Burden of Herpes Zoster Among Patients with Psoriatic Arthritis in the United States
- PMID: 38939905
- PMCID: PMC11208162
- DOI: 10.2147/PTT.S430151
Burden of Herpes Zoster Among Patients with Psoriatic Arthritis in the United States
Abstract
Purpose: Patients with psoriasis (PsO) and psoriatic arthritis (PsA) are at increased risk of herpes zoster (HZ), but healthcare resource use (HRU) and costs relating to HZ in adults with PsA are unknown. We aimed to estimate the incidence of HZ among adults with PsA vs without psoriatic disease and the additional HRU and costs among patients with PsA with vs without HZ.
Patients and methods: This retrospective, longitudinal, cohort study estimated HZ incidence in PsA+ vs PsO-/PsA- cohorts and HRU and medical/pharmacy costs among PsA+/HZ+ vs PsA+/HZ- cohorts comprised of adults from Optum's de-identified Clinformatics Data Mart Database during 2015-2020. For the HRU/cost analyses, index was the date of first HZ diagnosis (PsA+/HZ+ cohort) or was randomly assigned (PsA+/HZ- cohort). Generalized linear models were used for adjusted comparisons between cohorts.
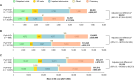
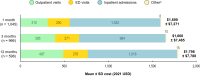
Results: HZ incidence was higher in the PsA+ (n = 57,126) vs PsO-/PsA- (n = 23,837,237) cohort (14.85 vs 7.67 per 1000 person-years; adjusted incidence rate ratio [aIRR]: 1.23; 95% confidence interval [CI]: 1.16-1.30). Numbers of outpatient visits, emergency department visits, and inpatient admissions were significantly higher in the PsA+/HZ+ (n = 1045) vs PsA+/HZ- (n = 36,091) cohorts during the first month after HZ diagnosis (outpatient: aIRR: 1.74; 95% CI: 1.63-1.86; emergency department: 3.14; 95% CI: 2.46-4.02; inpatient: aIRR: 2.61; 95% CI: 1.89-3.61). Mean all-cause per-patient costs were significantly higher in the PsA+/HZ+ vs PsA+/HZ- cohorts during the first month after index ($6493 vs $4521; adjusted cost difference: $2012; 95% CI: $1204-$3007). HRU and costs were numerically higher in the PsA+/HZ+ cohort during the first 3 and 12 months.
Conclusion: These findings, which provide evidence on the increased incidence and HRU and economic burden associated with HZ among adults with PsA, could be used to inform clinical practice and decision-making.
Keywords: United States; claims database; costs; healthcare resource use; incidence; psoriatic arthritis.
Plain language summary
Why was the study done? Psoriatic arthritis affects the joints of around 20% of patients with the skin condition, psoriasis.Patients with psoriatic arthritis are at increased risk of shingles, which can cause a painful skin rash and complications.This study aimed to provide information on how many patients with psoriatic arthritis get shingles and the healthcare use and costs of caring for patients with psoriatic arthritis and shingles. What did the researchers do and find? Using data from a large US health plan database, we estimated that for every 1000 patients with psoriatic arthritis observed for 1 year, 15 will develop shingles.Patients with psoriatic arthritis were 23% more likely to develop shingles than people without psoriatic disease.Patients with psoriatic arthritis and shingles had 2–3 times as many healthcare visits in the month after a shingles diagnosis as patients with psoriatic arthritis but no shingles.This resulted in an average additional cost of approximately $2000 per patient. What do these results mean? Psoriatic arthritis increases the risk of shingles.The costs associated with shingles in patients with psoriatic arthritis are substantial.Measures to prevent shingles in this population could be beneficial.
© 2024 GSK.
Conflict of interest statement
David Singer, Nikita Stempniewicz, and Sara Poston are employees of, and hold financial equities in, GSK. Philippe Thompson-Leduc, Deepshekhar Gupta, Wendy Y. Cheng, Selvam R. Sendhil, Manasvi Sundar, Ella Hagopian, and Mei Sheng Duh are employees of Analysis Group, Inc., a consulting firm that has received funding from GSK for the conduct of this study. Siyu Ma declares to have received postdoctoral fellowship grant from GSK during the conduct of the study. The authors declare no other financial and non-financial relationships and activities for this work.
Figures




Similar articles
-
Burden of Herpes Zoster Among Patients with Psoriasis in the United States.Dermatol Ther (Heidelb). 2023 Nov;13(11):2649-2668. doi: 10.1007/s13555-023-00988-y. Epub 2023 Sep 22. Dermatol Ther (Heidelb). 2023. PMID: 37740149 Free PMC article.
-
Increased Health Care Resource Utilization and Costs Associated with Herpes Zoster Among Patients Aged ≥50 Years with Chronic Obstructive Pulmonary Disease in the United States.Chronic Obstr Pulm Dis. 2021 Oct 28;8(4):502-516. doi: 10.15326/jcopdf.2021.0222. Chronic Obstr Pulm Dis. 2021. PMID: 34614552 Free PMC article.
-
Herpes zoster burden in patients with asthma: real-world incidence, healthcare resource utilisation and cost.BMJ Open Respir Res. 2024 Jun 11;11(1):e002130. doi: 10.1136/bmjresp-2023-002130. BMJ Open Respir Res. 2024. PMID: 38862238 Free PMC article.
-
A systematic review of herpes zoster incidence and consensus recommendations on vaccination in adult patients on systemic therapy for psoriasis or psoriatic arthritis: From the Medical Board of the National Psoriasis Foundation.J Am Acad Dermatol. 2019 Jul;81(1):102-110. doi: 10.1016/j.jaad.2019.03.017. Epub 2019 Mar 15. J Am Acad Dermatol. 2019. PMID: 30885757
-
Herpes Zoster Recurrence: A Narrative Review of the Literature.Dermatol Ther (Heidelb). 2024 Mar;14(3):569-592. doi: 10.1007/s13555-024-01101-7. Epub 2024 Feb 28. Dermatol Ther (Heidelb). 2024. PMID: 38416279 Free PMC article. Review.
References
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

