neuropathy remains unestablished in shift workers. Objective To identify NAFLD in seemingly healthy rotating shift workers and assess any potential impact of NAFLD on nerve function in this demographic. Methods This cross-sectional study involved 73 apparently healthy nonalcoholic security guards (aged 35 to 60 years) working in rotating shifts. The study included a comprehensive assessment, beginning with a medical history, an evaluation of physical activity, and anthropometric measurements. Confirmation of NAFLD was achieved through abdominal ultrasonography (USG), followed by the analysis of biochemical parameters. Motor and sensory nerve conduction studies (NCS) were conducted on participants with normal vitamin B12 levels using the Aleron electromyograph (EMG) machine (Recorders and Medicare Systems Private Ltd, Budanpur, India). The evaluation encompassed the Median and Common Peroneal motor nerves, as well as Median and Sural sensory nerves. Recorded parameters for motor nerves included distal motor latency (DML), compound muscle action potential (CMAP) amplitude, conduction velocity (CV), and F-wave minimum latency (F-wave), while sensory nerve parameters comprised sensory onset latency (SOL), sensory nerve action potential (SNAP) amplitude, and CV. Results Among 73 healthy security guards working in rotating shifts, 76.1% were diagnosed with NAFLD through abdominal ultrasound. Following participant withdrawals and exclusions due to vitamin B12 deficiency, a comparison of NCS parameters between NAFLD (n=24) and Non-NAFLD (n=12) groups revealed no significant disparities in motor or sensory parameters, except for a slightly diminished CMAP amplitude in the peroneal nerve of NAFLD subjects (8.21±2.83mV vs ±10.22±2.30 mV, p< 0.040). However, these differences fell within normal ranges, indicating no notable impact on peripheral nerve conduction in the presence of NAFLD. Conclusion The results indicate a high prevalence of NAFLD among individuals working rotating shifts. Moreover, the investigation suggests that despite the presence of NAFLD, there is no discernible influence on motor and sensory peripheral nerve conduction, particularly in common peroneal, median, and sural nerves.
Keywords: metabolic disorder; nafld; nerve conduction study; peripheral nerves; shift workers.
Copyright © 2024, Chatur et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Repeatability of nerve conduction measurements derived entirely by computer methods.Biomed Eng Online. 2009 Nov 6;8:33. doi: 10.1186/1475-925X-8-33. Biomed Eng Online. 2009. PMID: 19895683 Free PMC article.
-
Repeatability of nerve conduction measurements using automation.J Clin Monit Comput. 2006 Dec;20(6):405-10. doi: 10.1007/s10877-006-9046-8. Epub 2006 Sep 14. J Clin Monit Comput. 2006. PMID: 16972142 Free PMC article.
-
[Subclinical lesions of peripheral nervous system in multiple sclerosis patients].Neurol Neurochir Pol. 2004 Jul-Aug;38(4):257-64. Neurol Neurochir Pol. 2004. PMID: 15383952 Polish.
-
Clinical and molecular genetic characteristics of 24 families of hereditary neuropathy with liability to pressure palsy and literature review.Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2023 Oct 28;48(10):1572-1582. doi: 10.11817/j.issn.1672-7347.2023.230116. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2023. PMID: 38432886 Free PMC article. Review. Chinese, English.
-
Effect of extracorporeal shock wave therapy on nerve conduction: a systematic review and meta-analysis.Front Neurol. 2024 Nov 22;15:1493692. doi: 10.3389/fneur.2024.1493692. eCollection 2024. Front Neurol. 2024. PMID: 39650239 Free PMC article.
Cited by
-
Night shift-induced circadian disruption: links to initiation of non-alcoholic fatty liver disease/non-alcoholic steatohepatitis and risk of hepatic cancer.Hepatoma Res. 2024 Oct 30:2394-5079.2024.88. doi: 10.20517/2394-5079.2024.88. Online ahead of print. Hepatoma Res. 2024. PMID: 39525867 Free PMC article.
References
-
- The global NAFLD epidemic. Loomba R, Sanyal AJ. Nat Rev Gastroenterol Hepatol. 2013;10:686–690. - PubMed
-
- Nonalcoholic fatty liver disease in India - a lot done, yet more required! Duseja A. Indian J Gastroenterol. 2010;29:217–225. - PubMed
-
- 2019 global NAFLD prevalence: a systematic review and meta-analysis. Le MH, Yeo YH, Li X, et al. Clin Gastroenterol Hepatol. 2022;20:2809–2817. - PubMed
-
- Global prevalence, incidence, and outcomes of non-obese or lean non-alcoholic fatty liver disease: a systematic review and meta-analysis. Ye Q, Zou B, Yeo YH, et al. Lancet Gastroenterol Hepatol. 2020;5:739–752. - PubMed
LinkOut - more resources
Full Text Sources