Surgical Strategy for Lumbar Disc Herniation based on the MSU Classification: Percutaneous Endoscopic Lumbar Discectomy versus Transforaminal Lumbar Interbody Fusion: A 5-year Retrospective Study
- PMID: 38961670
- PMCID: PMC11293921
- DOI: 10.1111/os.14145
Surgical Strategy for Lumbar Disc Herniation based on the MSU Classification: Percutaneous Endoscopic Lumbar Discectomy versus Transforaminal Lumbar Interbody Fusion: A 5-year Retrospective Study
Abstract
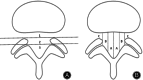
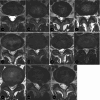
Objective: Currently, there is no established guideline on whether to opt for percutaneous endoscopic lumbar discectomy (PELD) or traditional transforaminal lumbar interbody fusion (TLIF) surgery based on specific types of lumbar disc herniation (LDH). Based on the Michigan State University (MSU) classification system, this study conducted a medium- to long-term follow-up analysis of two surgical methods over 5 years for the first time, aiming to provide empirical evidence to assist in making more informed decisions before surgery for LDH treatment.
Methods: This was a retrospective study that included 273 patients with single-level LDH who underwent PELD or TLIF treatment at our hospital between January 1, 2016, and December 31, 2018. Detailed metrics included preoperative and postoperative visual analogue scale (VAS) scores and Oswestry disability index (ODI) at 1-day, 1-week, 1-year, and 5-year follow-ups. Complications, recurrences, and 5-year postoperative modified MacNab criteria scores were also recorded. Statistical methods included independent sample t-tests, repeated measures analysis of variance (ANOVA), and χ2 tests.
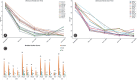
Results: Classified into seven groups according to the MSU classification, it was found that there was an improvement in the VAS and ODI scores at four postoperative follow-ups (p < 0.001). PELD showed better results than TLIF in reducing pain and improving the ODI scores in the classifications of 3B, 2B, and 2C (p < 0.05). TLIF demonstrated consistent superiority over PELD in 2A, 2AB, 3A, and 3AB classifications (p < 0.05). The total recurrence rate in the PELD group (11.05%) within 5 years after surgery was higher (p < 0.05) than that in the TLIF group (3.96%). These were mainly concentrated in the 2A, 2AB, 3A, and 3AB types. Moreover, the rate of excellent and good outcomes in the PELD was higher than in the TLIF but no significant difference (χ2 = 1.0568, p = 0.5895).
Conclusion: This study suggests that PELD and TLIF may relieve LDH, but have advantages under different MSU classifications. The MSU classification has specific guiding significance and could aid in the surgical selection of PELD or TLIF to achieve optimal treatment outcomes for patients with lumbar disc herniation.
Keywords: Lumbar disc herniation; MSU classification; PELD; Retrospective study; TLIF.
© 2024 The Author(s). Orthopaedic Surgery published by Tianjin Hospital and John Wiley & Sons Australia, Ltd.
Conflict of interest statement
The authors report no conflicts of interest.
Figures

References
-
- Al Qaraghli MI, De Jesus O. Lumbar disc herniation. StatPearls. Treasure Island, FL: StatPearls Publishing; 2023. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

