Drug-Drug Interactions Involving High-Alert Medications that Lead to Interaction-Associated Symptoms in Pediatric Intensive Care Patients: A Retrospective Study
- PMID: 38963501
- PMCID: PMC11335839
- DOI: 10.1007/s40272-024-00641-x
Drug-Drug Interactions Involving High-Alert Medications that Lead to Interaction-Associated Symptoms in Pediatric Intensive Care Patients: A Retrospective Study
Abstract
Background: Children treated in a pediatric intensive care unit (PICU) often receive several drugs together, among them drugs defined as high-alert medications (HAMs). Those drugs carry a high risk of causing patient harm, for example, due to a higher potential for interactions. HAMs should therefore be administered with caution, especially in a PICU.
Objectives: The objective of the current study was to identify drug-drug interactions involving HAMs that increase the risk of interaction-associated symptoms in pediatric intensive care.
Methods: In a retrospective study, we analyzed the electronic documentation of patients hospitalized for at least 48 h in a general PICU who received at least two different drugs within a 24-h interval. We assessed potential drug-drug interactions involving HAM on the basis of the two drug information databases UpToDate and drugs.com. Furthermore, we analyzed whether symptoms were observed after the administration of drug pairs that could lead to interaction-associated symptoms. For drug pairs involving HAM administered on at least 2% of patient days, and symptoms observed at least ten times after a respective drug pair, we calculated odds ratios, 95% confidence intervals, and p-values by using a univariate binary logistic regression.
Results: Among 315 analyzed patients, 81.3% (256/315) received drugs defined as high-alert medication for pediatric patients. Those high-alert medications were involved in 20,150 potential drug-drug interactions. In 14.0% (2830/20,150) of these, one or more symptoms were observed that could be a possible consequence of the interaction, resulting in 3203 observed symptoms affecting 56.3% (144/256) of patients receiving high-alert medication. The odds ratios for symptoms observed after a drug-drug interaction were increased for eight specific symptoms (each p ≤ 0.05), especially hemodynamic alterations and disturbances of electrolyte and fluid balance. The odds ratio was highest for decreased blood pressure observed after the administration of the drug pair fentanyl and furosemide (OR 5.06; 95% confidence interval 3.5-7.4; p < 0.001). Increased odds ratios for specific symptoms observed after drug-drug interactions resulted from eight combinations composed of eight different drugs: digoxin, fentanyl, midazolam, phenobarbital, potassium salts and vancomycin (high-alert medications), and the diuretics furosemide and hydrochlorothiazide (non-high-alert medications). The resulting drug pairs were: potassium salts-furosemide, fentanyl-furosemide, vancomycin-furosemide, digoxin-furosemide, digoxin-hydrochlorothiazide, fentanyl-phenobarbital, potassium salts-hydrochlorothiazide, and midazolam-hydrochlorothiazide.
Conclusions: In a cohort of PICU patients, this study identified eight specific drug pairs involving high-alert medications that may increase the risk of interaction-associated symptoms, mainly hemodynamic alterations and electrolyte/fluid balance disturbances. If the administration of those drug pairs is unavoidable, patients should be closely monitored.
© 2024. The Author(s).
Conflict of interest statement
A. Bertsche reports grants from UCB Pharma GmbH and honoraria for speaking engagements from Biogen GmbH, Desitin Arzneimittel GmbH, Eisai GmbH, GW Pharma GmbH, Neuraxpharm GmbH, Shire/Takeda GmbH, UCB Pharma GmbH, and ViroPharma GmbH. The other authors declare they have no conflicts of interests.
Figures

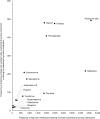
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

